Diagnostic Microbiology — MCQs

On this page
Which of the following are acid-fast staining organisms? 1. Nocardia 2. Mycobacterium leprae 3. Actinomyces 4. Cryptosporidium parvum 5. Isospora belli
A 32 year old laborer working at a construction site presented with fever and hemoptysis. The sputum sample collected for examination showed the following. The smear will be stained by which of the following sequences?
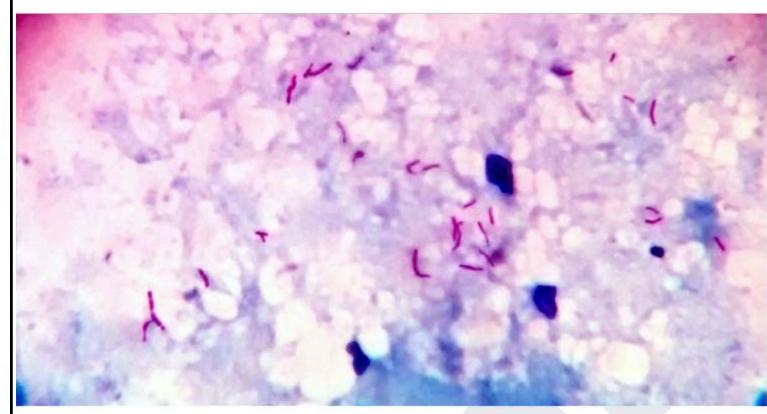
A sexually active adolescent presents with cervicitis. Which specimen collection method has the highest sensitivity for detecting N. gonorrhoeae?
Which of the following statements about nucleic acid amplification tests (NAATs) for STIs is FALSE?
What is the principle behind the FTA-ABS test?
A Gram stain from a pharyngeal membrane shows bacteria in 'Chinese letter' pattern with metachromatic granules. Which growth characteristic would confirm Corynebacterium diphtheriae?
A patient presents with suspected diphtheria. What media will be used to diagnose this condition?
Antemortem diagnosis of rabies is made with:
Auramine and rhodamine staining are used for:
Rapid examination of tubercle bacilli is possible with:
Practice by Chapter
Specimen Collection and Transport
Practice Questions
Microscopy in Microbiology
Practice Questions
Culture Methods and Media
Practice Questions
Bacterial Identification Techniques
Practice Questions
Antimicrobial Susceptibility Testing
Practice Questions
Serological Diagnosis
Practice Questions
Molecular Diagnostic Methods
Practice Questions
Rapid Diagnostic Tests
Practice Questions
Point-of-Care Testing
Practice Questions
Automation in Microbiology Laboratory
Practice Questions
Quality Control in Diagnostic Microbiology
Practice Questions
Interpretation of Microbiological Reports
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
