Back
How to Study Endocrinology for USMLE Step 2 CK: High-Yield Topics, Clinical Vignette Strategy and Exam Checklist (2026)
Master USMLE Step 2 CK endocrinology with this comprehensive guide covering diabetes management, thyroid disorders, adrenal conditions, clinical vignette strategy, and exam checklist for 2026.

How to Study Endocrinology for USMLE Step 2 CK: High-Yield Topics, Clinical Vignette Strategy and Exam Checklist (2026)
You are probably staring at endocrinology in your Step 2 CK prep wondering how to tackle the maze of hormone cascades, drug mechanisms, and clinical presentations. Here's the reality: endocrinology makes up roughly 8-12% of Step 2 CK questions, and unlike Step 1's focus on physiology, Step 2 CK tests your ability to diagnose and manage real patients through clinical vignettes.
The good news? Endocrinology follows predictable patterns. Most questions test your ability to recognize classic presentations (like the cushingoid patient with purple striae), choose appropriate initial workups (TSH vs free T4 timing), and avoid common management pitfalls (confusing central vs nephrogenic DI). Master these patterns, and you will see immediate score gains.
This guide breaks down the highest-yield endocrinology topics for Step 2 CK, shows you how to approach clinical vignettes systematically, and gives you a final exam checklist to ensure nothing slips through the cracks.
High-Yield Endocrinology Topics for Step 2 CK
Diabetes Mellitus: Management-Heavy Territory
Step 2 CK doesnt care about insulin synthesis pathways. It cares whether you know when to start metformin vs insulin, how to manage DKA vs HHS, and which complications require immediate intervention.
Type 1 Diabetes Management:
Initial presentation: polyuria, polydipsia, weight loss, ketosis
Management: insulin (never oral agents alone), carb counting, glucose monitoring
Complications: DKA (anion gap acidosis, ketones), hypoglycemia awareness
Type 2 Diabetes Management:
First-line: metformin (unless contraindicated)
Add-on agents: sulfonylureas, GLP-1 agonists, SGLT-2 inhibitors, insulin
Target HbA1c: <7% (individualize based on age, comorbidities)
The mnemonic engine generates instant recall chains for diabetes drug MOAs — biguanides, sulfonylureas, GLP-1 agonists, SGLT-2 inhibitors in one pass, helping students tackle the heaviest memorization load in pharmacology without re-reading drug tables repeatedly. Diabetic Ketoacidosis (DKA):
Triad: hyperglycemia (>250), ketosis, anion gap acidosis
Management: IV fluids, insulin, electrolyte replacement (especially potassium)
Complications: cerebral edema (especially in kids), hypokalemia
Hyperosmolar Hyperglycemic State (HHS):
Higher glucose (>600), no ketosis, severe dehydration
Management: aggressive fluid resuscitation, insulin, electrolyte monitoring
Study tip: Practice endocrinology questions focusing on when to choose DKA vs HHS management and drug selection scenarios.
Thyroid Disorders: Diagnostic Workup Focus
Hypothyroidism:
Clinical: fatigue, weight gain, cold intolerance, bradycardia, delayed DTRs
Labs: elevated TSH, low free T4
Management: levothyroxine (start low in elderly/cardiac patients)
Subclinical: elevated TSH, normal free T4
Hyperthyroidism:
Clinical: weight loss, heat intolerance, tachycardia, tremor, anxiety
Labs: suppressed TSH, elevated free T4/T3
Causes: Graves (ophthalmopathy, pretibial myxedema), toxic multinodular goiter, thyroiditis
Thyroid Storm:
Clinical: hyperthermia, tachycardia, altered mental status, heart failure
Management: propylthiouracil/methimazole, beta-blockers, steroids, iodine
After reading thyroid disorder lessons, students can immediately drill Probe Game rounds on hyperthyroid vs hypothyroid differentials, opening new study paths for active recall practice. Key Testing Pattern: Order TSH first. If abnormal, then free T4. If hyperthyroid, consider radioiodine uptake scan to differentiate causes.
Adrenal Disorders: Classic Presentations
Cushing Syndrome vs Cushing Disease:
Syndrome: any cause of excess cortisol
Disease: pituitary adenoma specifically
Clinical: central obesity, purple striae, proximal myopathy, moon face, buffalo hump
Workup: 24-hour urine cortisol or dexamethasone suppression test
Addison Disease (Primary Adrenal Insufficiency):
Clinical: fatigue, hyperpigmentation, hyperkalemia, hyponatremia
Labs: low cortisol, elevated ACTH
Management: hydrocortisone replacement, fludrocortisone for mineralocorticoids
Primary Hyperaldosteronism (Conn Syndrome):
Clinical: hypertension, hypokalemia, muscle weakness
Workup: aldosterone/renin ratio
Pheochromocytoma:
Triad: headache, diaphoresis, palpitations/tachycardia
Workup: 24-hour urine catecholamines or plasma metanephrines
Management: alpha-blockers before beta-blockers (avoid hypertensive crisis)
Study adrenal disorder lessons and practice related flashcards to cement these high-yield patterns.
