Following delivery, a tear involving the perineum and external anal sphincter with intact mucosa is classified as which grade?
Which of the following is NOT a cause of oligohydramnios?
Which of the following statements about chorionic villus sampling is false?
A 28-year-old primigravida with 32 weeks of gestation presents with profuse vaginal discharge since yesterday. She was advised USG, which showed a single live intrauterine gestational sac with FL and AC corresponding to the weeks of gestation and AFI as adequate. What is the diagnosis?
Poor prognostic factor for hydatidiform mole is -
Which of the following describes the points marked in the diagram of pelvic measurements?
Which of the following is not considered an absolute contraindication for the use of an Intra Uterine Contraceptive Device (IUD)?
NEET-PG 2015 - Obstetrics and Gynecology NEET-PG Practice Questions and MCQs
Question 61: Following delivery, a tear involving the perineum and external anal sphincter with intact mucosa is classified as which grade?
- A. First degree
- B. Second degree
- C. Third degree (Correct Answer)
- D. Fourth degree
Explanation: ***Third degree*** - A third-degree perineal tear involves the **perineum** and the **external anal sphincter (EAS)**, either partially or completely, while the **anal mucosa remains intact**. - This classification is crucial for determining the necessary repair technique and predicting potential long-term complications related to **anal incontinence**. *First degree* - A first-degree tear involves only the **skin** of the perineum and the **vaginal mucosa**, without involving the underlying muscle. - These tears are typically superficial and may not even require suturing. *Second degree* - A second-degree tear involves the **perineal muscles** but does not extend to the anal sphincter. - It includes the vaginal mucosa, perineal skin, and muscles but spares the **external anal sphincter**. *Fourth degree* - A fourth-degree tear is the most severe, involving the **perineum**, **external anal sphincter**, and extending through the **anal mucosa**, exposing the rectal lumen. - These tears carry the highest risk of **fecal incontinence** and require meticulous surgical repair.
Question 62: Which of the following is NOT a cause of oligohydramnios?
- A. Renal agenesis
- B. Amnion nodosum
- C. Chorioangioma (Correct Answer)
- D. IUGR
Explanation: ***Chorioangioma*** - A **chorioangioma** is a benign placental tumor that causes **polyhydramnios** (excess amniotic fluid), which is the **opposite** of oligohydramnios. - Large chorioangiomas lead to increased transudation from the tumor's vascular channels, fetal anemia, and high-output cardiac failure, resulting in increased fetal urine production. - This is clearly **NOT a cause** of oligohydramnios, making it the correct answer. *IUGR* - **Intrauterine growth restriction (IUGR)**, particularly with placental insufficiency, is a common cause of **oligohydramnios**. - Reduced placental perfusion leads to decreased **fetal renal blood flow** and diminished urine production. - Since fetal urine is the main source of amniotic fluid after 16 weeks, reduced output causes oligohydramnios. *Renal agenesis* - **Bilateral renal agenesis** (Potter syndrome) is a classic and severe cause of **oligohydramnios/anhydramnios**. - Complete absence of kidneys means **no fetal urine production**, eliminating the primary source of amniotic fluid in the second and third trimesters. - Results in severe oligohydramnios with associated pulmonary hypoplasia and Potter facies. *Amnion nodosum* - **Amnion nodosum** refers to small, grayish-yellow nodules on the fetal surface of the amnion, composed of aggregated fetal squamous epithelial cells and vernix. - These nodules are a **pathological finding** that occurs as a **consequence** of chronic oligohydramnios, not a cause. - They form due to prolonged contact between the fetal skin and amnion when amniotic fluid is severely reduced. - While technically "not a cause," it is strongly **associated with** oligohydramnios, whereas chorioangioma causes the opposite condition entirely.
Question 63: Which of the following statements about chorionic villus sampling is false?
