Back
USMLE Step 1 Pharmacology: High-Yield Drug Classes, Mechanisms and Exam Strategy (2026)
Master USMLE Step 1 pharmacology with high-yield drug classes, mechanisms, and proven exam strategies. Complete guide covering cardiovascular, antibiotics, CNS, endocrine drugs and more for 2026.

USMLE Step 1 Pharmacology: High-Yield Drug Classes, Mechanisms and Exam Strategy (2026)
You are probably staring at a pharmacology textbook right now, wondering how you'll memorize 3,000+ drugs for Step 1. Here's the truth: you dont need to memorize them all. Step 1 pharmacology tests mechanism understanding and clinical application — not drug name recall.
Step 1 has roughly 50-70 pharmacology questions spread across all systems. That's 20-30% of your score. The students who crush pharmacology dont memorize every side effect. They master 6 high-yield drug classes that appear in 80% of questions. They connect mechanisms to pathophysiology. They can predict side effects from first principles.
If you have ever felt overwhelmed by the sheer volume of pharmacology, this guide breaks down exactly what matters for Step 1. No fluff, no low-yield rabbit holes — just the drug classes, mechanisms, and strategy that separates 230s from 250s.
Why Step 1 Pharmacology Feels Overwhelming (And How to Fix It)
Most students approach pharmacology wrong. They study individual drugs in isolation. Propranolol. Atenolol. Metoprolol. Esmolol. Suddenly they have 20 beta-blockers with slightly different properties and their brain shuts down.
Here's what works: study by drug class and mechanism, not individual drugs. Once you understand beta-adrenergic receptor blockade, you can predict the effects of any beta-blocker. The specifics (cardioselective vs non-selective, half-life differences) become details, not separate facts to memorize.
Step 1 tests three things in pharmacology:
1. Mechanism of action — How does the drug work at the molecular level?
2. Predictable side effects — What happens when you block this pathway?
3. Clinical application — When do you use this drug class?
Master these three elements for the high-yield drug classes, and you'll recognize the pattern in 90% of pharmacology questions.
The 6 High-Yield Drug Classes That Dominate Step 1
1. Autonomic Pharmacology: Alpha/Beta Agonists and Blockers
This is your foundation. The autonomic nervous system affects every organ, so these drugs appear in cardiovascular, respiratory, endocrine, and psychiatric questions.
Key mechanism concepts:
Alpha-1 blockers (prazosin, terazosin): vasodilation → hypotension, but also smooth muscle relaxation in prostate
Beta-1 blockers (metoprolol, atenolol): decreased heart rate and contractility → bradycardia, fatigue
Beta-2 agonists (albuterol): bronchodilation and vasodilation → tremor, tachycardia
Non-selective beta blockers (propranolol): blocks both beta-1 and beta-2 → can trigger asthma
The pattern: know which receptors are where (heart = beta-1, lungs = beta-2, vessels = alpha-1), and you can predict any drug's effects.
Step 1 loves testing: Beta-blocker contraindications (asthma, diabetes), alpha-blocker first-dose hypotension, and choosing cardioselective vs non-selective agents.
Practice these concepts with targeted USMLE cardiovascular pharmacology questions to solidify the receptor-based thinking.
2. Cardiovascular Drugs: The Big Four Classes
Cardiovascular pharmacology shows up everywhere — in cardiology blocks, nephrology cases, even emergency medicine scenarios.
ACE Inhibitors vs ARBs:
ACE inhibitors (lisinopril, enalapril): block conversion of angiotensin I → II, but also decrease bradykinin breakdown → dry cough
ARBs (losartan, valsartan): block angiotensin II receptor directly → no cough, but same therapeutic effects
This is where mechanisms save you time. Students often ask 'explain the mechanism of action of ACE inhibitors vs ARBs' when reviewing cases — rather than memorizing two separate pathways, understanding the RAAS system lets you derive both mechanisms using Rezzy's lesson chat feature. Statins (atorvastatin, simvastatin):
Mechanism: HMG-CoA reductase inhibition → decreased cholesterol synthesis
Side effects: Myopathy (watch CK levels), hepatotoxicity (monitor LFTs)
Key point: The myopathy risk increases with CYP3A4 inhibitors (grapefruit juice, macrolides)
Antiarrhythmics — Learn by mechanism, not by drug:
Class I: Sodium channel blockers → prolonged QRS
Class II: Beta blockers → bradycardia
Class III: Potassium channel blockers (amiodarone) → prolonged QT
Class IV: Calcium channel blockers → bradycardia, hypotension
Master these four classes through our comprehensive ACE inhibitor lessons, and you'll handle most cardiovascular pharmacology questions.
