Bacteriology — MCQs

On this page
Which of the following is known as Preiz Nocard bacillus?
Which type of bacteria cannot survive in the absence of oxygen?
Which of the following is a catalase-negative, beta-hemolytic Streptococcus?
Which of the following are primarily human pathogenic bacteria?
Which bacterium possesses strains known as Et, Eh, and EP?
What is the most common organism causing upper respiratory tract infections in adults?
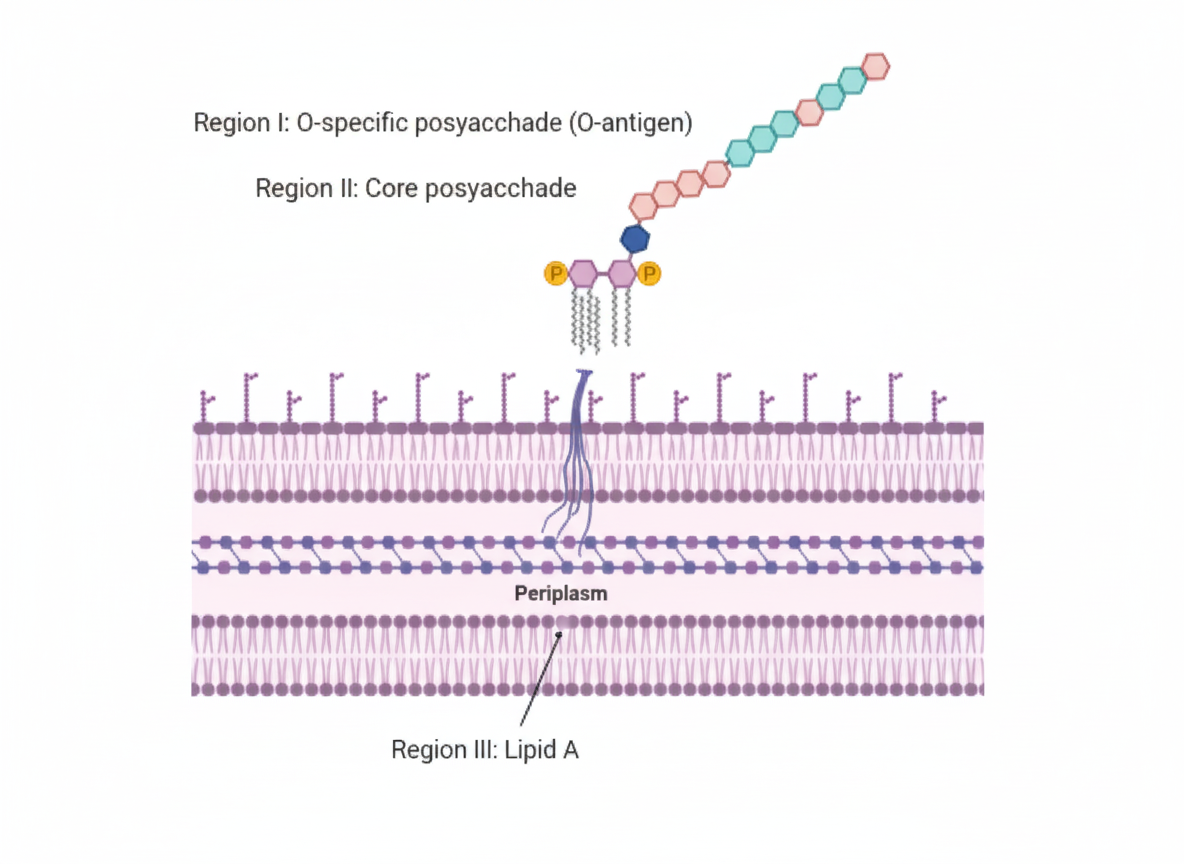
Which component of the bacterial cell wall is responsible for endotoxic activity?
What is the antibiotic of choice for streptococcal pharyngitis?
A couple, who did not know each other very well, dated and had sexual contact. Several weeks later, the man noticed a small, painless vesicle on his penis, which ruptured and then healed. Soon, his inguinal lymph nodes enlarged and discharged pus through multiple sinus tracts. Lymphogranuloma venereum (LGV) is a venereal disease caused by serotype L1, L2, or L3 of Chlamydia trachomatis. The differential diagnosis should include which of the following?
Which of the following is used as a biological indicator for control in plasma sterilization?
Practice by Chapter
Staphylococci
Practice Questions
Streptococci and Enterococci
Practice Questions
Neisseria and Moraxella
Practice Questions
Corynebacterium and Listeria
Practice Questions
Bacillus and Clostridium
Practice Questions
Enterobacteriaceae
Practice Questions
Vibrio, Aeromonas, and Plesiomonas
Practice Questions
Pseudomonas and Related Bacteria
Practice Questions
Haemophilus and HACEK Group
Practice Questions
Bordetella and Brucella
Practice Questions
Mycobacteria
Practice Questions
Spirochetes
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