- A. Can cause limb deformities
- B. Is used for prenatal genetic diagnosis
- C. Villi are collected from chorion frondosum
- D. Is performed only in second trimester of pregnancy (Correct Answer)
Explanation: ***Is performed only in second trimester of pregnancy*** - This statement is false because **chorionic villus sampling (CVS)** is typically performed earlier in pregnancy, specifically during the **first trimester**, usually between 10 and 13 weeks of gestation. - Performing CVS only in the second trimester would negate one of its main advantages: providing earlier genetic diagnostic information than **amniocentesis**. *Is used for prenatal genetic diagnosis* - **CVS** is a primary method for **prenatal genetic diagnosis**, allowing for the detection of chromosomal abnormalities and genetic disorders. - It involves analyzing fetal cells obtained from the **chorionic villi**. *Villi are collected from chorion frondosum* - The sample for **CVS** is indeed collected from the **chorion frondosum**, which is the fetal part of the placenta containing numerous chorionic villi. - These villi are genetically identical to the fetus, making them suitable for **genetic analysis**. *Can cause limb deformities* - There is a recognized, albeit small, risk of **limb reduction defects** associated with CVS, particularly if performed very early in gestation (before 9-10 weeks). - This risk is part of the counseling provided to prospective parents considering the procedure.
Question 64: A 28-year-old primigravida with 32 weeks of gestation presents with profuse vaginal discharge since yesterday. She was advised USG, which showed a single live intrauterine gestational sac with FL and AC corresponding to the weeks of gestation and AFI as adequate. What is the diagnosis?
- A. Candidiasis
- B. Trichomoniasis
- C. Normal vaginal discharge (Correct Answer)
- D. Preterm Premature Rupture of Membranes (PPROM)
Explanation: ***Normal vaginal discharge*** - Profuse vaginal discharge is a common and **physiological occurrence** in pregnancy due to increased estrogen levels and blood flow to the vagina. - The ultrasound findings of **adequate amniotic fluid index (AFI)** rule out rupture of membranes, and no other symptoms of infection are reported. *Preterm Premature Rupture of Membranes (PPROM)* - PPROM would present with a significant reduction in the **amniotic fluid index (AFI)** on ultrasound, which is noted as adequate in this case. - The discharge in PPROM is typically **amniotic fluid**, which is clear and watery, unlike mere profuse vaginal discharge. *Trichomoniasis* - This infection typically causes a **frothy, greenish-yellow discharge** with a foul odor, along with vulvar itching and irritation. - These characteristic symptoms are not mentioned in the patient's presentation. *Candidiasis* - Vaginal candidiasis usually presents with a **thick, white, cottage cheese-like discharge** accompanied by intense itching and burning. - The patient's description of discharge is simply "profuse," without these specific characteristics.
Question 65: Poor prognostic factor for hydatidiform mole is -
- A. Prior molar pregnancy
- B. Metastasis to lung
- C. No prior chemotherapy
- D. WHO score > 8 (Correct Answer)
Explanation: ***WHO score > 8*** - A **WHO score > 8** (more specifically, WHO/FIGO score ≥7) indicates **high-risk gestational trophoblastic neoplasia (GTN)**, which is associated with a poor prognosis and requires multi-agent chemotherapy. - The WHO prognostic scoring system incorporates various factors: age, prior pregnancy outcome, antecedent pregnancy type, interval from index pregnancy, pre-treatment hCG level, largest tumor size, site of metastases, and number of metastases. - This is the **strongest poor prognostic indicator** among the options listed. *Prior molar pregnancy* - A **prior molar pregnancy** increases the *risk* of developing another molar pregnancy (recurrence risk ~1-2%), but it is **not a component of the WHO prognostic scoring system** and is not a poor prognostic factor for the outcome of current GTN. - The history affects surveillance requirements but doesn't dictate the difficulty of treating the current episode. *Metastasis to lung* - **Lung metastases** are actually among the **better prognostic sites** for metastatic GTN in the WHO scoring system. - Lung and vaginal metastases score only 1 point, whereas liver and brain metastases (true poor prognostic sites) score 4 points each. - While any metastasis indicates more advanced disease, isolated lung metastases generally have a *good prognosis* with appropriate chemotherapy, with cure rates >90%. *No prior chemotherapy* - The *absence* of **prior chemotherapy** is a **favorable prognostic factor**, not a poor one. - Patients who have *failed* prior chemotherapy or have received ≥2 drugs previously score 2-4 points in the WHO system, indicating worse prognosis. - No prior chemotherapy (scores 0 points) means better treatment response and outcomes.
