Bacteriology — MCQs

On this page
Which microorganisms are typically found in a lung abscess?
In a patient presenting with diarrhea and pus cells in stool, which of the following is LEAST likely to be the causative organism?
Primary tuberculosis most commonly involves which organ?
All of the following are true for non-typable strains of Haemophilus influenzae EXCEPT:
Which of the following bacteria shows this test positive?

What is the staining technique used here?
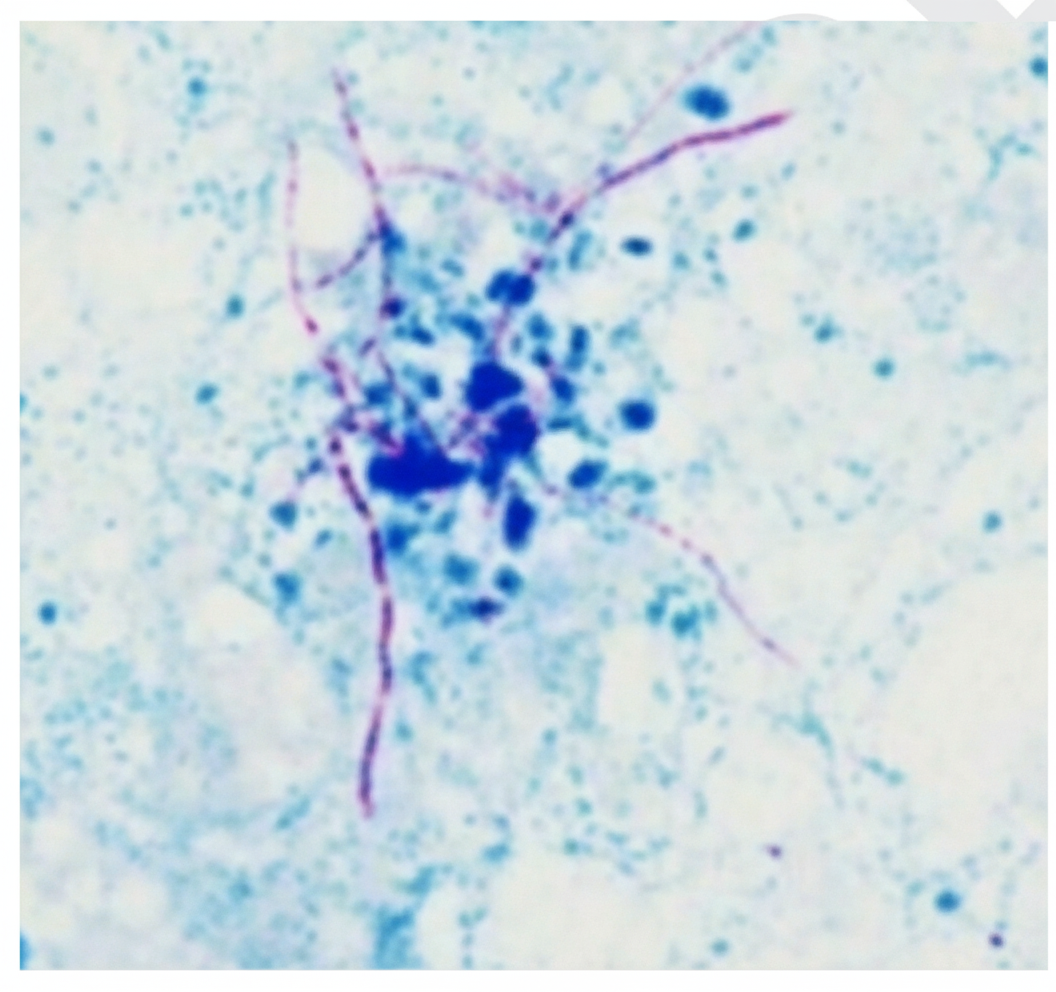
A rapid urea breath test is positive in which of the following infections?
Naegler's reaction is given by:
A 20-year-old male presents with abdominal pain and mild fever, followed by gastroenteritis. Stool examination reveals the presence of pus cells and red blood cells on microscopy. What is the most likely etiological agent responsible?
What inclusion bodies are present in lymphogranuloma venereum (LGV)?
Practice by Chapter
Staphylococci
Practice Questions
Streptococci and Enterococci
Practice Questions
Neisseria and Moraxella
Practice Questions
Corynebacterium and Listeria
Practice Questions
Bacillus and Clostridium
Practice Questions
Enterobacteriaceae
Practice Questions
Vibrio, Aeromonas, and Plesiomonas
Practice Questions
Pseudomonas and Related Bacteria
Practice Questions
Haemophilus and HACEK Group
Practice Questions
Bordetella and Brucella
Practice Questions
Mycobacteria
Practice Questions
Spirochetes
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