Pituitary Disorders: Hormone Excess/Deficiency
Acromegaly:
Cause: growth hormone excess (usually pituitary adenoma)
Clinical: enlarged hands/feet, coarse facial features, macroglossia, carpal tunnel
Workup: IGF-1 levels, oral glucose tolerance test with GH measurement
Prolactinoma:
Clinical: galactorrhea, amenorrhea (women), erectile dysfunction (men)
Workup: prolactin levels (>200 suggests prolactinoma)
Management: dopamine agonists (cabergoline, bromocriptine)
Diabetes Insipidus (DI):
Central DI: ADH deficiency (responds to desmopressin)
Nephrogenic DI: kidney resistance to ADH (doesnt respond to desmopressin)
Workup: water deprivation test, desmopressin trial
SIADH:
Clinical: hyponatremia, concentrated urine, euvolemic
Causes: CNS disorders, lung disease, medications
Management: fluid restriction, demeclocycline
Calcium Disorders and MEN Syndromes
Hypercalcemia:
Most common causes: hyperparathyroidism, malignancy
Clinical: kidney stones, bone disease, peptic ulcers, psychiatric symptoms ("stones, bones, groans, psychiatric overtones")
Workup: PTH levels (elevated = hyperparathyroidism, suppressed = non-PTH causes)
MEN Syndromes:
MEN 1: parathyroid, pancreatic islets, pituitary ("3 P's")
MEN 2A: medullary thyroid cancer, pheochromocytoma, hyperparathyroidism
MEN 2B: medullary thyroid cancer, pheochromocytoma, marfanoid habitus, mucosal neuromas
The mnemonic engine builds memory chains for MEN 1/2A/2B tumor lists and anterior pituitary hormone triggers, making complex classifications stick without repeatedly re-reading tables. PCOS (Polycystic Ovary Syndrome):
Clinical: oligomenorrhea, hirsutism, acne, obesity
Labs: elevated LH/FSH ratio, elevated androgens
Management: lifestyle modifications, metformin, OCPs for cycle regulation
Clinical Vignette Strategy for Step 2 CK Endocrinology
Endocrinology is almost entirely clinical-vignette territory on Step 2 CK. You won't see standalone hormone pathway questions. Instead, expect patient presentations that test your diagnostic reasoning and next-step decision making.
Typical Vignette Patterns
Pattern 1: Diagnostic Workup "A 45-year-old woman presents with weight gain, fatigue, and cold intolerance over 6 months. Physical exam shows bradycardia and delayed DTRs. What is the most appropriate initial test?"
Answer: TSH (not free T4 first)
Pattern 2: Management Decision "A 28-year-old man with type 1 diabetes presents with nausea, vomiting, and fruity breath odor. Labs show glucose 380, anion gap 18, moderate ketones. What is the most appropriate initial management?"
Answer: IV normal saline (before insulin)
Pattern 3: Complication Recognition "A 55-year-old woman with Graves disease develops fever, tachycardia, and altered mental status 2 days after thyroidectomy. What is the most likely diagnosis?"
Answer: Thyroid storm
Step-by-Step Vignette Approach
1. Identify the chief complaint and timeline - acute vs chronic presentations guide your differential
2. Note key physical exam findings - cushingoid features, thyroid exam, skin changes
3. Analyze lab patterns - glucose, electrolytes, hormone levels
4. Consider the question type - diagnosis, next best step, management, complication
5. Apply clinical decision rules - TSH first for thyroid, dexamethasone suppression for Cushing
Clinical Rounds presents AI-guided case scenarios like a 45-year-old with proximal muscle weakness, purple striae, and hypertension, forcing students to work through diagnostic reasoning and management steps that mirror actual Step 2 CK question formats.
