Bacteriology — MCQs

On this page
Which of the following bacteria has the flagellar characteristic shown in the image?
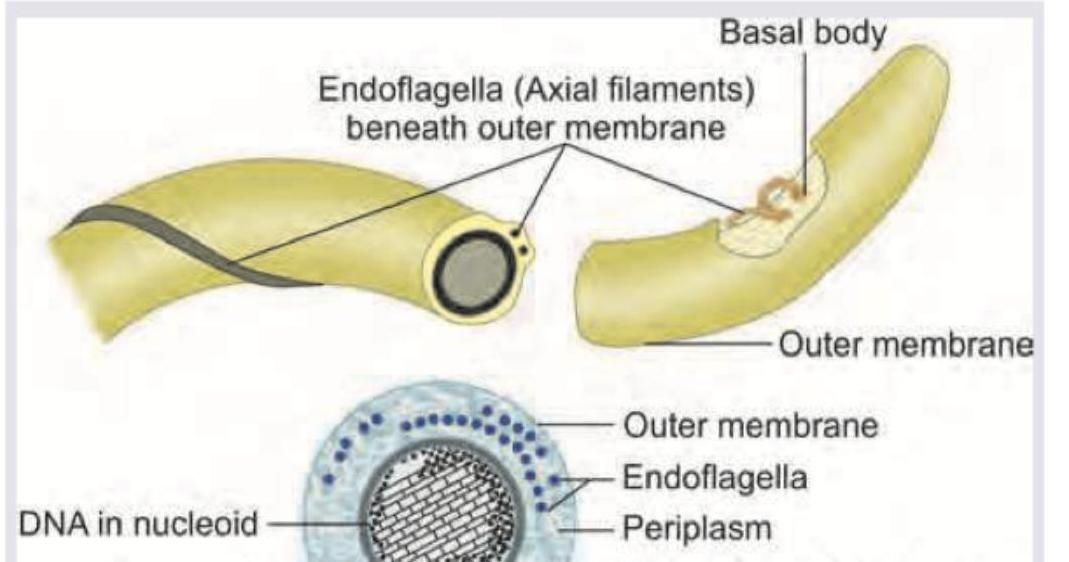
A 13-year-old girl with cystic fibrosis has been having recurrent severe respiratory infections and transtracheal aspirate was sent for culture. The growth of pink colonies in the image shows presence of:
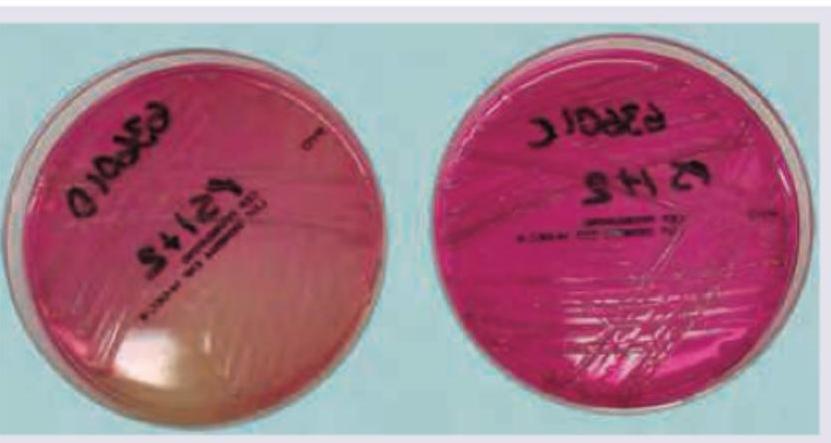
All are true about Helicobacter pylori on special stain preparation of stomach except:
Which one of the following is the causative organism of Erythrasma, a mild, localized and superficial skin infection?
Gas Gangrene resulting in crepitus in tissues and a sweet smelling brown exudate is caused due to infection by :
Which one of the following statements regarding Gas Gangrene Infection is correct?
Clinical signs and symptoms in tetanus are a result of
Which one of the following organisms is not associated with synergistic gangrene?
Donovan bodies are associated with :
The pathogenic organism responsible for the causation of Donovaniasis is
Practice by Chapter
Staphylococci
Practice Questions
Streptococci and Enterococci
Practice Questions
Neisseria and Moraxella
Practice Questions
Corynebacterium and Listeria
Practice Questions
Bacillus and Clostridium
Practice Questions
Enterobacteriaceae
Practice Questions
Vibrio, Aeromonas, and Plesiomonas
Practice Questions
Pseudomonas and Related Bacteria
Practice Questions
Haemophilus and HACEK Group
Practice Questions
Bordetella and Brucella
Practice Questions
Mycobacteria
Practice Questions
Spirochetes
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
