What is the most common feature of sarcoidosis on chest X-ray?
Radiological sign in case of Perthes disease?
Which of the following conditions is the MOST COMMON cause of rib notching?
What is an X-ray artifact?
Frequency of ultrasound waves in USG -
Gyromagnetic property of proton is seen in -
For pericardial calcifications, which is the best investigation?
Barium swallow is used for -
"String of beads" appearance on horizontal abdominal view X-ray is suggestive of:
What condition is indicated by the double bubble sign on an abdominal X-ray?
NEET-PG 2013 - Radiology NEET-PG Practice Questions and MCQs
Question 21: What is the most common feature of sarcoidosis on chest X-ray?
- A. Bilateral hilar lymphadenopathy (Correct Answer)
- B. Cavitation
- C. Pleural effusion
- D. Reticular opacities
Explanation: ***Bilateral hilar lymphadenopathy*** - **Bilateral hilar lymphadenopathy** is the hallmark radiological feature of sarcoidosis, seen in over 75% of cases. - This finding, often symmetrical, represents the accumulation of **non-caseating granulomas** in the lymph nodes. - Classic presentation in **Stage I and Stage II** sarcoidosis. *Pleural effusion* - **Pleural effusions** are uncommon in sarcoidosis, occurring in less than 5% of cases. - When present, they are usually small and unilateral, and their presence should prompt consideration of alternative diagnoses. *Cavitation* - **Cavitation** is a rare manifestation of sarcoidosis and is more characteristic of infectious processes like **tuberculosis** or certain fungal infections. - If seen, it usually suggests severe parenchymal involvement or superimposed infection. *Reticular opacities* - While **reticular opacities** (interstitial changes) can be seen in later stages of sarcoidosis, representing **pulmonary fibrosis**, they are not the *most common* initial finding. - These opacities indicate chronic disease progression (Stage III/IV) rather than the initial presentation.
Question 22: Radiological sign in case of Perthes disease?
- A. Flattening of femoral head (Correct Answer)
- B. Fragmentation of femoral head epiphysis
- C. Lateral femoral head displacement
- D. Limited hip abduction
Explanation: ***Flattening of femoral head*** - **Flattening** and **fragmentation** of the femoral head are characteristic radiological findings in **early-stage** Perthes disease. - This flattening is a direct consequence of the **avascular necrosis** and subsequent **remodeling** of the femoral epiphysis. *Fragmentation of femoral head epiphysis* - While **fragmentation** is a key feature of Perthes disease, it's typically observed **after** the initial flattening and sclerosis in the avascular stage. - It represents the process of **resorption** and **revascularization** as the bone attempts to heal. *Lateral femoral head displacement* - **Lateral displacement** of the femoral head is a more common finding in conditions like **slipped capital femoral epiphysis (SCFE)**, where the epiphysis slips from the metaphysis. - In Perthes disease, the primary issue is the **necrosis and collapse** of the femoral head itself, rather than displacement from the neck. *Limited hip abduction* - **Limited hip abduction** is a clinical sign, not a radiological sign, and it is a common symptom in Perthes disease due to pain, inflammation, and deformity of the femoral head. - Radiological signs are visual abnormalities observed on imaging studies like X-rays.
Question 23: Which of the following conditions is the MOST COMMON cause of rib notching?
- A. Coarctation of aorta (Correct Answer)
- B. Atrial septal defect
- C. Chronic superior venacava obstruction
- D. Congenital interruption of aorta
Explanation: ***Coarctation of aorta*** - **Coarctation of the aorta** is the classic and **most common cause** of rib notching. - The notching is caused by the enlargement and tortuosity of the **intercostal arteries** as they provide collateral circulation to bypass the narrowed aorta. *Chronic superior venacava obstruction* - Chronic superior vena cava (SVC) obstruction may lead to the development of collateral circulation through the azygos and hemiazygos veins, but it does **not typically cause rib notching**. - Rib notching is specifically related to collateral flow bypassing an aortic obstruction, not a venous obstruction. *Atrial septal defect* - An **atrial septal defect (ASD)** is a communication between the atria that can lead to right heart volume overload and pulmonary hypertension. - While it's a congenital heart defect, an ASD does **not cause rib notching** as it does not involve an obstruction of systemic arterial flow requiring collateral circulation via the intercostal arteries. *Congenital interruption of aorta* - While **congenital interruption of the aorta** also involves an aortic obstruction, it is a **much rarer condition** than coarctation of the aorta. - Due to its rarity, it is not considered the most common cause of rib notching, even though it would theoretically lead to similar collateral vessel formation.
