Bacteriology — MCQs

On this page
The causative organism of Chancroid is
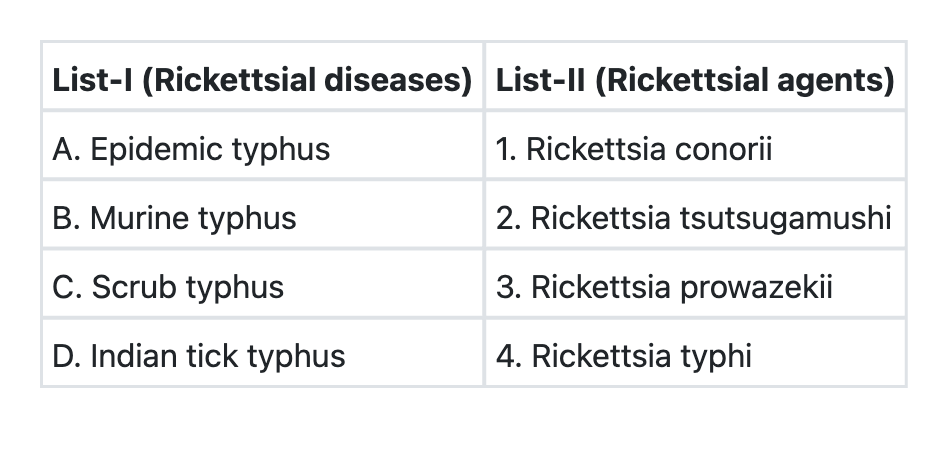
Match List-I with List-II and select the correct answer using the code given below the Lists:
Which of the following cause/causes bacterial vaginosis? 1. Gardnerella 2. Mycoplasma hominis 3. Ureaplasma urealyticum Select the correct answer using the code given below:
A surgeon told the patient’s attendant that his patient has “flesh eating bug” which is the cause of such severe infection in his dirty wound on his lower limb. Which organism was the surgeon referring to?
The most common organism causing Acute Otitis media in children is:
A 27-year-old man presents with clear urethral discharge and dysuria for 3 days. Gram stain shows numerous polymorphonuclear leukocytes without intracellular diplococci. What is the most likely pathogen?
What mechanism accounts for the neuroinvasive potential of Treponema pallidum?
Which structure of Treponema pallidum is responsible for its characteristic motility?
Which organism causes Granuloma inguinale (Donovanosis)?
What structure of Neisseria gonorrhoeae is primarily responsible for its pathogenicity?
Practice by Chapter
Staphylococci
Practice Questions
Streptococci and Enterococci
Practice Questions
Neisseria and Moraxella
Practice Questions
Corynebacterium and Listeria
Practice Questions
Bacillus and Clostridium
Practice Questions
Enterobacteriaceae
Practice Questions
Vibrio, Aeromonas, and Plesiomonas
Practice Questions
Pseudomonas and Related Bacteria
Practice Questions
Haemophilus and HACEK Group
Practice Questions
Bordetella and Brucella
Practice Questions
Mycobacteria
Practice Questions
Spirochetes
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
