Internal Medicine
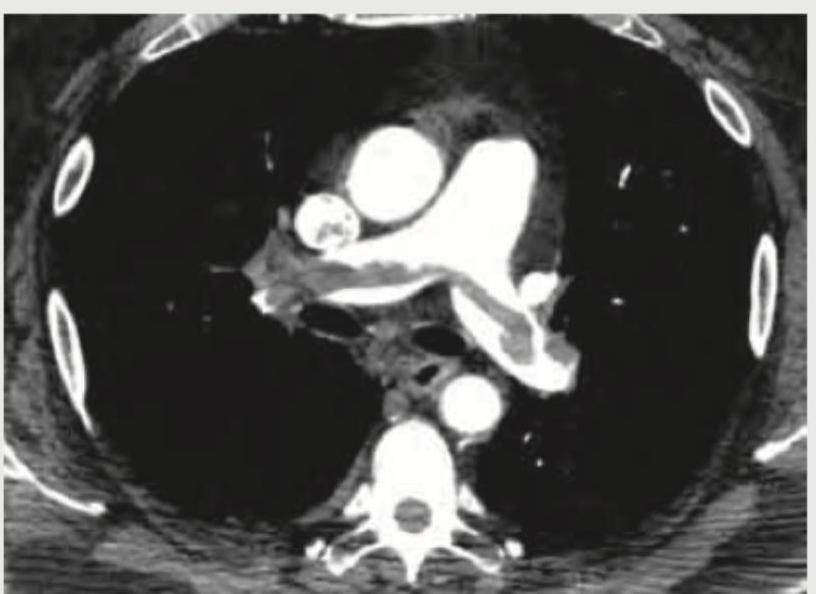
1 questionsA 35-year-old male with history of 4 weeks of immobilization for fracture of femur develops sudden onset breathlessness and blood in sputum. CT angiography shows? (Recent NEET Pattem 2018-19)
Pathology
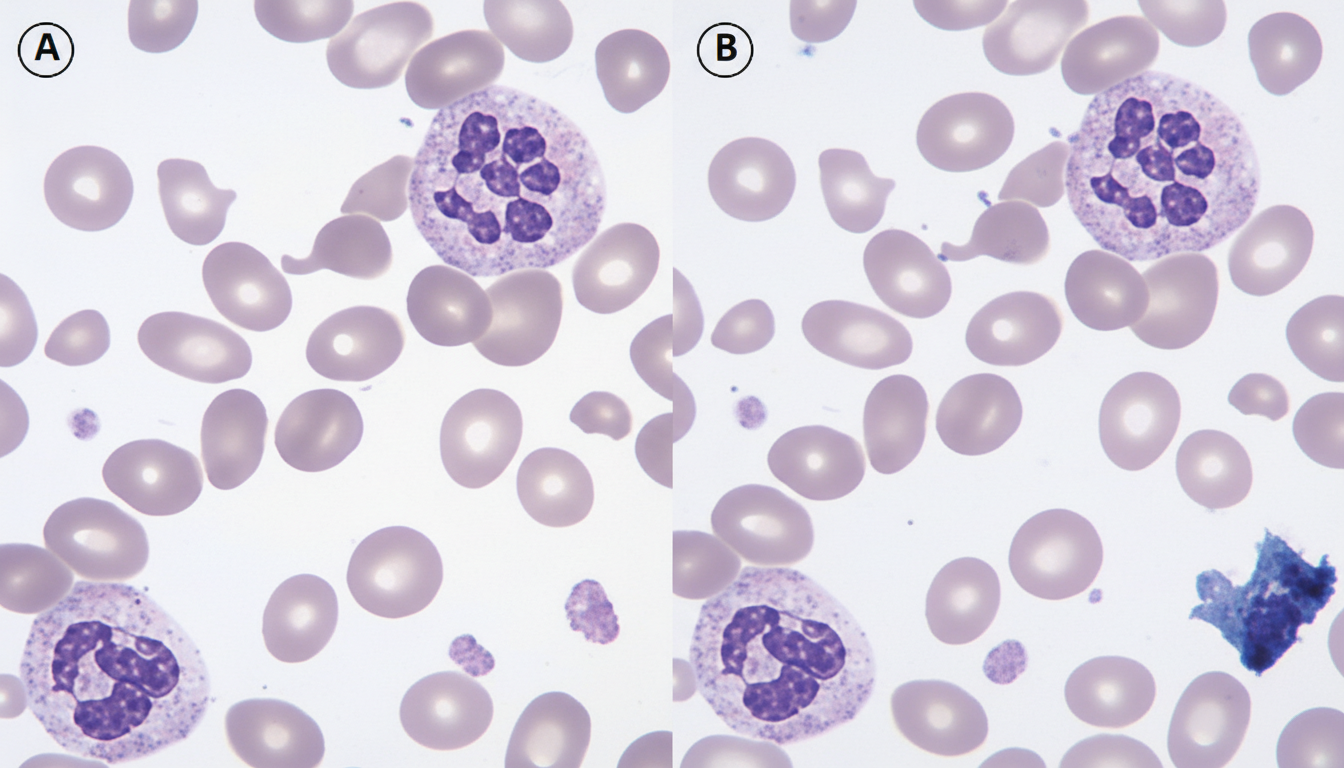
5 questionsWhich of the following hematological condition is shown below?
