Bacteriology — MCQs

On this page
On which medium is the earliest growth of diphtheria detected?
Kanagawa's phenomenon is seen in ?
What is the primary use of PLET medium in microbiology?
A militant presents with rashes all over his body sparing the palms and soles. On examination, he was febrile and lice were noted. Which of the following is responsible for his condition?
Identify the following bacterium from the image.

Which organism is responsible for causing Lymphogranuloma venereum (LGV)?
A 6-year-old boy presents with fever and chills, cough, rapid breathing, difficulty breathing, and chest pain. A culture from a respiratory sample shows Gram-positive bacteria. What is the most likely organism causing this infection?
Which of the following cell components produced by Neisseria gonorrhoeae is responsible for attachment to host cells?
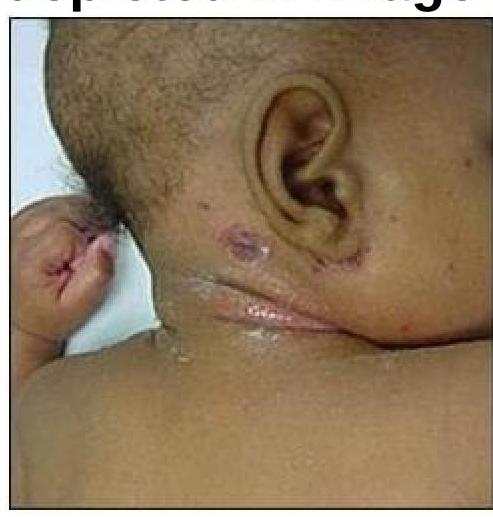
What is the causative organism for the condition depicted in the image?
Which of the following does not possess superantigen properties?
Practice by Chapter
Staphylococci
Practice Questions
Streptococci and Enterococci
Practice Questions
Neisseria and Moraxella
Practice Questions
Corynebacterium and Listeria
Practice Questions
Bacillus and Clostridium
Practice Questions
Enterobacteriaceae
Practice Questions
Vibrio, Aeromonas, and Plesiomonas
Practice Questions
Pseudomonas and Related Bacteria
Practice Questions
Haemophilus and HACEK Group
Practice Questions
Bordetella and Brucella
Practice Questions
Mycobacteria
Practice Questions
Spirochetes
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
