Biochemistry
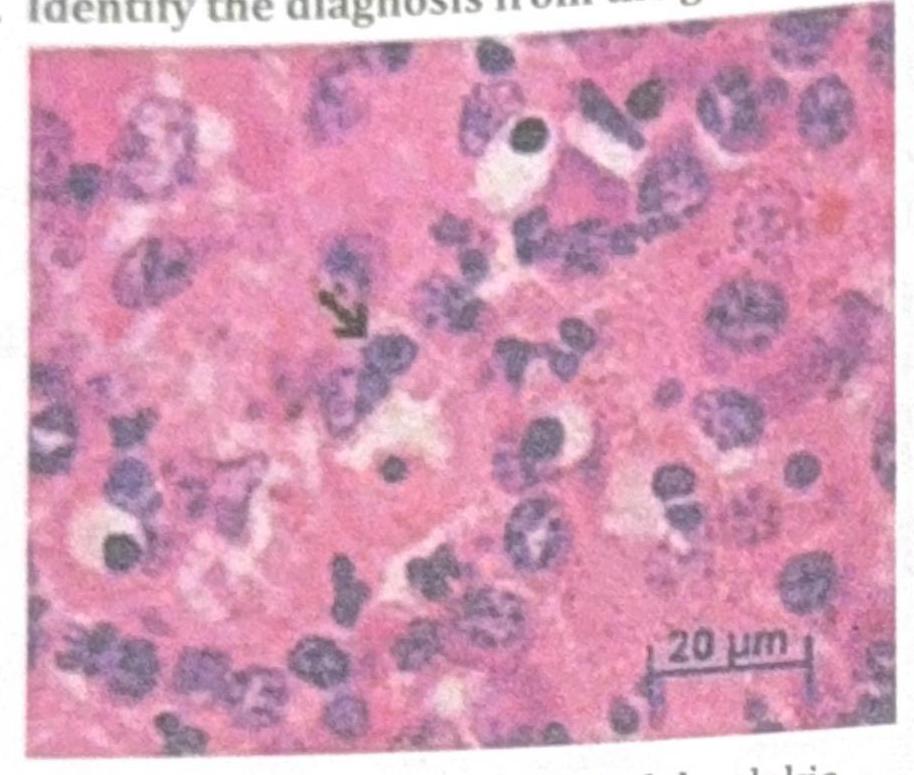
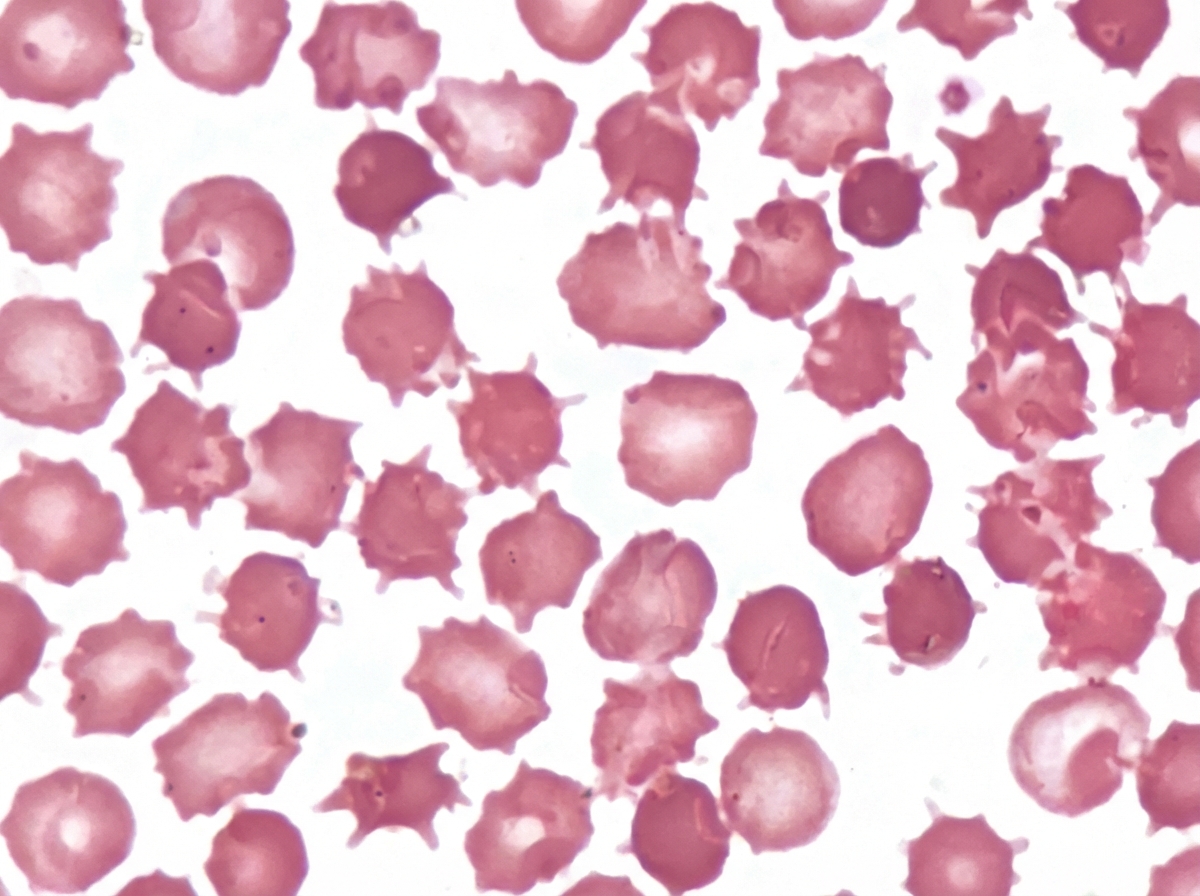
1 questionsAn adult male presented with a protruding abdomen, diarrhea, visual symptoms, and neurological manifestations. His LDL is low. Based on the peripheral smear finding shown in the image, what is the likely diagnosis?
