Cardiology — MCQs

On this page
A 19-year-old Caucasian college student is home for the summer. Her parents note that she has lost quite a bit of weight. The daughter explains that the weight loss was unintentional. She also notes an increase in thirst, hunger, and urine output. Her parents decide to take her to their family physician, who suspects finding which of the following?
A 14-year-old boy is brought to the physician for generalized fatigue and mild shortness of breath on exertion for 3 months. He has a history of recurrent patellar dislocations. He is at the 99th percentile for height and at the 30th percentile for weight. His temperature is 37°C (98.6°F), pulse is 99/min, and blood pressure is 140/50 mm Hg. Examination shows scoliosis, a protruding breast bone, thin extremities, and flat feet. Ocular examination shows upwards displacement of bilateral lenses. A grade 3/6 early diastolic murmur is heard along the left sternal border. Further evaluation of this patient is most likely to show which of the following?
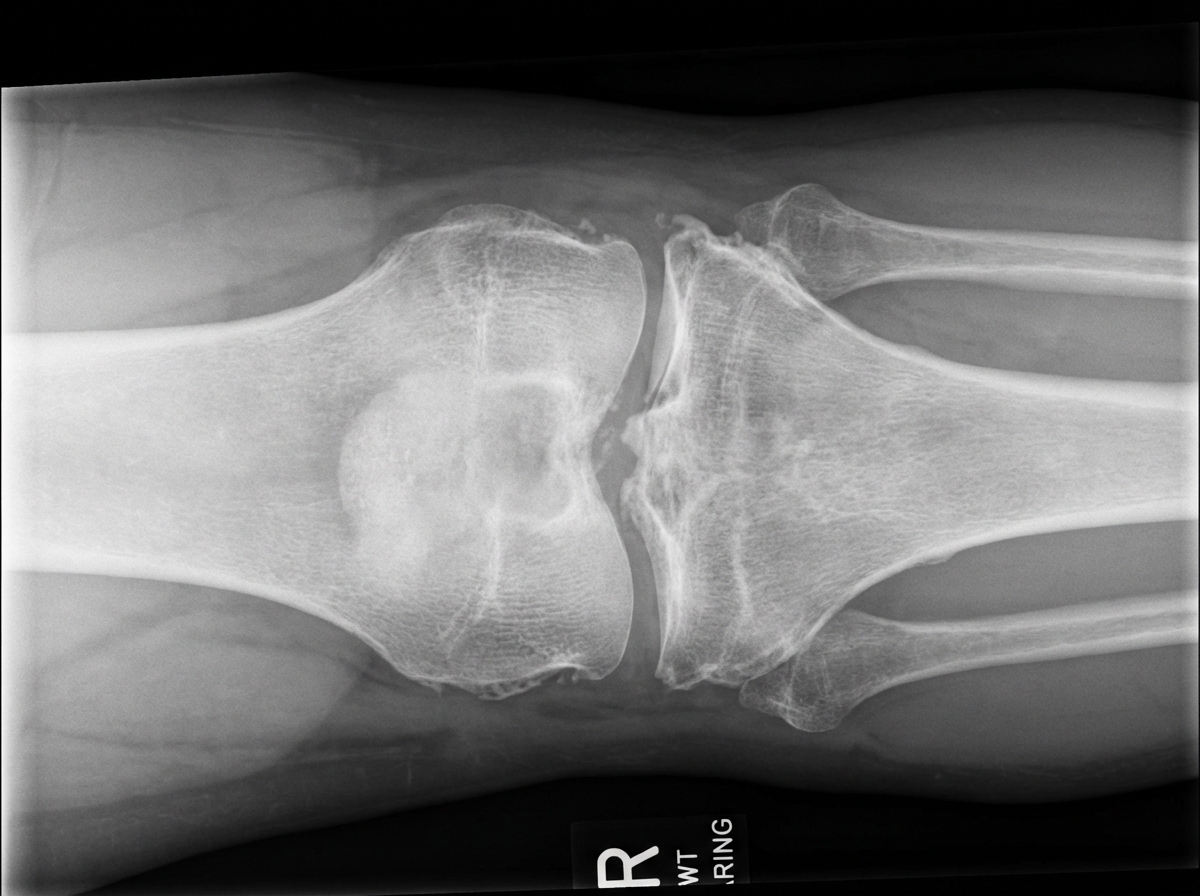
A 52-year-old woman comes to the physician because of a 3-week history of pain in her right knee. The pain is worse at the end of the day and when she walks. She says that it has become difficult for her to walk up the flight of stairs to reach her apartment. She has hypertension and psoriasis. Her sister has rheumatoid arthritis. She drinks 2–3 beers daily. Current medications include hydrochlorothiazide, topical betamethasone, and a multivitamin. She is 160 cm (5 ft 3 in) tall and weighs 92 kg (202 lb); BMI is 36 kg/m2. She appears anxious. Her temperature is 37°C (98.6°F), pulse is 87/min, and blood pressure is 135/83 mm Hg. Cardiopulmonary examinations shows no abnormalities. There are several scaly plaques over the patient's upper and lower extremities. The right knee is not tender nor erythematous; range of motion is limited. Crepitus is heard on flexion and extension of the knee. Her hemoglobin concentration is 12.6 g/dL, leukocyte count is 9,000/mm3, and erythrocyte sedimentation rate is 16 mm/h. An x-ray of the right knee is shown. Which of the following is the most appropriate next step in the management of this patient?
