Diagnostic Microbiology — MCQs

On this page
Which is the most commonly used antigen detection test for Chlamydia trachomatis in genital specimens?
Which test is used to directly visualize Treponema pallidum in lesion exudate?
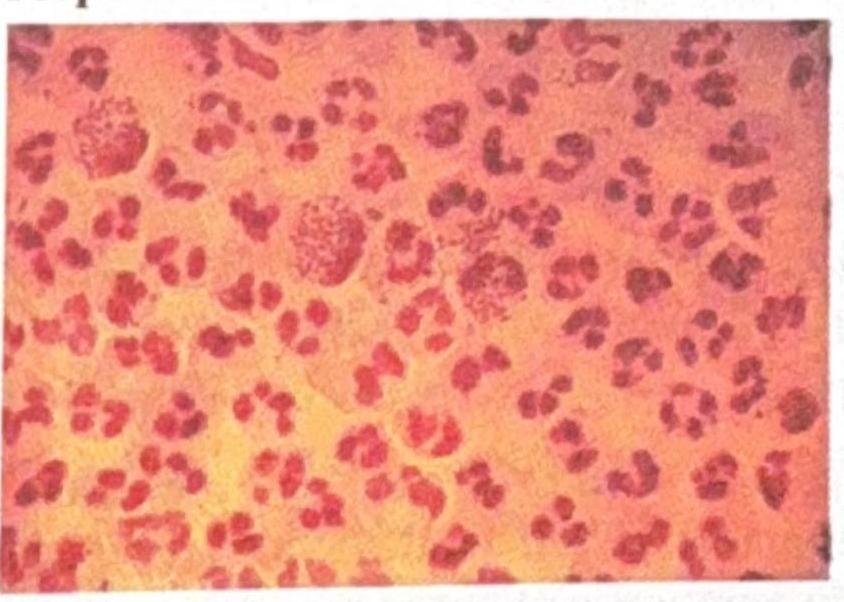
A man presents with dysuria and urethral discharge after a history of unprotected sex. The Gram stain of his discharge is shown. What is the best culture medium for isolating the organism responsible?
A female patient presents with dysuria and frequency. A coagulase-negative, novobiocin-resistant Staphylococcus species (>10^4 CFU/mL) was grown in urine culture. What does this indicate?
A frequent traveler presented with 4 days of continuous fever, abdominal pain, and bradycardia. What is the best diagnostic test to confirm the pathogen?
A child presented with bloody stools and abdominal pain. Which enrichment medium should be used for processing the fecal sample?
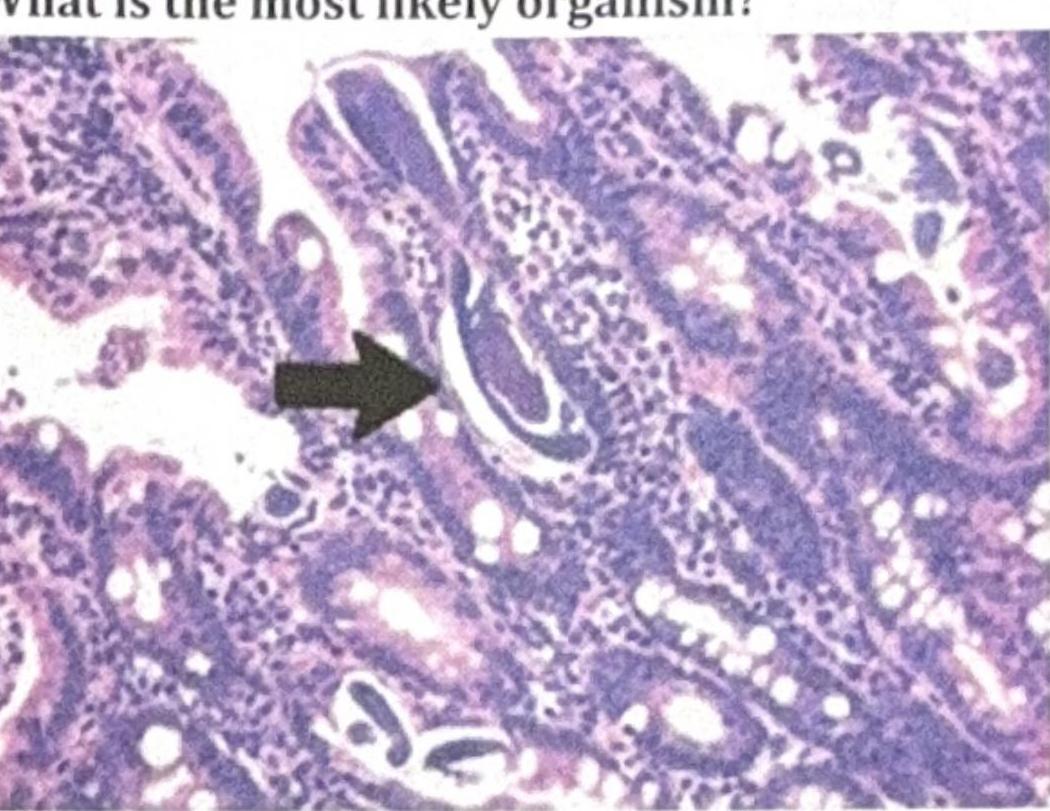
A patient on steroids presented with nocturnal cough and chronic urticaria. Bronchoalveolar lavage (BAL) staining was done, and the organism shown in the image was identified. What is the most likely organism?
A patient was suspected of having brucellosis. A serum sample was sent for a standard agglutination test, which was initially negative but became positive after dilution of the sample. What is the most likely reason for the initial negative test?
A truck driver presented with a painless, demarcated ulcer on the penis and inguinal lymphadenopathy. What is the best method to visualize the motility of the most likely causative agent?
On Ziehl-Neelsen (ZN) staining oocysts of size 8-10 µm are visible. Identify the organism.
Practice by Chapter
Specimen Collection and Transport
Practice Questions
Microscopy in Microbiology
Practice Questions
Culture Methods and Media
Practice Questions
Bacterial Identification Techniques
Practice Questions
Antimicrobial Susceptibility Testing
Practice Questions
Serological Diagnosis
Practice Questions
Molecular Diagnostic Methods
Practice Questions
Rapid Diagnostic Tests
Practice Questions
Point-of-Care Testing
Practice Questions
Automation in Microbiology Laboratory
Practice Questions
Quality Control in Diagnostic Microbiology
Practice Questions
Interpretation of Microbiological Reports
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
