Bacteriology — MCQs

On this page
What is the main constituent of the pneumococcal capsule?
Sulfur granules and multiple draining sinuses are a characteristic feature of which condition?
Which organism is NOT part of the HACEK group?
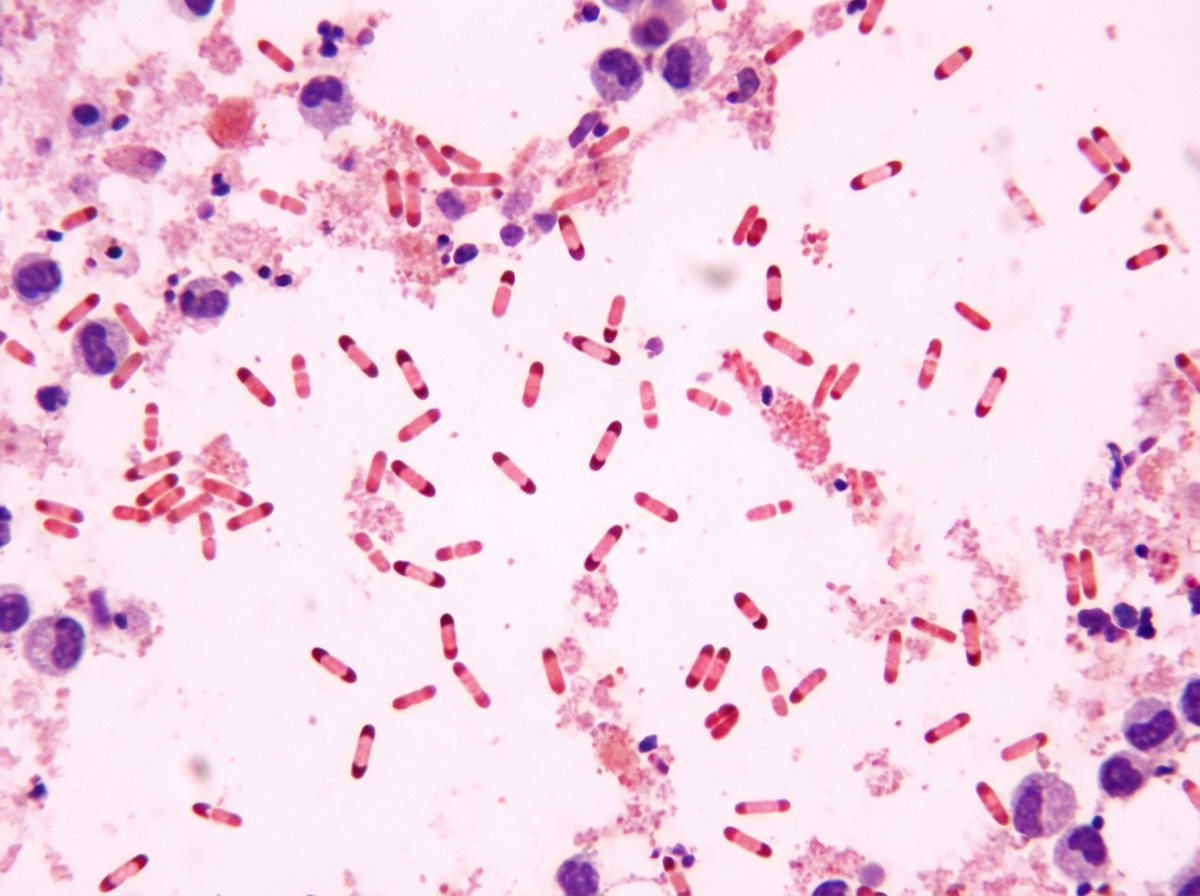
A 20-year-old male presented with left axillary pain, fever, malaise, and myalgias. On examination, there is a tender, boggy swelling in the left axilla with a hard core. A characteristic lesion was observed on the skin of the upper abdominal quadrant. Gram staining of the aspirate was performed. What is the drug of choice in the above condition?
Which of the following statements about H. pylori is NOT true?
Which bacterium exhibits motility differences according to temperature changes?
What substance is uniquely found in the cell wall of Gram-positive organisms and differentiates them from Gram-negative organisms?
Which of the following infections is caused by Rickettsia?
Clostridium difficile can be spread through all EXCEPT:
TCBS agar is used for the isolation of which bacterium?
Practice by Chapter
Staphylococci
Practice Questions
Streptococci and Enterococci
Practice Questions
Neisseria and Moraxella
Practice Questions
Corynebacterium and Listeria
Practice Questions
Bacillus and Clostridium
Practice Questions
Enterobacteriaceae
Practice Questions
Vibrio, Aeromonas, and Plesiomonas
Practice Questions
Pseudomonas and Related Bacteria
Practice Questions
Haemophilus and HACEK Group
Practice Questions
Bordetella and Brucella
Practice Questions
Mycobacteria
Practice Questions
Spirochetes
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