3. Antibiotics: Mechanisms, Coverage, and Resistance Patterns
Antibiotics account for 10-15 Step 1 questions, but the approach is mechanism-heavy. Dont memorize which bacteria each drug covers — understand how the mechanism determines coverage.
Beta-lactams (penicillins, cephalosporins, carbapenems):
Mechanism: Inhibit cell wall synthesis by binding PBPs
Resistance: Beta-lactamase production (bacteria make enzymes that destroy the drug)
Coverage pattern: Gram-positive > Gram-negative (with exceptions)
For complex beta-lactam mechanisms like PBP binding and resistance patterns, AI-generated mnemonic chains help lock in the pathways in one pass.
Aminoglycosides (gentamicin, streptomycin):
Mechanism: 30S ribosomal subunit inhibition → bactericidal
Toxicity: Nephrotoxicity and ototoxicity (both dose-dependent)
Coverage: Gram-negative aerobes (need oxygen for drug uptake)
Fluoroquinolones (ciprofloxacin, levofloxacin):
Mechanism: DNA gyrase inhibition → can't supercoil DNA
Resistance: Mutations in DNA gyrase gene
Side effects: Tendon rupture, QT prolongation
Macrolides (azithromycin, clarithromycin):
Mechanism: 50S ribosomal subunit → bacteriostatic
Key interactions: CYP3A4 inhibition (especially clarithromycin)
Study these systematically through beta-lactam antibiotic lessons and aminoglycoside mechanisms.
4. CNS Pharmacology: Antidepressants, Antipsychotics, and Antiepileptics
CNS drugs are mechanism-heavy with predictable side effect patterns. The key is understanding which neurotransmitter systems each class affects.
Antidepressants:
SSRIs (fluoxetine, sertraline): Block serotonin reuptake → GI effects, sexual dysfunction
SNRIs (venlafaxine): Block serotonin + norepinephrine → hypertension
TCAs (amitriptyline): Block serotonin/NE + anticholinergic effects → dry mouth, constipation, urinary retention
Antipsychotics:
Typical (haloperidol): D2 receptor blockade → extrapyramidal symptoms
Atypical (risperidone, olanzapine): D2 + 5-HT2A → weight gain, metabolic effects
Antiepileptics — Study by mechanism:
Sodium channel blockers (phenytoin, carbamazepine): stabilize inactive state
GABA enhancers (valproate, benzodiazepines): increase inhibition
Calcium channel blockers (ethosuximide): T-type channels in thalamus
Strengthen your CNS pharmacology foundation with comprehensive antiepileptic drug lessons.
5. Endocrine Pharmacology: Diabetes and Thyroid Drugs
Endocrine pharmacology is high-yield because diabetes and thyroid disorders appear across multiple systems.
Diabetes medications:
Insulin: Know the kinetics — rapid (lispro), short (regular), intermediate (NPH), long (glargine)
Sulfonylureas (glyburide): Close K+ channels in pancreatic beta cells → hypoglycemia risk
Metformin: Decreases hepatic glucose output → lactic acidosis (rare but testable)
DPP-4 inhibitors (sitagliptin): Prevent GLP-1 breakdown → weight neutral
Thyroid drugs:
Levothyroxine: T4 replacement → takes 6-8 weeks for steady state
Methimazole: Inhibits thyroid peroxidase → can cause agranulocytosis
Propranolol: Beta-blocker for symptomatic hyperthyroidism
Using spaced repetition flashcards for high-volume drug lists prioritizes cards you keep missing, so you spend time where it counts. Master the mechanisms with endocrine pharmacology lessons.
