Endocrinology — Flashcards

On this page
Secondary sexual characters appear normal in the following: No answer _____

Diagnosis of parathyroid disease summary: no answer _____
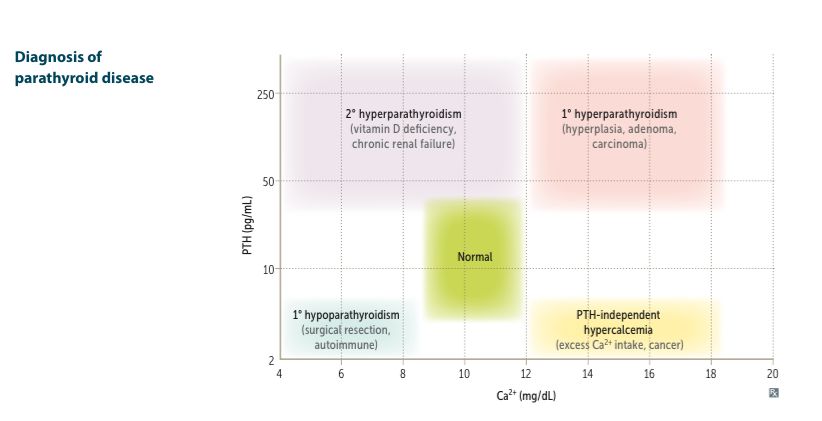
1. Identify → _____ 2. Use → _____
Growth hormone secreting pituitary adenoma causes _____ (adults) or gigantism (children)
In treating SIADH, _____tonic saline is given when treating a patient with severe symptoms, and isotonic saline is given for mild symptoms
A defective androgen receptor presents with _____ testosterone and increased LH
_____ is the most common cause of isolated elevated alkaline phosphatase in patients > 40 years old
Congenital adrenal hyperplasia is a result of decreased levels of _____, causing increased ACTH secretion via negative feedback
Thyroid, Pituitary, & Adrenal _____ may be used to treat acromegaly and gigantism if symptoms persist after trans-sphenoidal resection
_____ diabetes insipidus is characterized by polyuria and polydipsia with an inability to concentrate urine due to lack of ADH
Study by Chapter
Diabetes Mellitus
Flashcards
Thyroid Disorders
Flashcards
Adrenal Gland Disorders
Flashcards
Pituitary Disorders
Flashcards
Calcium and Bone Metabolism
Flashcards
Reproductive Endocrinology
Flashcards
Lipid Disorders
Flashcards
Endocrine Hypertension
Flashcards
Multiple Endocrine Neoplasia
Flashcards
Obesity and Metabolic Syndrome
Flashcards
Neuroendocrine Tumors
Flashcards
Endocrine Emergencies
Flashcards
About Endocrinology Flashcards for NEET-PG
These Endocrinology flashcards are designed for NEET-PG Internal Medicine preparation, using active recall to help you retain high-yield concepts, clinical correlations, and commonly tested facts. Each card prompts you to retrieve information from memory rather than passively reviewing notes, which research shows leads to significantly better exam performance.
The 207 cards in this deck cover the most important topics in Endocrinology, including key mechanisms, diagnostic criteria, treatment protocols, and clinical pearls that frequently appear in NEET-PG examinations. Cards are organised by chapter so you can focus on specific areas or work through the entire topic systematically.
For personalised spaced repetition scheduling that adapts to your performance, unlimited flashcards, and detailed progress analytics, download the Oncourse app.
Frequently Asked Questions
Are Endocrinology flashcards free on Oncourse?
How do flashcards help with NEET-PG preparation?
How many Endocrinology flashcards are available?
Can I study Endocrinology flashcards by chapter?
What topics do these Internal Medicine flashcards cover?
Want unlimited flashcards?
Get full access to all flashcards, spaced repetition, and progress tracking.
Start For Free