Question 24: What is an X-ray artifact?
- A. A radiographic finding that indicates disease pathology
- B. A normal anatomical structure visible on X-ray
- C. An image distortion produced when the patient moves during the X-ray procedure
- D. An unwanted image distortion that doesn't represent actual anatomy (Correct Answer)
Explanation: ***An unwanted image distortion that doesn't represent actual anatomy*** - An **X-ray artifact** is any feature or distortion on a radiographic image that is not present in the actual object being imaged. - These can arise from various sources such as patient movement, equipment malfunction, or improper technique, leading to **misinterpretation** of the image. - Artifacts are unwanted findings that can obscure true pathology or mimic disease. *A normal anatomical structure visible on X-ray* - This describes a **true anatomical finding**, which is the intended purpose of an X-ray. - Normal anatomical structures are expected and assist in diagnosis, unlike artifacts which obscure or mimic pathology. *An image distortion produced when the patient moves during the X-ray procedure* - While **patient motion** is a common cause of X-ray artifacts, this describes just one specific type (motion artifact), not a comprehensive definition of what an artifact is. - Other sources like metallic objects, scatter radiation, or detector issues can also cause artifacts. *A radiographic finding that indicates disease pathology* - This describes **true pathology** or disease findings, which is what radiologists aim to identify. - Artifacts are the opposite - they are false findings that do not represent actual anatomy or pathology.
Question 25: Frequency of ultrasound waves in USG -
- A. 2000 Hz
- B. 5000 Hz
- C. < 2 MHz
- D. >2 MHz (Correct Answer)
Explanation: ***>2 MHz*** - Medical diagnostic ultrasound typically uses frequencies in the **range of 2-15 MHz**, with some applications extending from 1-20 MHz. - Frequencies **above 2 MHz** are considered the standard for diagnostic ultrasonography, providing adequate **spatial resolution** and tissue penetration for imaging internal structures. - **Frequency selection** depends on the application: - **2-5 MHz**: Deep structures (abdominal, obstetric imaging) - better penetration - **5-10 MHz**: Vascular studies, cardiac imaging - **7-15 MHz**: Superficial structures (thyroid, breast, musculoskeletal) - better resolution - Higher frequencies provide better resolution but less penetration; the choice represents a trade-off based on clinical needs. *2000 Hz* - This frequency (2 kHz) falls within the **audible range** for humans (20 Hz to 20 kHz). - Such low frequencies would not provide the necessary **spatial resolution** for diagnostic imaging and lack the characteristics needed for medical ultrasound. *5000 Hz* - At 5 kHz, this is still within the **audible frequency range**. - These frequencies are far too low for medical ultrasound imaging, which requires **megahertz frequencies** to generate diagnostically useful images with adequate detail. *< 2 MHz* - Frequencies below 2 MHz, while technically ultrasound (>20 kHz), are generally **below the diagnostic range** for most clinical applications. - Although lower frequencies offer better tissue penetration, frequencies below 2 MHz provide **insufficient spatial resolution** for standard diagnostic medical imaging.