Hysterectomy specimen from a 40-year-old lady is shown along with histology slide. The diagnosis is:
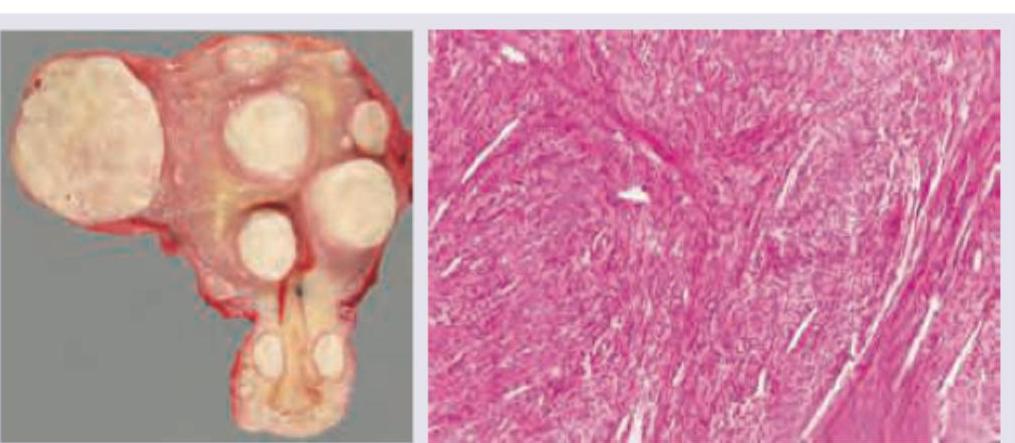
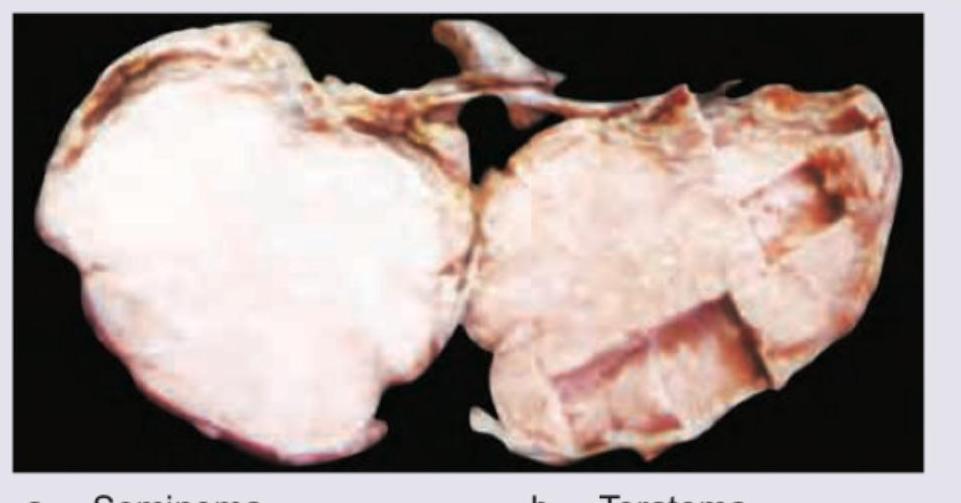
The following is a post-orchidectomy histopathological specimen. Diagnosis is:
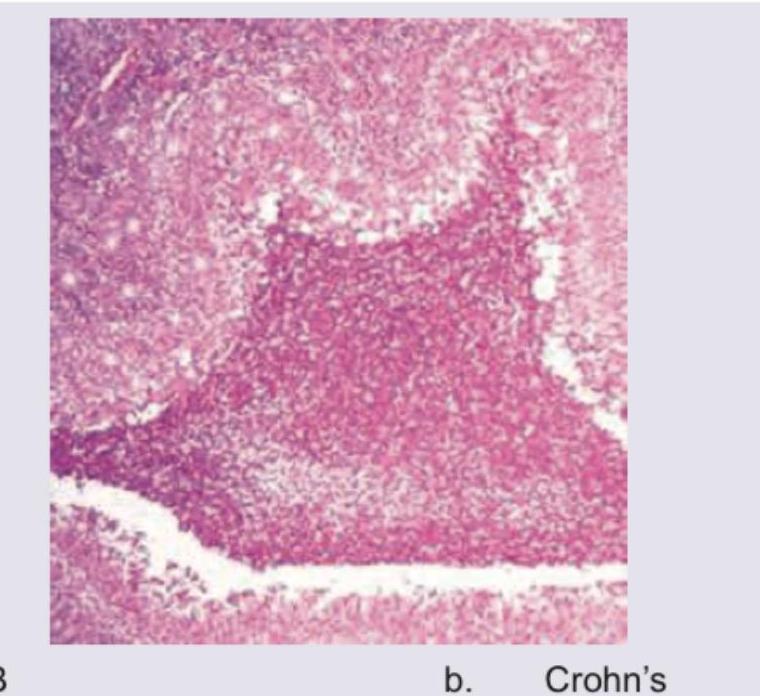
The image shows a histological section of intestinal tissue with a granuloma. What is the most likely diagnosis?
