Diagnostic Microbiology — MCQs

On this page
What condition is diagnosed using dark field microscopy, as illustrated in the accompanying color plate?
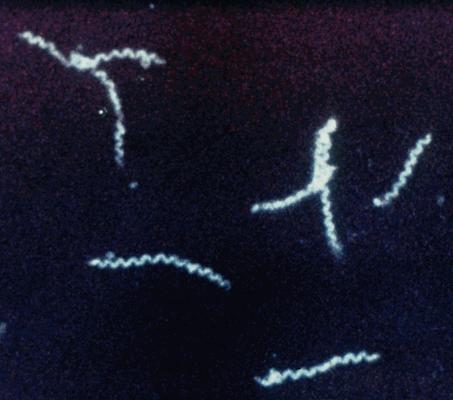
Toxoplasmosis in the fetus can be best confirmed by:
In the context of microbiological testing, stool specimens are transported in which of the following media?
Which medium is used for liquid culture of Mycobacterium tuberculosis?
When a surgeon wants to send an autopsy specimen for virological examination, the specimen should be preserved in:
Diagnosis of falciparum malaria is typically made by which of the following methods?
An advanced diagnostic technique that has been suggested as an alternative to culture methods is:
Which organism is detected using ELISA for virulence marker antigen (VMA)?
Selective media for Neisseria gonorrhoeae is:
Which of the following statements about the Widal test in typhoid fever is correct?
Practice by Chapter
Specimen Collection and Transport
Practice Questions
Microscopy in Microbiology
Practice Questions
Culture Methods and Media
Practice Questions
Bacterial Identification Techniques
Practice Questions
Antimicrobial Susceptibility Testing
Practice Questions
Serological Diagnosis
Practice Questions
Molecular Diagnostic Methods
Practice Questions
Rapid Diagnostic Tests
Practice Questions
Point-of-Care Testing
Practice Questions
Automation in Microbiology Laboratory
Practice Questions
Quality Control in Diagnostic Microbiology
Practice Questions
Interpretation of Microbiological Reports
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