Question 26: Gyromagnetic property of proton is seen in -
- A. MRI (Correct Answer)
- B. CT
- C. PET scan
- D. USG
Explanation: ***MRI*** - Magnetic Resonance Imaging (MRI) relies on the **gyromagnetic properties of protons**, primarily hydrogen nuclei in water and fat. - These protons align with a strong magnetic field and, when pulsed with radiofrequency waves, emit detectable signals that form the image. *CT* - Computed Tomography (CT) utilizes **X-rays** and their differential absorption by various tissues to create cross-sectional images. - It does not involve the gyromagnetic properties of protons. *PET scan* - Positron Emission Tomography (PET) scans detect **gamma rays** emitted from radiotracers, typically radionuclides like Fluorine-18, that accumulate in metabolically active tissues. - This imaging modality is based on radioactive decay, not proton spin. *USG* - Ultrasonography (USG) generates images by sending **high-frequency sound waves** into the body and detecting the echoes that bounce back from various tissues. - It relies on acoustic properties and tissue interfaces, not magnetic properties of protons.
Question 27: For pericardial calcifications, which is the best investigation?
- A. Ultrasound
- B. CT scan (Correct Answer)
- C. MRI
- D. Transesophageal echocardiography
Explanation: ***Correct: CT scan*** - **CT scans** are highly sensitive and specific for detecting **pericardial calcifications** due to their excellent spatial resolution and ability to measure calcium density (Hounsfield units). - They provide detailed anatomical information about the **pericardium** and can accurately map the extent, location, and thickness of calcified areas. - **CT is the gold standard** for detecting and quantifying pericardial calcification, particularly in constrictive pericarditis. *Incorrect: Ultrasound* - While ultrasound (echocardiography) can visualize the pericardium and may detect calcifications, its ability to definitively identify and characterize **calcifications** is limited compared to CT. - **Acoustic shadowing** from calcifications can obscure underlying structures, making a precise assessment challenging. - Useful for detecting pericardial effusion and thickening, but not optimal for calcification assessment. *Incorrect: MRI* - **MRI excels** in visualizing soft tissues, pericardial inflammation, and fluid collections, but it is **poor at detecting calcium**. - Calcifications typically appear as signal voids (black) on MRI, making it difficult to differentiate them from other structures, air, or motion artifacts. - MRI is valuable for assessing pericardial inflammation and constriction but not the preferred method for calcification. *Incorrect: Transesophageal echocardiography* - TEE offers high-resolution images of cardiac structures and is primarily used for assessing valve function, intracardiac masses, endocarditis, and aortic pathology. - Its utility in detecting and characterizing **pericardial calcifications** is limited compared to CT, especially for diffuse or subtle calcifications. - The pericardium is not optimally visualized with TEE compared to transthoracic echocardiography.
Question 28: Barium swallow is used for -
- A. Colon
- B. Esophagus (Correct Answer)
- C. Duodenum
- D. Jejunum
Explanation: ***Esophagus*** - A **barium swallow** specifically visualizes the **esophagus**, pharynx, and sometimes the early stomach. - It's used to identify abnormalities like **dysphagia**, strictures, **achalasia**, or tumors by coating the mucosal lining. *Colon* - The colon is typically examined using a **barium enema**, where barium sulfate is administered rectally. - This procedure is effective for visualizing the large intestine for conditions like **polyps**, diverticula, or inflammatory bowel disease. *Duodenum* - While a barium swallow may transiently show the **duodenum**, its primary target is the esophagus and stomach. - More detailed imaging of the duodenum often requires an **upper GI series (UGI)**, which is a broader study of the upper digestive tract. *Jejunum* - The jejunum is part of the small intestine and is best visualized through a **small bowel follow-through (SBFT)** procedure. - This involves ingesting barium and taking serial X-rays as it progresses through the small bowel, to detect conditions like **Crohn's disease** or obstructions.
