Anatomy
7 questionsThe covering of an omphalocele is derived from which of the following layers?
A patient presents with pain in the back of the thigh and leg after lifting heavy weights. Which spinal segment is most likely involved?
Which artery is palpated behind the medial malleolus and in front of the Achilles tendon?
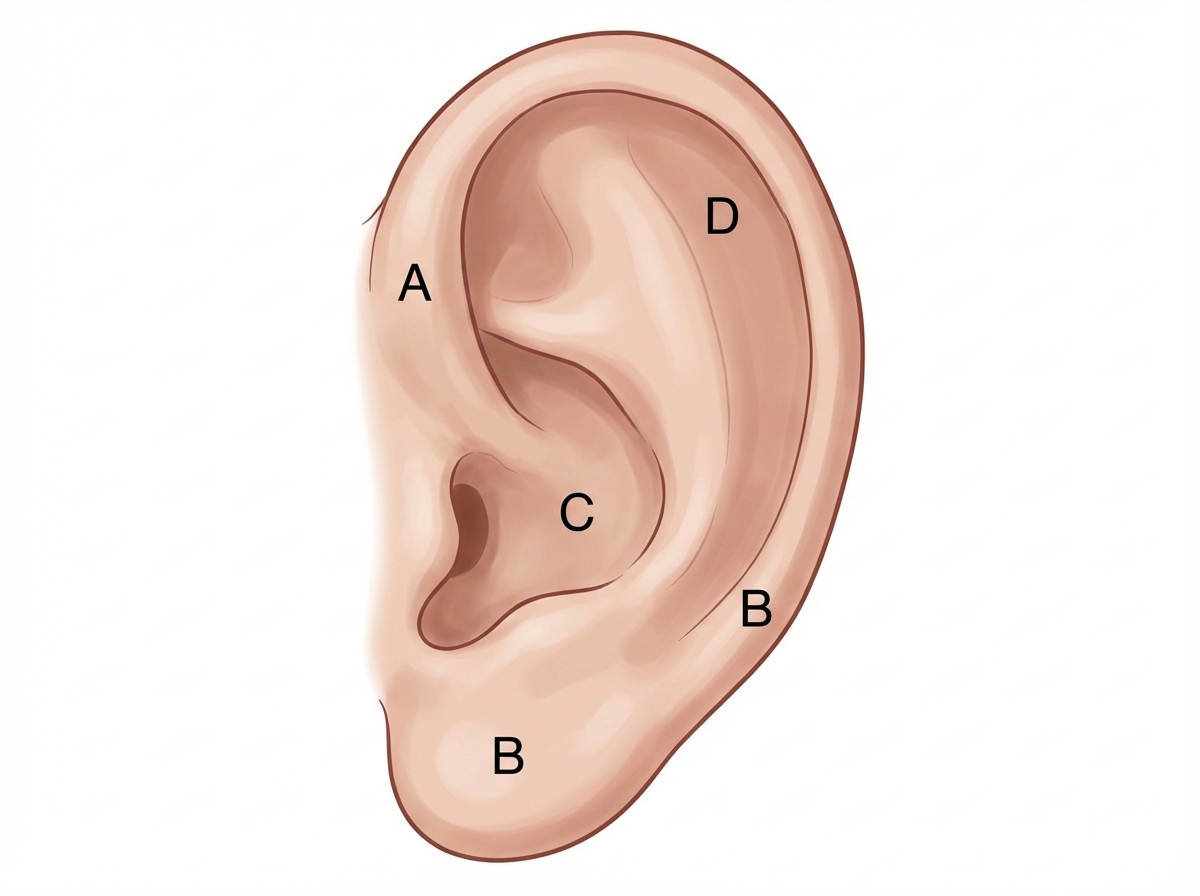
Match the following nerves to their respective areas of supply to the auricle
A patient diagnosed with sciatica has tender hamstrings. Which of the following nerves supplies a hybrid muscle that is partially spared in this patient?
