Anatomy
1 questionsTrigone of urinary bladder develops from:
Forensic Medicine
1 questionsDuring a postmortem examination of a young adult found with a faded tattoo, relatives mentioned that the tattoo was once visible. What is the best method to identify the tattoo?
Internal Medicine
2 questionsA 50 year old male presents with fever and malaise for 4 months and pain in the knees and ankles. Blood tests are normal apart from a raised ESR. Chest x-ray shows bilateral hilar adenopathy and pulmonary infiltrates most severe in the upper and mid zones. Mantoux test is negative. What is the most likely diagnosis?
Which of the following syndromes is least likely to be associated with obesity?
Microbiology
1 questionsNeutralization test is
Obstetrics and Gynecology
1 questionsWhich of the following describes the points marked in the diagram of pelvic measurements?
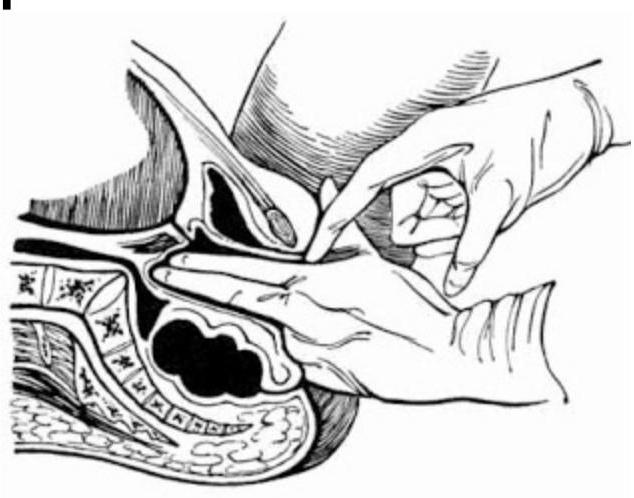
Pediatrics
1 questionsWhich of the following is not a known cause of neuroregression in children?
Pharmacology
2 questionsWhat is the mechanism of action of duloxetine?
Which of the following is the only clinically available depolarizing muscle relaxant?
Radiology
1 questionsEpidural hematoma on CT scan shows which of the following?