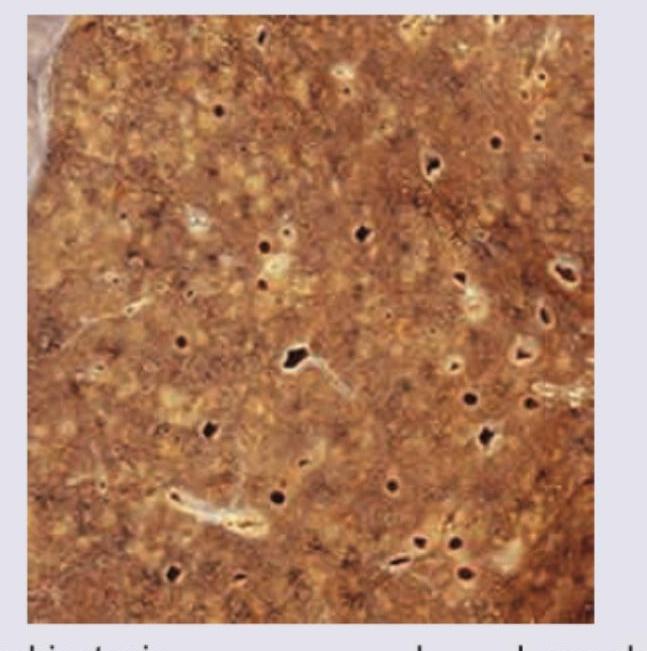
A 40-year-old man underwent lung transplantation. The resected lung specimen is shown below. Comment on the diagnosis.
Pediatrics
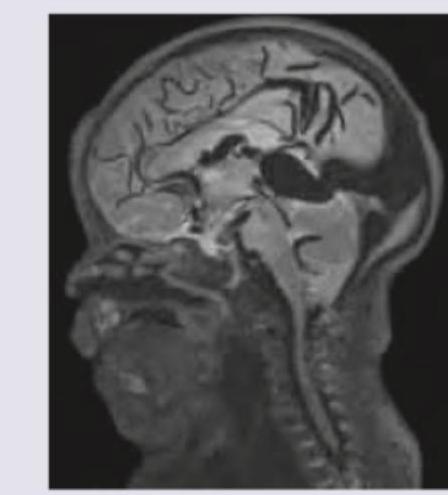
1 questionsA 6 month infant was brought with complaints of a failure to gain weight and a large head. On examination, increased head circumference, bounding pulses and features of heart failure were noted. On cranial auscultation loud cranial bruit was heard. MRI head shows? (Recent NEET Pattern 2018-19)