A 40-year-old woman comes to the physician because of a small lump on the right side of her neck that she noticed while putting lotion on 1 week ago. She does not have any weight change, palpitations, or altered bowel habits. There is no family history of serious illness. Menses occur at regular 30-day intervals and lasts for 4 days. She appears well. Her temperature is 37°C (98.6° F), pulse is 88/min, and blood pressure is 116/74 mm Hg. Examination shows a small swelling on the right side of the neck that moves with swallowing. There is no lymphadenopathy. Ultrasound of the neck shows a 0.9-cm (0.35-in) right lobe thyroid mass with microcalcifications and irregular margins. Which of the following is the most appropriate next step in diagnosis?
A 77-year-old man is brought to his primary care physician by his daughter. She states that lately, his speech has been incoherent. It seemed to have started a few weeks ago and has been steadily worsening. He is otherwise well; however, she notes that she has had to start him on adult diapers. The patient has a past medical history of hypertension, hyperlipidemia, and type 2 diabetes mellitus. He has been smoking 1 pack of cigarettes per day for over 40 years. His temperature is 98.9°F (37.2°C), blood pressure is 167/108 mmHg, pulse is 83/min, respirations are 12/min, and oxygen saturation is 97% on room air. Physical exam reveals a confused elderly man who does not respond coherently to questions. Cardiac and pulmonary exam is within normal limits. Inspection of the patient's scalp reveals a healing laceration which the daughter claims occurred yesterday when he fell while walking. Gait testing is significant for the patient taking short steps with reduced cadence. Which of the following findings is most likely in this patient?
A 56-year-old woman is brought to the emergency department by her husband because of slurred speech and left facial droop for the past 30 minutes. During this period, she has also had numbness on the left side of her face. She has never had such an episode before. She has hypertension, hypercholesterolemia, and type 2 diabetes mellitus. Her father died of lung cancer 1 week ago. The patient has smoked one pack of cigarettes daily for 30 years. She drinks one glass of wine daily. Her current medications include metformin, sitagliptin, enalapril, and atorvastatin. She is 168 cm (5 ft 6 in) tall and weighs 86 kg (190 lb); BMI is 30.5 kg/m2. She is oriented to time, place, and person. Her temperature is 37°C (98.7°F), pulse is 97/min, and blood pressure is 140/90 mm Hg. Examination shows drooping of the left side of the face. Her speech is clear. Examination shows full muscle strength. Deep tendon reflexes are 2+ bilaterally. A finger-nose test and her gait are normal. Cardiopulmonary examination shows a right-sided carotid bruit. A complete blood count and serum concentrations of creatinine, glucose, and electrolytes are within the reference ranges. An ECG shows left ventricular hypertrophy. A noncontrast CT scan of the brain shows no abnormalities. On the way back from the CT scan, her presenting symptoms resolve. Which of the following is the most likely diagnosis?
A 71-year-old Caucasian male presents to your office with bloody diarrhea and epigastric pain that occurs 30 minutes after eating. He has lost 15 pounds in 1 month, which he attributes to fear that the pain will return following a meal. He has a history of hyperlipidemia and myocardial infarction. Physical exam and esophagogastroduodenoscopy are unremarkable. What is the most likely cause of this patient's pain?
A 24-year-old woman comes to the physician because of pain and swelling of her left leg over the past 24 hours. The pain is worse while walking and improves when resting. Seven months ago, she was diagnosed with a pulmonary embolism and was started on warfarin. Anticoagulant therapy was discontinued 1 month ago. Her sister has systemic lupus erythematosus. The patient does not smoke. She currently takes no medications. Her temperature is 37.8°C (100°F), pulse is 78/min, and blood pressure is 123/72 mm Hg. On physical examination, the left calf is diffusely erythematous, swollen, and tender. Dorsal flexion of the left foot elicits pain. Cardiopulmonary examination shows no abnormalities. On duplex ultrasonography, the left popliteal vein is not compressible. Laboratory studies show an elevated serum concentration of D-dimer and insensitivity to activated protein C. Further examination is most likely to show which of the following?
The rapid response team is called for a 74-year-old woman on an inpatient surgical floor for supraventricular tachycardia. The patient had surgery earlier in the day for operative management of a femur fracture. The patient has a history of hypertension, atherosclerosis, type 2 diabetes, and uterine cancer status post total abdominal hysterectomy 20 years prior. With carotid massage, valsalva maneuvers, and metoprolol, the patient breaks out of her supraventricular tachycardia. Thirty minutes later, the nurse notices a decline in the patient’s status. On exam, the patient has a temperature of 98.4°F (36.9°C), blood pressure of 102/74 mmHg, pulse of 86/min, and respirations are 14/min. The patient is now dysarthric with noticeable right upper extremity weakness of 2/5 in elbow flexion and extension. All other extremities demonstrate normal strength and sensation. Which of the following most likely contributed to this decline?
A 38-year-old man with a history of hypertension presents to his primary care physician for a headache and abdominal pain. His symptoms began approximately 1 week ago and have progressively worsened. He describes his headache as pressure-like and is mildly responsive to ibuprofen. His abdominal pain is located in the bilateral flank area. His hypertension is poorly managed with lifestyle modification and chlorthalidone. He had 1 urinary tract infection that was treated with ciprofloxacin approximately 6 months ago. He has a home blood pressure monitor, where his average readings are 155/95 mmHg. Family history is significant for his father expiring secondary to a myocardial infarction and his history was complicated by refractory hypertension and end-stage renal disease. His vital signs are significant for a blood pressure of 158/100 mmHg. Physical examination is notable for bilateral flank masses. Laboratory testing is significant for a creatinine of 3.1 mg/dL. Urinalysis is remarkable for hematuria and proteinuria. Which of the following will this patient most likely be at risk for developing?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
