All (1550)Anatomy (110)Anesthesiology (34)Biochemistry (129)Community Medicine (109)Dental (16)Dermatology (34)ENT (62)Forensic Medicine (100)General Medicine (2)Internal Medicine (120)Microbiology (108)Obstetrics and Gynecology (79)Ophthalmology (78)Orthopaedics (41)Pathology (90)Pediatrics (33)Pharmacology (134)Physiology (91)Psychiatry (6)Psychiatry (81)Radiology (41)Surgery (52)
Internal Medicine
1 questionsQ1301
Wireless capsule endoscopy is done to visualize which of the following condition?
Ophthalmology
1 questionsQ1301
Fluorescein angiography is used to examine -
Radiology
7 questionsQ1301
For pericardial calcifications, which is the best investigation?
Q1302
Barium swallow is used for -
Q1303
"String of beads" appearance on horizontal abdominal view X-ray is suggestive of:
Q1304
What condition is indicated by the double bubble sign on an abdominal X-ray?
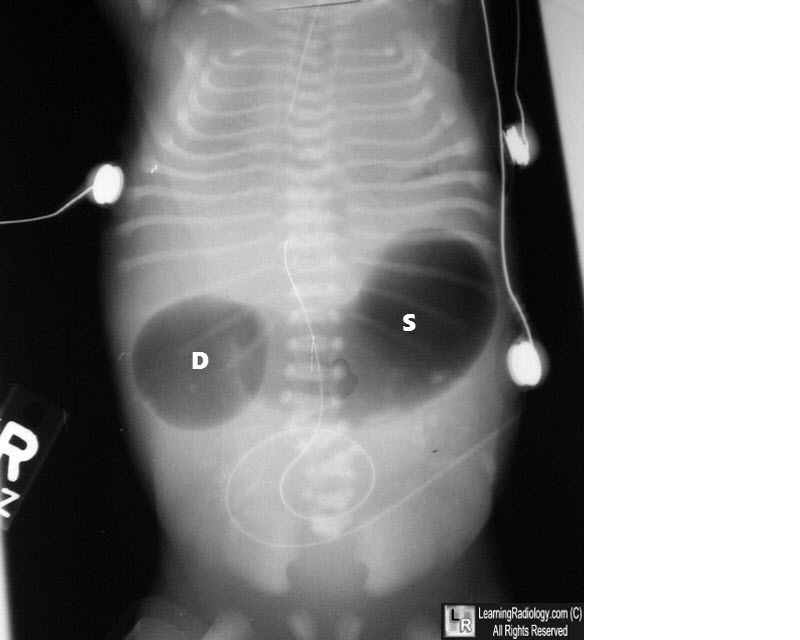
Q1305
Investigation with least radiation dose in the diagnosis of Meckel's diverticulum is -
Q1306
What is the echogenic lesion size criterion for chronic pancreatitis?
Q1307
What is the CT scan finding in a carotid cavernous sinus fistula?
Surgery
1 questionsQ1301
Pulled up cecum is seen in which condition?