Radiology
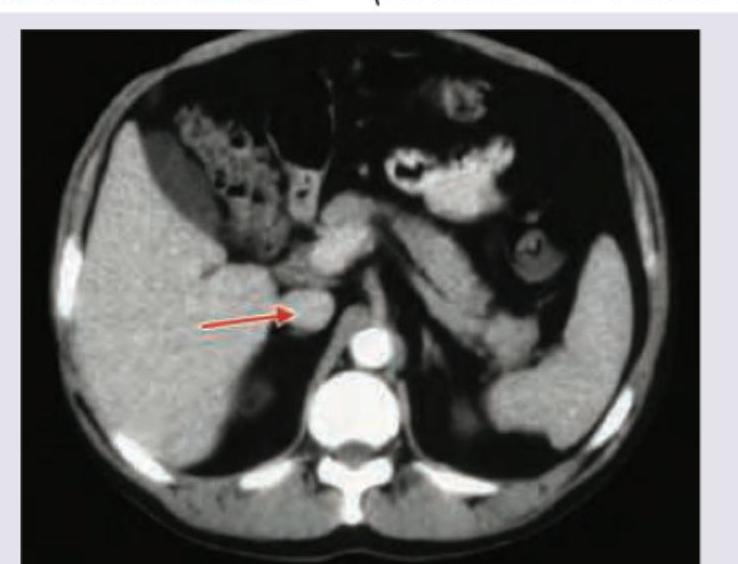
3 questionsIdentify the marked structure in the CT abdomen section shown below? (Recent NEET Pattern 2018-19)
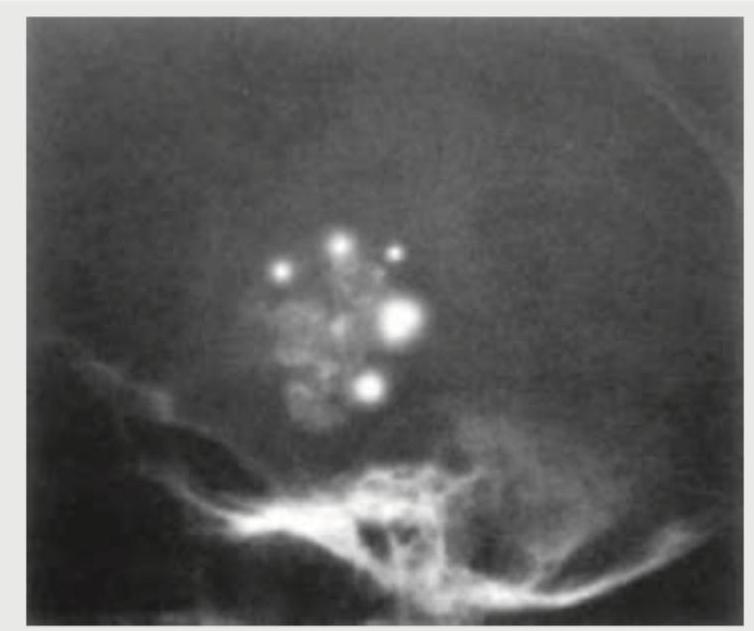
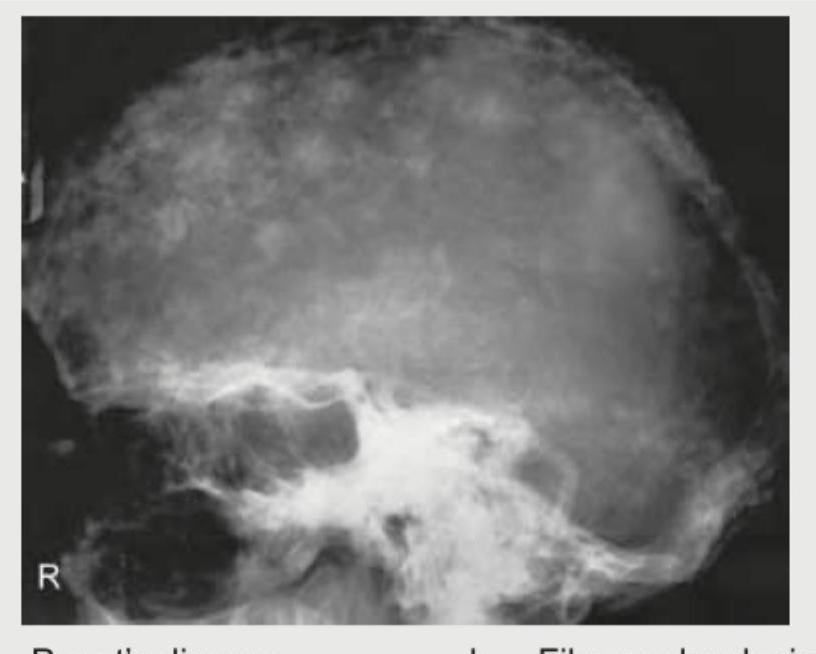
A 65-year-old man presents with bone pains. X-ray Skull shows? (Recent NEET Pattem 2018-19)
A 9-year-old female child presents with history of headache and visual disturbances. X-Ray skull is shown below. What is the possible diagnosis? (Recent NEET Pattern 2018-19)