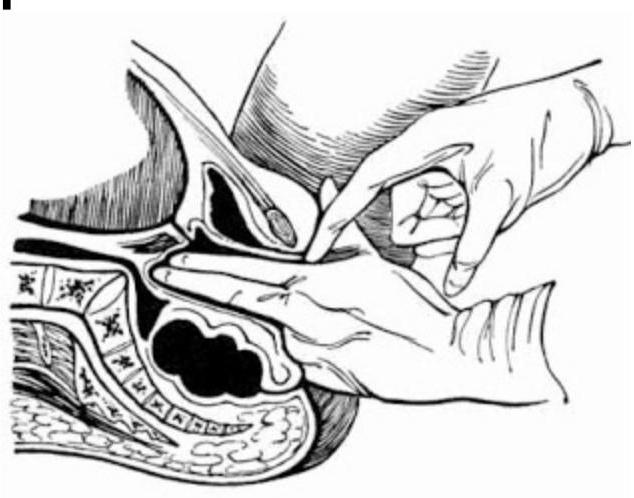
Question 66: Which of the following describes the points marked in the diagram of pelvic measurements?
- A. Diagonal conjugate (Correct Answer)
- B. Obstetric conjugate measurement
- C. True conjugate measurement
- D. Oblique conjugate measurement
Explanation: ***Diagonal conjugate*** - The image depicts a **bimanual examination** where one hand is inserted vaginally to measure the distance from the **lower border of the pubic symphysis** to the **sacral promontory**. - This measurement directly corresponds to the **diagonal conjugate**, which is a clinically estimated measurement of the pelvic inlet. *Obstetric conjugate measurement* - The **obstetric conjugate** is the smallest anteroposterior diameter through which the fetal head must pass. - It extends from the **middle of the sacral promontory** to the **innermost aspect of the pubic symphysis** and cannot be measured directly by clinical examination. *True conjugate measurement* - The **true conjugate**, also known as the anatomical conjugate, extends from the **sacral promontory** to the **upper border of the pubic symphysis**. - Like the obstetric conjugate, it is not directly palpable and must be estimated from the diagonal conjugate (true conjugate = diagonal conjugate - 1.5 to 2 cm). *Oblique conjugate measurement* - The **oblique conjugate** measures the distance between the sacroiliac joint on one side to the iliopectineal eminence on the opposite side. - This measurement is not typically assessed during a routine pelvic examination as depicted and is more relevant for identifying asymmetric pelvic deformities.
Question 67: Which of the following is not considered an absolute contraindication for the use of an Intra Uterine Contraceptive Device (IUD)?
- A. Undiagnosed vaginal bleeding
- B. Pregnancy
- C. Pelvic inflammatory disease
- D. Uterine malformation (Correct Answer)
Explanation: ***Uterine malformation*** - While a uterine malformation can make IUD insertion more difficult or reduce its effectiveness, it is often considered a **relative contraindication**, depending on the specific anomaly and the patient's desire for contraception. - In certain cases, an IUD might still be a viable option, but it requires careful consideration and specialized insertion techniques. *Pregnancy* - The presence of an existing pregnancy is an **absolute contraindication** for IUD insertion, as it can lead to complications such as miscarriage or ectopic pregnancy. - An IUD is a contraceptive device, and inserting it when a woman is already pregnant directly contradicts its purpose and poses significant risks. *Undiagnosed vaginal bleeding* - This is an **absolute contraindication** because it could be a symptom of a serious underlying condition, such as cervical cancer, endometrial cancer, or ectopic pregnancy. - Inserting an IUD before diagnosing the cause of the bleeding could delay treatment of a potentially life-threatening condition and exacerbate the bleeding. *Pelvic inflammatory disease* - Current or recent (within the last 3 months) **pelvic inflammatory disease (PID)** is an **absolute contraindication** due to the increased risk of worsening infection. - IUD insertion can introduce bacteria from the vagina into the uterus, potentially exacerbating an existing infection or causing a new one.