Bacteriology — MCQs

On this page
Chlamydia causes all except:
Which of the following statements are true regarding Legionella, EXCEPT?
A girl from Shimla presented to OPD with fever, hypotension, malaise and axillary and inguinal lymphadenopathy. Culture in glucose broth shows stalactite growth. Most likely causative organism is?
What is the generation time for *M. tuberculosis*?
All of the following organisms cause gastroenteritis within 6 hours, EXCEPT:
True about lepra bacilli is
Which of the following is the aetiological agent most often associated with Epiglottitis in children -
A person working in an abattoir presented with malignant pustule on hand. What is the causative agent?
Vital staining technique is used to demonstrate:
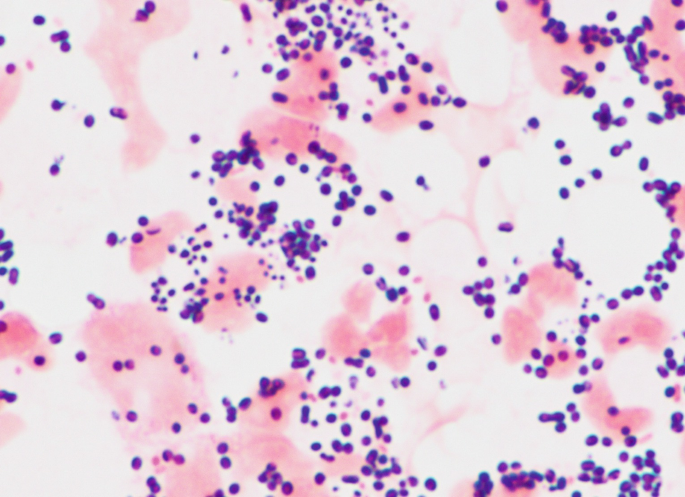
A 9 years old child presented to OPD with complaints of high grade fever, vomiting, one episode of seizure. CSF examination was done and Gram staining of the culture showed the following finding. What is the probable causative agent?
Practice by Chapter
Staphylococci
Practice Questions
Streptococci and Enterococci
Practice Questions
Neisseria and Moraxella
Practice Questions
Corynebacterium and Listeria
Practice Questions
Bacillus and Clostridium
Practice Questions
Enterobacteriaceae
Practice Questions
Vibrio, Aeromonas, and Plesiomonas
Practice Questions
Pseudomonas and Related Bacteria
Practice Questions
Haemophilus and HACEK Group
Practice Questions
Bordetella and Brucella
Practice Questions
Mycobacteria
Practice Questions
Spirochetes
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