Dermatology
2 questionsThe skin biopsy shown below is most consistent with which of the following conditions? 
A child presents with itchy lesions and diarrhea and has been advised to follow a gluten-free diet. What is the most likely etiology of this condition?
Internal Medicine
3 questionsWhich of the following antibodies is associated with Celiac disease?
A patient is a known case of thalassemia. Which of the following viruses would be responsible for attacking progenitor cells and causing aplastic anemia?
A patient presents with respiratory distress and is diagnosed with panacinar emphysema. Which of the following is deficient?
Pathology
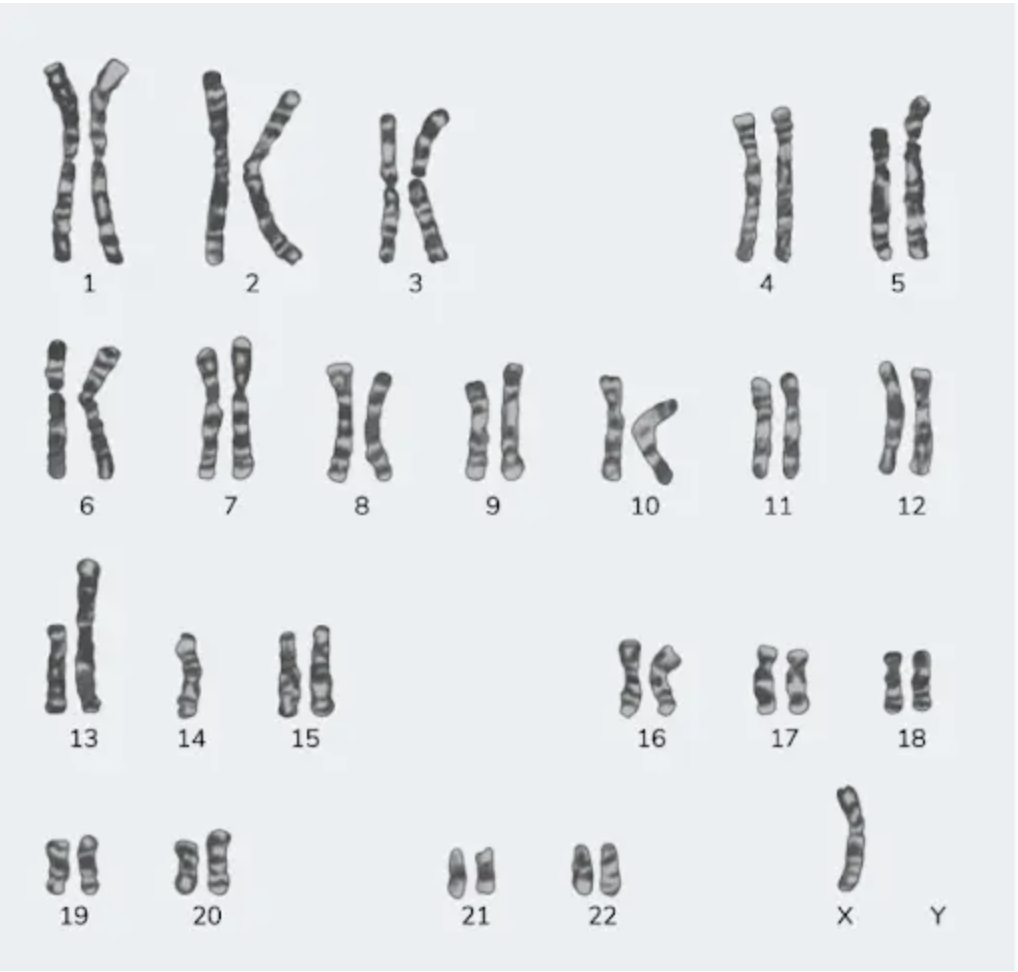
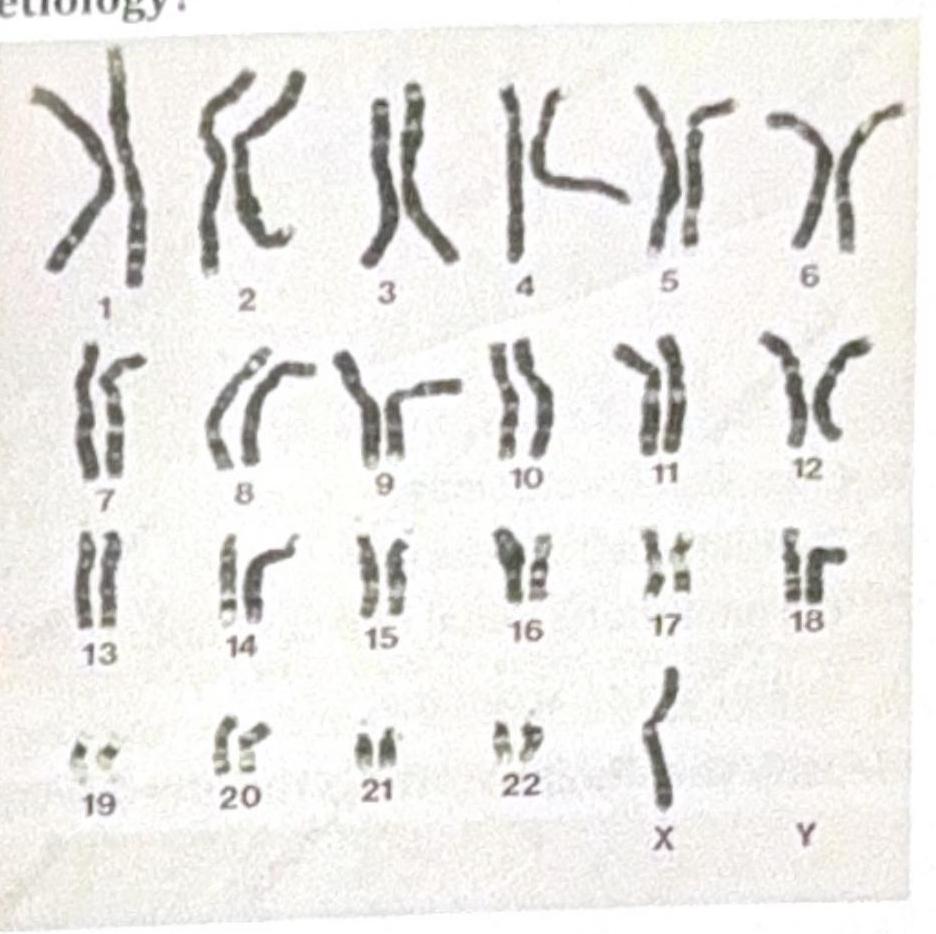
4 questionsA 23-year-old female with a height of 4 feet has a karyotype as shown in the image below. Which among the following indicates the correct etiology?
Identify the image and the disease it is associated with: 
A male patient is not responding to oxygen therapy and has been diagnosed with ARDS (Acute Respiratory Distress Syndrome). What is the role of IL-8 in ARDS?
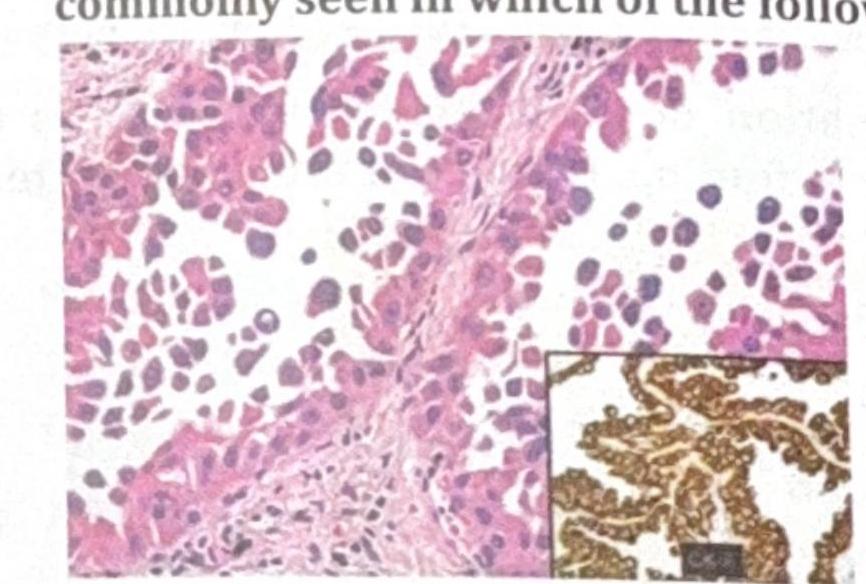
Identify the diagnosis from the given image