Bacteriology — MCQs

On this page
Which of the following statements regarding gullwing-shaped bacteria is FALSE?
Staphylococcus aureus produces a superantigen that contributes to massive cytokine release and polyclonal T-cell activation. Which of the following best fits this description of a superantigen?
Buffered charcoal yeast extract agar is a selective medium for which bacterium?
Inspissation is used for?
All of the following statements regarding Clostridium tetani are true, except?
Which of the following statements about Gram-positive cocci is false?
Which of the following statements regarding L-forms of bacteria is FALSE?
All of the following bacteria show bipolar staining except?
Coagulase-negative staphylococci includes all of the following except?
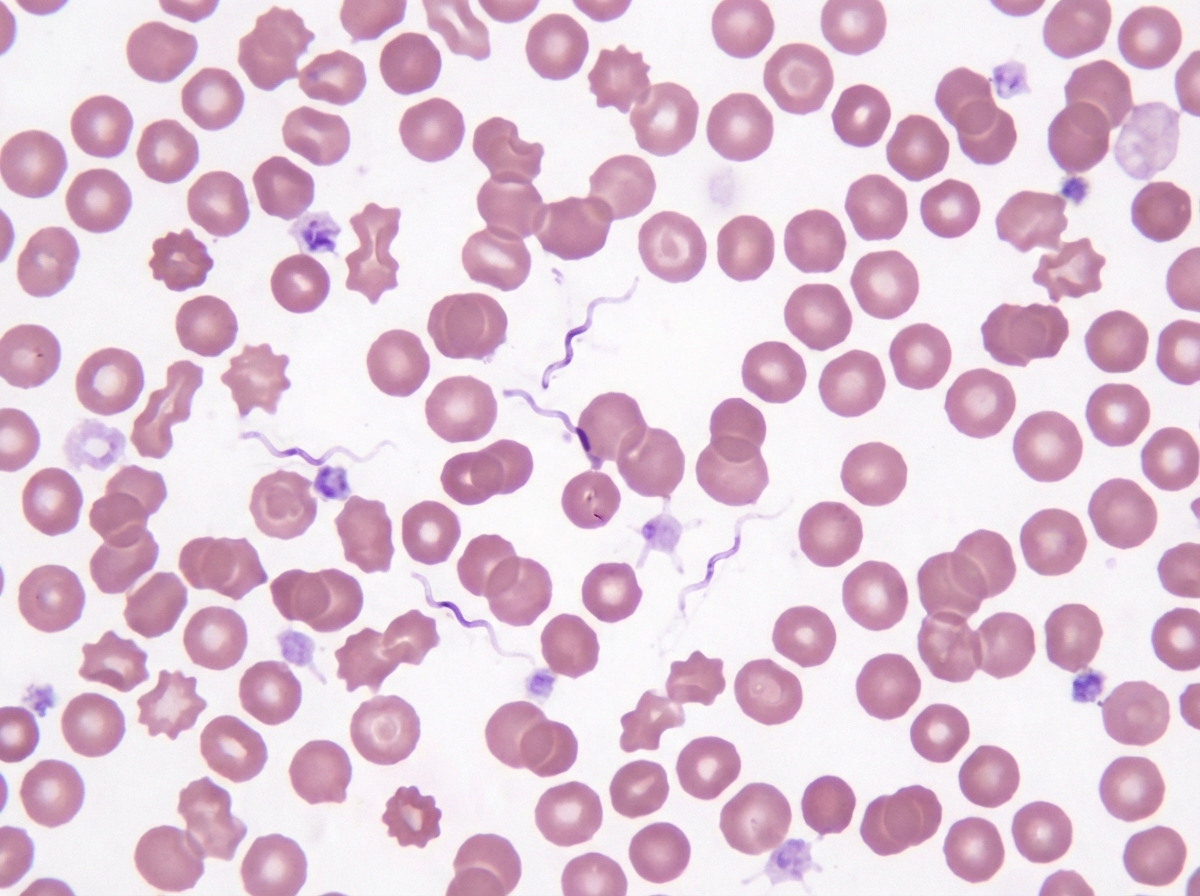
Peripheral blood smear of a patient with relapse of a fever seven days after remittance is shown. What is a true statement about the etiological agent?
Practice by Chapter
Staphylococci
Practice Questions
Streptococci and Enterococci
Practice Questions
Neisseria and Moraxella
Practice Questions
Corynebacterium and Listeria
Practice Questions
Bacillus and Clostridium
Practice Questions
Enterobacteriaceae
Practice Questions
Vibrio, Aeromonas, and Plesiomonas
Practice Questions
Pseudomonas and Related Bacteria
Practice Questions
Haemophilus and HACEK Group
Practice Questions
Bordetella and Brucella
Practice Questions
Mycobacteria
Practice Questions
Spirochetes
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