6. Antineoplastics: Cell-Cycle Specific vs Non-Specific
Cancer pharmacology appears in 5-8 Step 1 questions, always testing mechanism and major toxicities.
Cell-cycle specific drugs:
Antimetabolites (5-FU, methotrexate): S phase → bone marrow suppression
Alkylating agents (cyclophosphamide): G0 phase → hemorrhagic cystitis
Mitotic inhibitors (vincristine): M phase → peripheral neuropathy
Key toxicity patterns:
Doxorubicin: Dilated cardiomyopathy (dose-dependent)
Bleomycin: Pulmonary fibrosis
Cisplatin: Nephrotoxicity and ototoxicity
The pattern: mechanism determines both efficacy and toxicity. Understand how each drug class kills cancer cells, and the side effects follow logically.
Study these systematically through antineoplastic drug management lessons.
High-Yield Study Strategy for Step 1 Pharmacology
Phase 1: Build Your Foundation (Weeks 1-2)
Start with autonomic pharmacology. This creates the framework for everything else. Spend 2 weeks understanding:
Receptor types and locations
Agonist vs antagonist effects
How to predict side effects from mechanism
Use the UFAP approach (UWorld, First Aid, Pathoma), but add active recall. After reading about beta-blockers, close the book and draw the mechanism from memory.
Phase 2: Master the Big Six (Weeks 3-8)
Work through each high-yield drug class systematically. Spend 1 week per class:
Day 1-2: Learn mechanisms
Day 3-4: Practice questions
Day 5-6: Focus on side effects and contraindications
Day 7: Review and flashcards
For each drug class, create mechanism maps. Draw how the drug works, where it acts, and what happens when you block that pathway.
Phase 3: Integration and Question Practice (Weeks 9-12)
Now connect pharmacology to pathophysiology. Step 1 rarely asks "What is the mechanism of propranolol?" Instead: "A patient with hyperthyroidism is started on propranolol. What is the most likely mechanism for symptom improvement?"
Practice integration through:
System-based question blocks
Mixed pharmacology questions
Timed practice to simulate exam conditions
The Power of Active Recall in Pharmacology
Passive reading kills pharmacology retention. Your brain thinks it "knows" ACE inhibitor mechanisms after reading about them, but can you explain the pathway without looking?
Effective active recall techniques: 1. Mechanism sketching: Draw drug pathways from memory 2. Question prediction: After learning a mechanism, predict what Step 1 would ask 3. Teaching moments: Explain drug classes to study partners 4. Flashcard cycling: Review weak drugs more frequently
The goal isnt to memorize — its to understand so deeply that you can derive answers during the exam.
Step 1 Pharmacology Question Patterns
Pattern 1: Mechanism-Based Side Effects
Question type: "A 65-year-old man develops a dry cough after starting antihypertensive therapy. What is the most likely mechanism?" Answer approach: Think about which drug classes cause cough (ACE inhibitors) and why (bradykinin accumulation).
Pattern 2: Drug Class Selection
Question type: "A patient with asthma and hypertension needs cardiovascular medication. Which drug should be avoided?" Answer approach: Non-selective beta-blockers (propranolol) can trigger bronchospasm in asthmatics.
Pattern 3: Interaction Predictions
Question type: "A patient on warfarin is prescribed azithromycin. What effect is expected?" Answer approach: Macrolides inhibit CYP3A4 → increased warfarin levels → bleeding risk.
Pattern 4: Resistance Mechanisms
Question type: "A bacteria produces extended-spectrum beta-lactamase. Which antibiotic would be most effective?" Answer approach: ESBLs destroy penicillins and cephalosporins, but not carbapenems.
Study these patterns through comprehensive pharmacology questions that mirror actual Step 1 format.
Common Pharmacology Mistakes on Step 1
Mistake 1: Memorizing Without Understanding
Students memorize "ACE inhibitors cause cough" without understanding why. When Step 1 asks about bradykinin, they're lost.