Question 29: "String of beads" appearance on horizontal abdominal view X-ray is suggestive of:
- A. Intussusception
- B. Sigmoid volvulus
- C. Small bowel obstruction (Correct Answer)
- D. Large bowel obstruction
Explanation: ***Small bowel obstruction*** - A "string of beads" appearance on a horizontal abdominal view X-ray refers to small gas bubbles trapped between the valvulae conniventes in a dilated small bowel loop. - This finding is highly suggestive of **complete small bowel obstruction**, particularly when accompanied by multiple air-fluid levels and dilated bowel loops. *Intussusception* - While it causes obstruction, intussusception usually appears as a **target sign** (doughnut sign) on ultrasound or a **meniscus sign** on barium enema, not a string of beads on plain X-ray. - Plain X-rays may show signs of **bowel obstruction**, but the string of beads is not characteristic. *Sigmoid volvulus* - Sigmoid volvulus is characterized by a **dilated loop of colon** forming an inverted U-shape, often described as a **coffee bean sign** or **omega sign**, on plain X-ray. - This involves the large bowel, and the "string of beads" specifically relates to gas in the small bowel. *Large bowel obstruction* - Large bowel obstruction typically presents with a **dilated colon** proximal to the obstruction and a collapsed distal colon, often with absent or minimal gas in the rectum and sigmoid. - While air-fluid levels can be present, the "string of beads" is a specific sign of gas within dilated small bowel loops, distinguishing it from most large bowel obstructions.
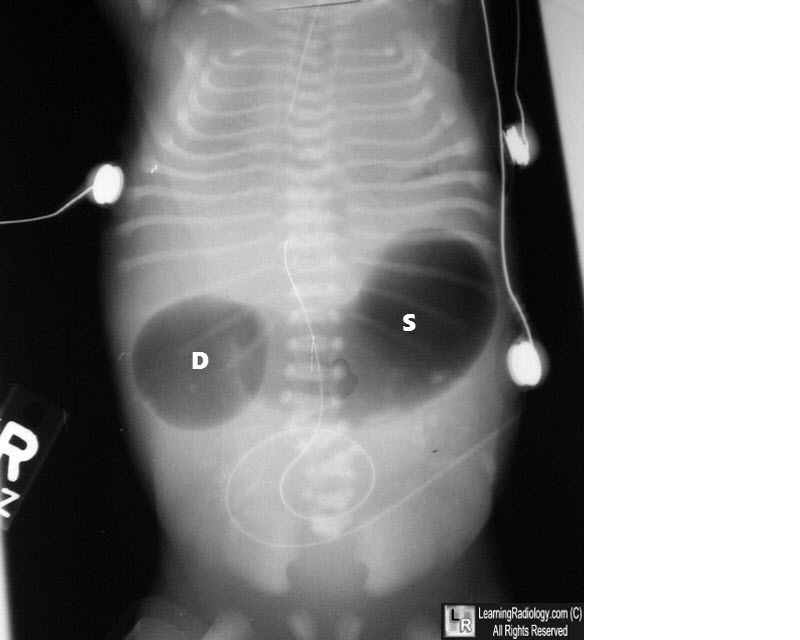
Question 30: What condition is indicated by the double bubble sign on an abdominal X-ray?
- A. Duodenal stenosis
- B. Volvulus
- C. All of the options
- D. Duodenal atresia (Correct Answer)
Explanation: ***Duodenal atresia*** - The **double bubble sign** on an abdominal X-ray is pathognomonic for **duodenal atresia**, characterized by two air-filled bubbles: one in the stomach and one in the proximal duodenum, separated by the pylorus. - This congenital anomaly results from a complete obstruction of the duodenum, preventing the passage of air and fluid past this point. *Duodenal stenosis* - While also an obstruction of the duodenum, **duodenal stenosis** is an incomplete obstruction, meaning some gas will pass beyond the duodenum. - This would result in gas being present in the distal bowel, which is not seen with a classic "double bubble" where the bowel distal to the duodenum is gasless. *Volvulus* - **Volvulus** involves the twisting of a loop of intestine, leading to obstruction and potentially ischemia. - While it can cause obstruction, it typically presents with a "corkscrew" appearance on an upper GI series or signs of diffuse bowel distension, not the isolated double bubble. *All of the options* - The double bubble sign is highly specific to **duodenal atresia** due to the complete obstruction it signifies. - Other conditions like duodenal stenosis and volvulus cause different radiological patterns, making this option incorrect.