What is the most common site of congenital diaphragmatic hernia?
A patient presents with loss of sensation on the lateral 3½ fingers and thenar atrophy. Which nerve is most likely involved?
Pediatrics
1 questionsWhat is the diagnosis based on the image shown 
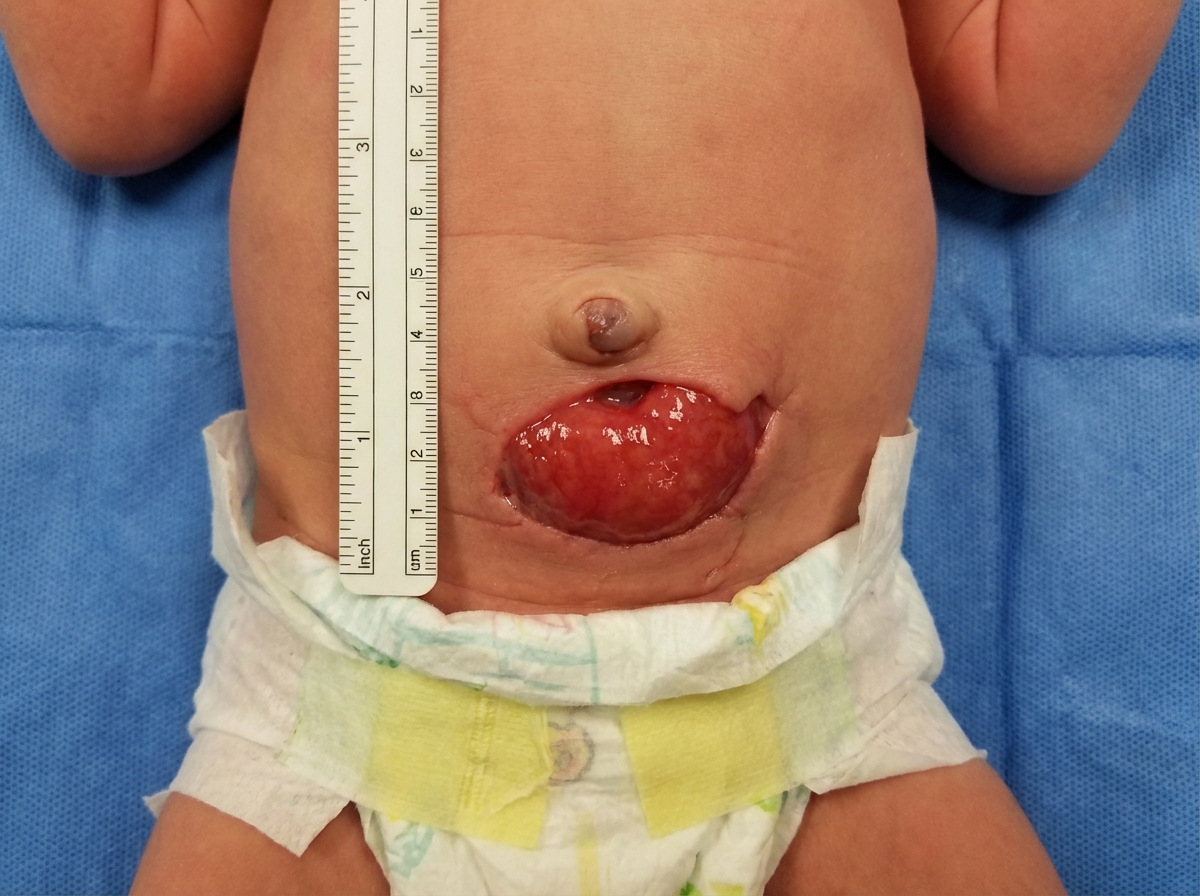
Physiology
1 questionsWhat are the effects of a lesion in Brodmann area 22?
Surgery
1 questionsA patient presents with fecal discharge from the umbilicus. What is the most likely diagnosis?