Bacteriology — MCQs

On this page
A urinary bacterial count of less than 10^5/mL is considered insignificant in which of the following scenarios?
Which of the following is a selective medium for Pseudomonas?
A 14-year-old girl with cystic fibrosis is admitted to the hospital with fever and shortness of breath, diagnosed with pneumonia. During a respiratory therapy session, she coughs up mucus that is distinctly greenish in color. Which of the following organisms should be suspected?
A 34-year-old person presents with rapidly developing cough, dyspnea, expectoration, and blood-tinged sputum. The patient is febrile, cyanosed, and appears toxic. Chest examination reveals crepitations and rhonchi. What is the most likely diagnosis?
Tetanus is caused by which type of microorganism?
Absence of Vi-antibody in a typhoid patient indicates what regarding prognosis?
Which rickettsiae are able to grow in cell-free media?
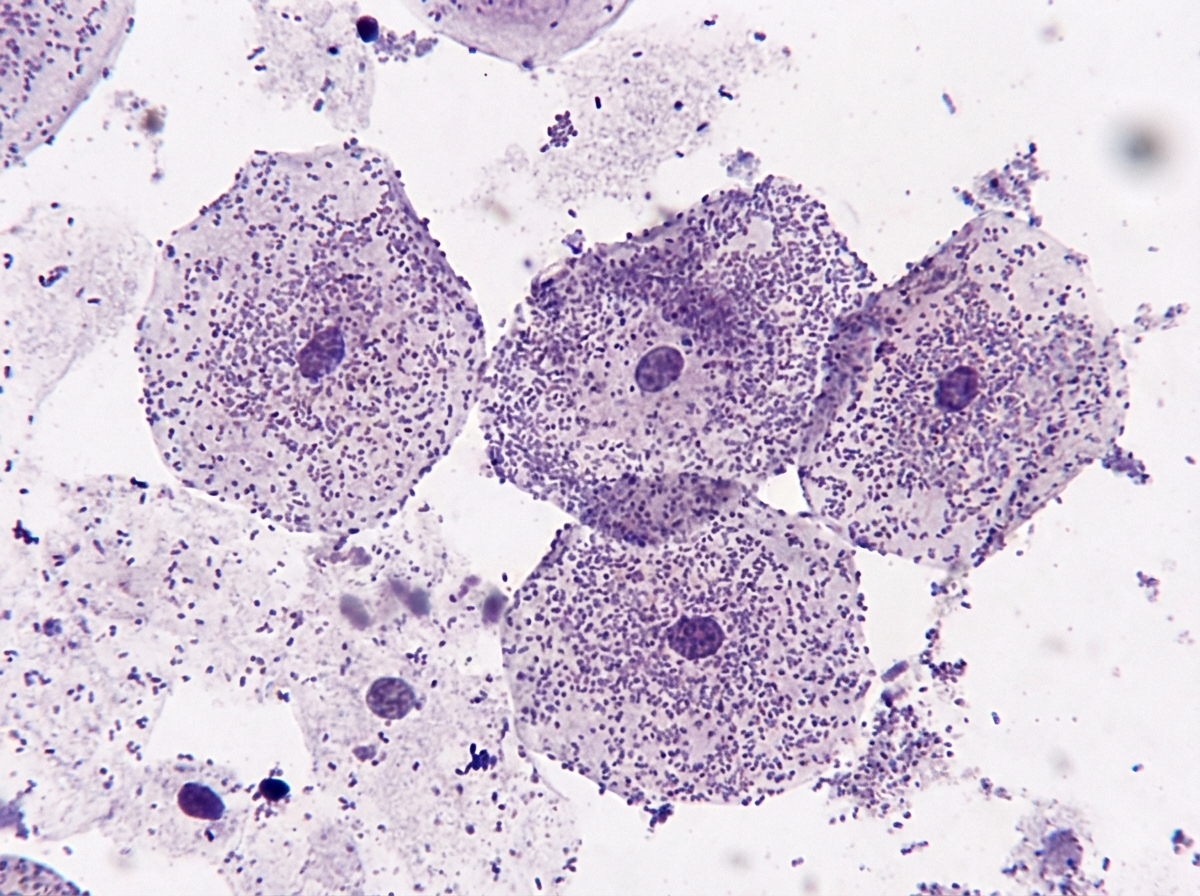
A 40-year-old woman presented with complaints of profuse vaginal discharge. There was no discharge from the cervix on speculum examination. The microscopy image of the vaginal discharge is shown above. Which of the following is NOT a diagnostic criterion for bacterial vaginosis?
Subterminal spores are found in which of the following organisms?
Spasm of masseter muscles occur in which condition?
Practice by Chapter
Staphylococci
Practice Questions
Streptococci and Enterococci
Practice Questions
Neisseria and Moraxella
Practice Questions
Corynebacterium and Listeria
Practice Questions
Bacillus and Clostridium
Practice Questions
Enterobacteriaceae
Practice Questions
Vibrio, Aeromonas, and Plesiomonas
Practice Questions
Pseudomonas and Related Bacteria
Practice Questions
Haemophilus and HACEK Group
Practice Questions
Bordetella and Brucella
Practice Questions
Mycobacteria
Practice Questions
Spirochetes
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