Fix: Always learn the mechanism first, then the clinical facts follow naturally.
Mistake 2: Ignoring Drug Interactions
Pharmacokinetic interactions account for 10-15% of pharmacology questions. Students focus on individual drugs and miss the CYP enzyme systems.
Fix: Learn major CYP inhibitors (grapefruit, macrolides) and inducers (rifampin, phenytoin).
Mistake 3: Weak on Contraindications
Step 1 loves asking when NOT to use a drug. Students know indications but miss contraindications.
Fix: For each drug class, memorize absolute contraindications. Beta-blockers in asthma. ACE inhibitors in pregnancy. Metformin in kidney disease.
Mistake 4: Poor Side Effect Prediction
Students memorize side effect lists instead of understanding mechanism-based toxicities.
Fix: Connect side effects to mechanism. Anticholinergic drugs cause dry mouth, constipation, and urinary retention because they block all muscarinic receptors.
Creating Your Pharmacology Study Schedule
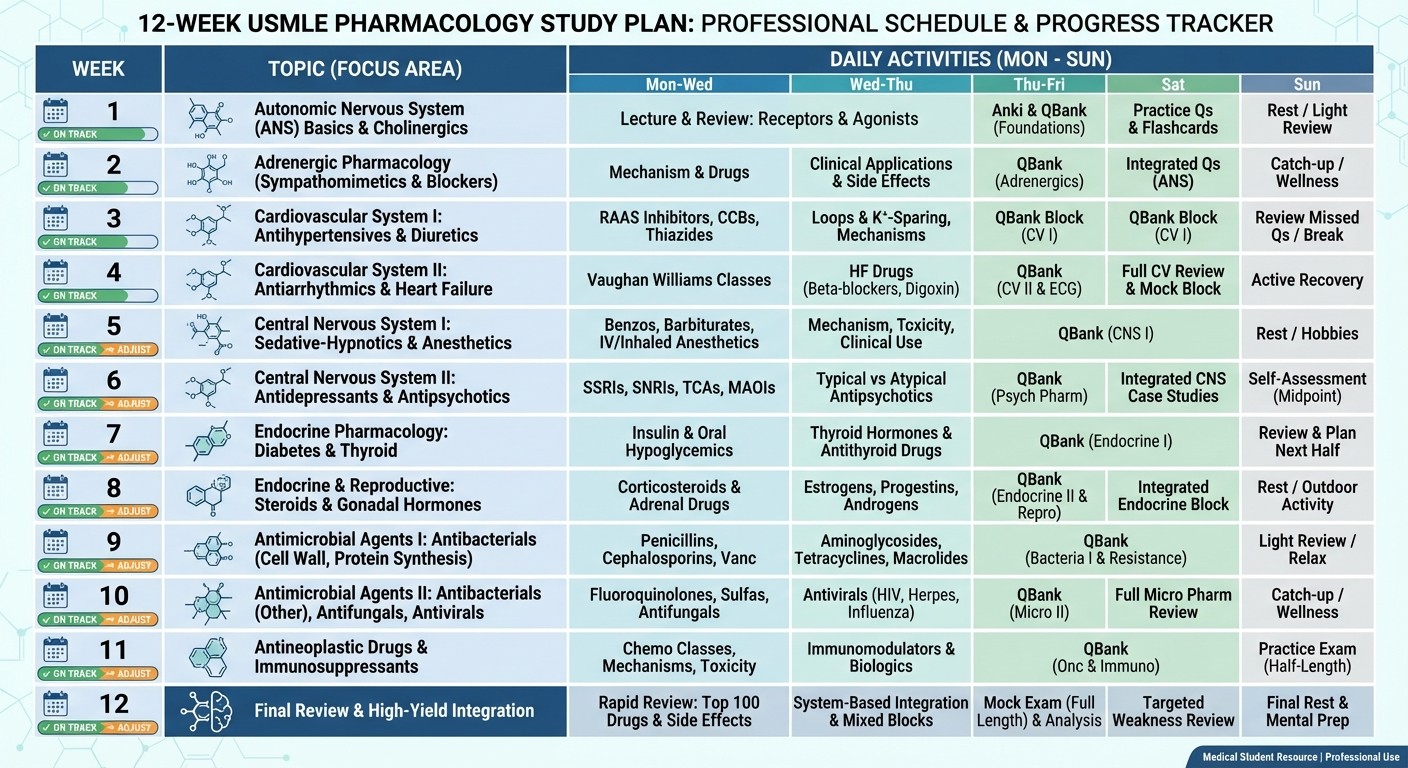
Weeks 1-2: Foundation Building
Week 1: Autonomic pharmacology (alpha/beta systems)
Week 2: Basic pharmacokinetics and drug interactions
Weeks 3-8: High-Yield Drug Classes
Week 3: Cardiovascular drugs (ACE-I, ARBs, beta-blockers)
Week 4: Antibiotics Part 1 (beta-lactams, aminoglycosides)
Week 5: Antibiotics Part 2 (fluoroquinolones, macrolides)
Week 6: CNS drugs (antidepressants, antipsychotics)
Week 7: Endocrine drugs (diabetes, thyroid)
Week 8: Antineoplastics and other high-yield classes
Weeks 9-12: Integration and Review
Week 9: System integration (cardio + renal pharmacology)
Week 10: Mixed question blocks and weak areas
Week 11: High-yield review and flashcards
Week 12: Final review and exam simulation
Advanced Pharmacology Concepts for Step 1
Understanding Pharmacokinetics vs Pharmacodynamics
Pharmacokinetics (what the body does to the drug):
Absorption: First-pass metabolism, bioavailability
Distribution: Protein binding, volume of distribution
Metabolism: CYP enzymes, Phase I vs Phase II
Elimination: Renal vs hepatic clearance
Pharmacodynamics (what the drug does to the body):
Receptor binding: Agonists, antagonists, partial agonists
