Obstetrics and Gynecology
1 questionsWhich of the following describes the points marked in the diagram of pelvic measurements?
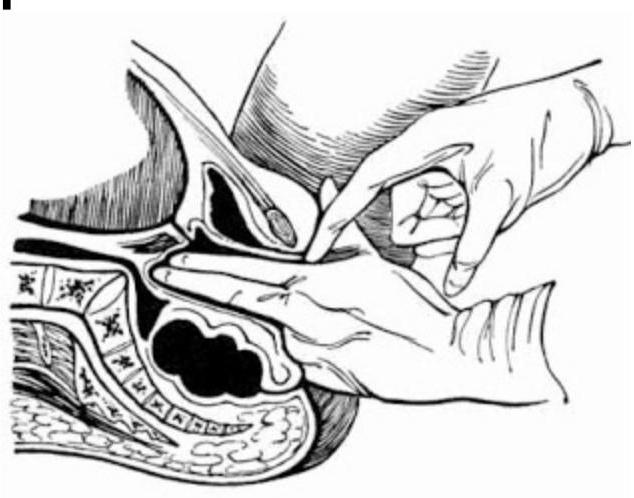
Pediatrics
1 questionsWhich of the following is not a known cause of neuroregression in children?
Pharmacology
3 questionsModafinil is primarily used for the treatment of which of the following conditions?
What is the treatment for extrapyramidal side effects induced by Haloperidol?
What is the mechanism of action of duloxetine?
Psychiatry
5 questionsWhich first-line conventional drug is commonly used in the treatment of delirium?
What is the PRIMARY psychological cause of oppositional behavior in young children?
Which of the following conditions is NOT typically associated with increased REM latency?
Which drug is not considered a mood stabilizer?
Most common complication of modified ECT