Common Endocrinology Pitfalls to Avoid
Cushing Syndrome vs Disease Confusion:
Syndrome = any cause of excess cortisol
Disease = specifically pituitary adenoma
Don't mix up the terminology in your answer choices
DI Central vs Nephrogenic Workup:
Both present with polyuria and polydipsia
Central responds to desmopressin trial, nephrogenic doesnt
Water deprivation test helps differentiate
Thyroid Function Test Ordering:
Always order TSH first
Only order free T4 if TSH is abnormal
Don't jump straight to antibodies or imaging
Diabetes Management Priorities:
DKA: fluids first, then insulin
Type 2 diabetes: metformin first-line unless contraindicated
Don't start insulin immediately in newly diagnosed type 2
When you get endocrinology MCQs wrong, Explanation Chat delivers immediate AI-driven breakdowns of why the right answer is right and why your distractor was wrong, plugging exact reasoning gaps rather than providing generic topic reviews.
Study Schedule and Resource Integration
Week 1-2: Foundation Building
Complete endocrinology lessons for each major topic
Focus on pathophysiology and clinical presentations
Create disease comparison tables
Week 3-4: Active Recall and Application
Daily endocrinology flashcards for hormone pathways and drug mechanisms
Practice clinical vignette questions focusing on diagnosis and management
Run dedicated endocrinology clinical round sessions to stress-test vignette-to-diagnosis mapping
Week 5-6: Integration and Weak Spot Targeting
Mixed practice questions combining endocrinology with other systems
Focus on commonly tested combinations (diabetes + cardiovascular, thyroid + pregnancy)
Review explanation chats for wrong answers to build personal weak spot log
USMLE Step 2 CK Endocrinology Exam Checklist
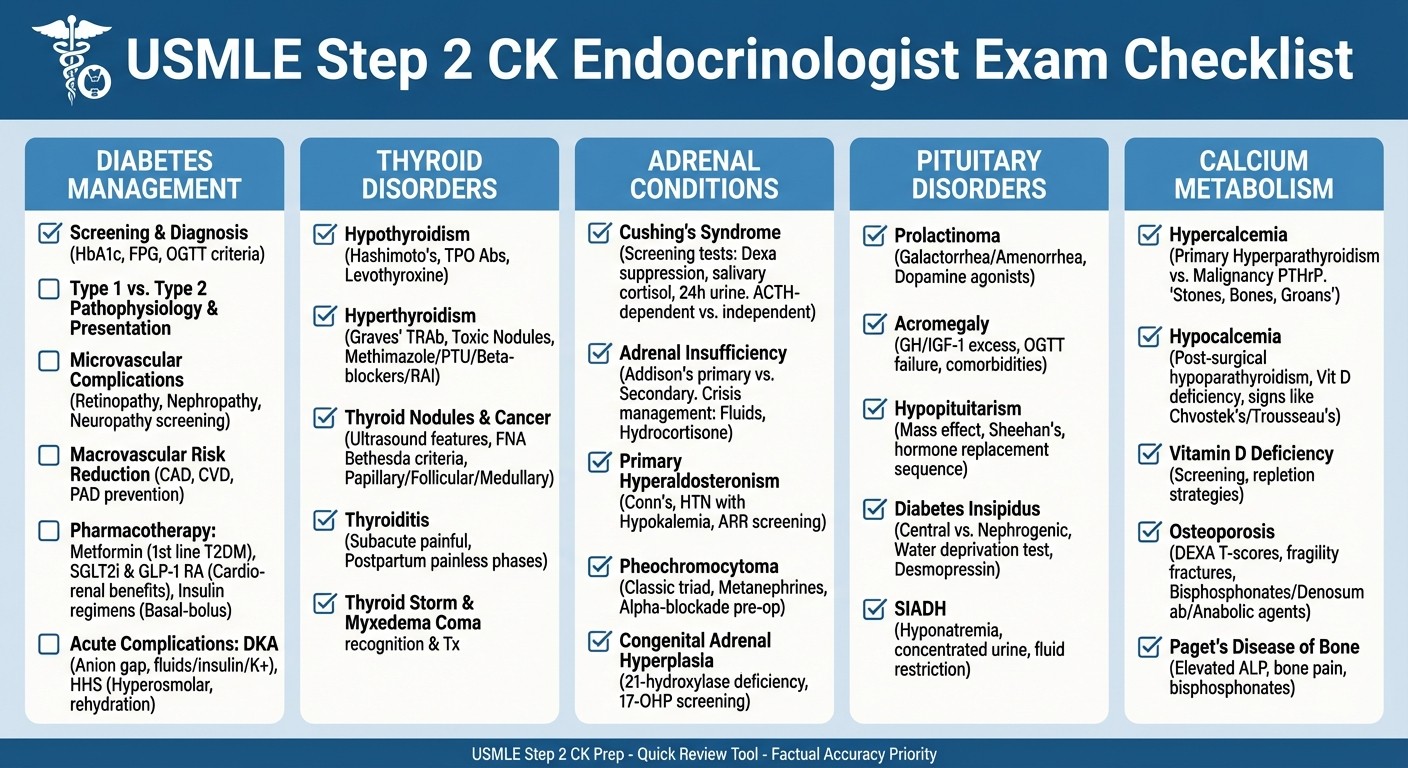
Diabetes Mellitus
[ ] Type 1 vs Type 2 clinical presentation differences
[ ] Metformin first-line for Type 2 (unless contraindicated)
[ ] DKA triad: hyperglycemia >250, ketosis, anion gap acidosis
[ ] HHS: glucose >600, no ketosis, severe dehydration
[ ] DKA management: IV fluids first, then insulin, monitor potassium
[ ] Target HbA1c <7% (individualize based on patient factors)
Thyroid Disorders
[ ] Order TSH first, then free T4 if abnormal
[ ] Hypothyroidism: elevated TSH, low free T4, start levothyroxine
[ ] Hyperthyroidism: suppressed TSH, elevated free T4/T3
[ ] Graves disease: ophthalmopathy, pretibial myxedema
[ ] Thyroid storm: hyperthermia, tachycardia, altered mental status
[ ] Thyroid storm management: antithyroid drugs, beta-blockers, steroids, iodine
Adrenal Disorders
[ ] Cushing syndrome (any cause) vs Cushing disease (pituitary)
[ ] Cushing clinical: central obesity, purple striae, proximal myopathy
[ ] Addison disease: fatigue, hyperpigmentation, hyperK, hypoNa
[ ] Primary hyperaldosteronism: hypertension + hypokalemia