Dose-response curves: EC50, therapeutic window
Drug interactions: Competitive vs non-competitive
CYP Enzyme Systems: High-Yield for Step 1
The major CYP enzymes appear in 15-20 Step 1 questions, usually as drug interaction scenarios.
CYP3A4 (most important):
Substrates: Statins, calcium channel blockers, many others
Inhibitors: Grapefruit juice, azole antifungals, macrolides
Inducers: Rifampin, phenytoin, St. Johns wort
Clinical relevance: Patient on atorvastatin + clarithromycin → increased statin levels → myopathy risk.
Practice CYP interactions through pharmacokinetic mechanism questions.
Frequently Asked Questions
How much time should I spend on pharmacology for Step 1?
Dedicate 25-30% of your study time to pharmacology. For a 12-week study period, that's 3-4 weeks of focused pharmacology study, spread throughout your prep.
Should I memorize every drug name and dosage?
No. Step 1 rarely asks about specific dosages. Focus on drug classes, mechanisms, major side effects, and contraindications. Generic names are more important than brand names.
How do I remember all the drug interactions?
Dont memorize individual interactions. Learn the major CYP enzyme systems (especially CYP3A4) and which drugs inhibit or induce them. This lets you predict most clinically relevant interactions.
What's the best resource for Step 1 pharmacology?
Use a combination approach: First Aid for high-yield facts, UWorld for application practice, and comprehensive pharmacology lessons for mechanism understanding. Avoid relying on any single source.
How important are pharmacology calculations on Step 1?
Minimal. Step 1 focuses on conceptual understanding rather than calculations. You might see basic clearance or half-life concepts, but complex math is rare.
Should I study toxicology separately from pharmacology?
No. Integrate toxicology with pharmacology. Most "toxicology" questions are actually mechanism-based side effects of therapeutic drugs. Understanding why acetaminophen causes hepatotoxicity is more valuable than memorizing antidotes.
---
Prepare smarter with Oncourse AI — adaptive MCQs, spaced repetition, and AI explanations built for USMLE Step 1. Download free on Android and iOS.