Diagnostic Microbiology — MCQs

On this page
CSF gram stain of a child suffering with meningitis is shown below. What is the causative agent? (NEET Pattern 2019)
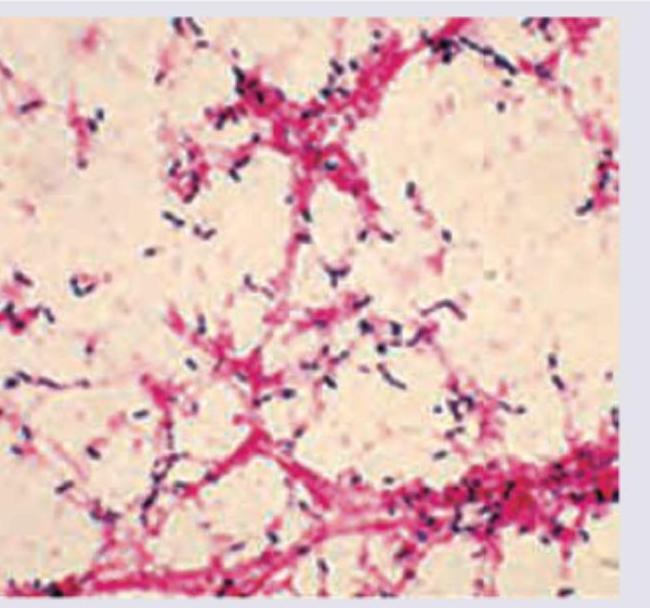
The following culture medium is used for the isolation of: (NEET Pattern 2019)

A wet mount preparation of vaginal discharge shows the following. Identify the organism responsible.
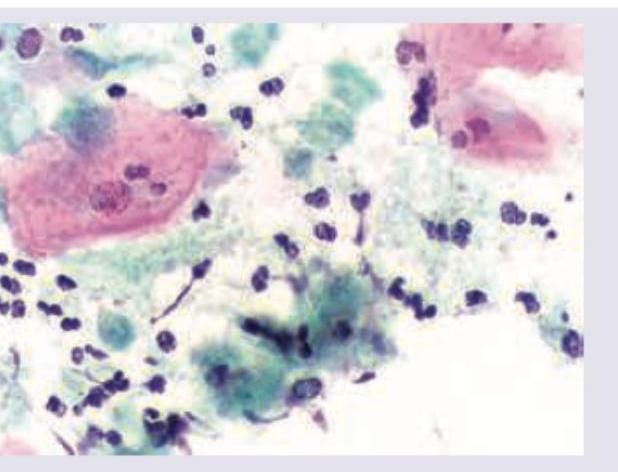
Two microscopic preparations of cerebrospinal fluid from a patient with meningitis are shown. Identify the stains used in images A and B.
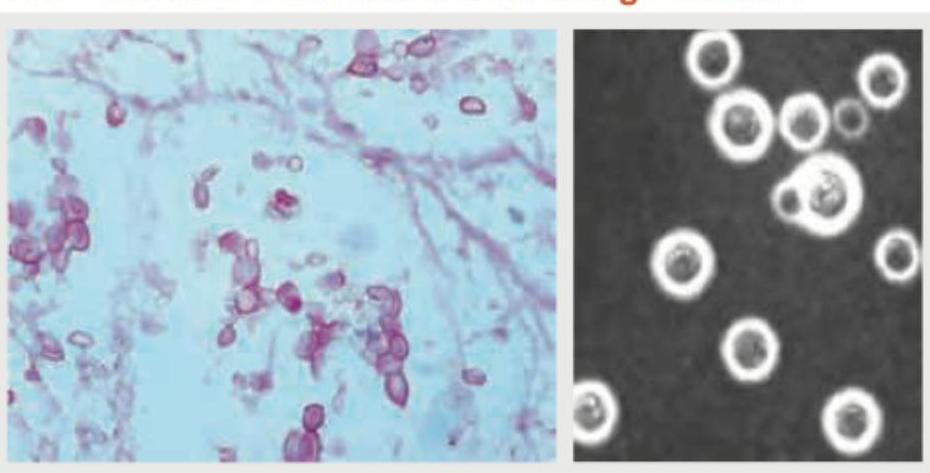
What is the most sensitive diagnostic method for detecting Trichomonas vaginalis?
What is the significance of prozone phenomenon in syphilis testing?
Which of the following specimens is most appropriate for Chlamydia trachomatis NAAT testing in men?
Which of the following is TRUE about screening for Trichomonas vaginalis?
Which serologic test for syphilis relies on flocculation reaction using cardiolipin-lecithin-cholesterol antigen?
Which of the following statements about non-treponemal tests for syphilis is NOT correct?
Practice by Chapter
Specimen Collection and Transport
Practice Questions
Microscopy in Microbiology
Practice Questions
Culture Methods and Media
Practice Questions
Bacterial Identification Techniques
Practice Questions
Antimicrobial Susceptibility Testing
Practice Questions
Serological Diagnosis
Practice Questions
Molecular Diagnostic Methods
Practice Questions
Rapid Diagnostic Tests
Practice Questions
Point-of-Care Testing
Practice Questions
Automation in Microbiology Laboratory
Practice Questions
Quality Control in Diagnostic Microbiology
Practice Questions
Interpretation of Microbiological Reports
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