[ ] Pheochromocytoma triad: headache, diaphoresis, palpitations
[ ] Pheo management: alpha-blockers before beta-blockers
Pituitary Disorders
[ ] Acromegaly: enlarged hands/feet, coarse features, check IGF-1
[ ] Prolactinoma: galactorrhea, amenorrhea, treat with dopamine agonists
[ ] Central DI: responds to desmopressin
[ ] Nephrogenic DI: doesnt respond to desmopressin
[ ] SIADH: hyponatremia + concentrated urine, fluid restriction
Calcium and MEN Syndromes
[ ] Hypercalcemia workup: check PTH (elevated = hyperparathyroidism)
[ ] MEN 1: parathyroid, pancreatic islets, pituitary (3 P's)
[ ] MEN 2A: medullary thyroid cancer, pheo, hyperparathyroidism
[ ] MEN 2B: medullary thyroid cancer, pheo, marfanoid habitus
[ ] PCOS: oligomenorrhea, hirsutism, elevated LH/FSH ratio
Common Pitfalls to Remember
[ ] Never confuse central vs nephrogenic DI management
[ ] Don't order free T4 before TSH
[ ] Remember fluid resuscitation before insulin in DKA
[ ] Alpha-blockers must come before beta-blockers in pheochromocytoma
[ ] Distinguish Cushing syndrome from Cushing disease terminology
Frequently Asked Questions
How much time should I spend on endocrinology for Step 2 CK?
Allocate 2-3 weeks of dedicated endocrinology study within your 8-12 week Step 2 CK prep. Endocrinology comprises 8-12% of the exam, so it deserves focused attention but shouldnt dominate your schedule.
What's the most high-yield endocrinology topic for Step 2 CK?
Diabetes management, particularly DKA vs HHS differentiation and Type 2 diabetes medication selection. These topics appear frequently and test practical clinical decision-making skills.
Should I memorize all hormone pathways for Step 2 CK endocrinology?
No. Step 2 CK focuses on clinical application, not detailed pathophysiology. Focus on diagnostic workups, management decisions, and recognizing classic clinical presentations rather than memorizing biochemical pathways.
How do I avoid confusing central vs nephrogenic diabetes insipidus?
Remember the desmopressin trial: central DI responds (because ADH is missing), nephrogenic DI doesnt respond (because kidneys resist ADH). Use this functional difference rather than trying to memorize causes.
What's the best way to practice endocrinology clinical vignettes?
Focus on pattern recognition: chief complaint → key exam findings → appropriate workup → management. Practice with case-based questions that mirror the Step 2 CK format rather than isolated fact-based questions.
How important are MEN syndromes for Step 2 CK?
Moderately important. Know the basic components of MEN 1 (3 P's) and MEN 2A/2B, but dont spend excessive time memorizing rare manifestations. Focus on when to suspect these syndromes clinically.
Prepare smarter with Oncourse AI — adaptive MCQs, spaced repetition, and AI explanations built for USMLE Step 2 CK. Download free on Android and iOS.