Bacteriology — MCQs

On this page
Treponema is most difficult to isolate from which type of lesion?
Which mycobacteria grow in culture within 1-2 weeks?
A seven-year-old boy presented with high-grade fever, headache, disorientation, and projectile vomiting. Examination revealed neck rigidity and a positive Kernig's sign. Lumbar puncture was performed. Gram staining of the cerebrospinal fluid (CSF) showed Gram-negative cocci. What is the most likely cause of this infection?
Which of the following is a Category A Bioterrorism agent?
Which organisms are involved in pit and fissure caries?
A 40-year-old man presents with a nonproductive cough, malaise, sinusitis, and sore throat. His chest x-ray reveals patchy infiltrates in the upper right lung without consolidation. He denies recent exposure to new pets. Sputum Gram-stain shows poorly staining Gram-negative rods. Laboratory cultures on standard media are unsuccessful, but the organism grows in tissue culture. What bacterium is most likely causing this infection?
The Donath-Landsteiner reaction is used in the diagnosis of:
How can a carrier of Neisseria meningitidis be detected?
Which of the following is NOT a characteristic feature of Hutchinson's triad?
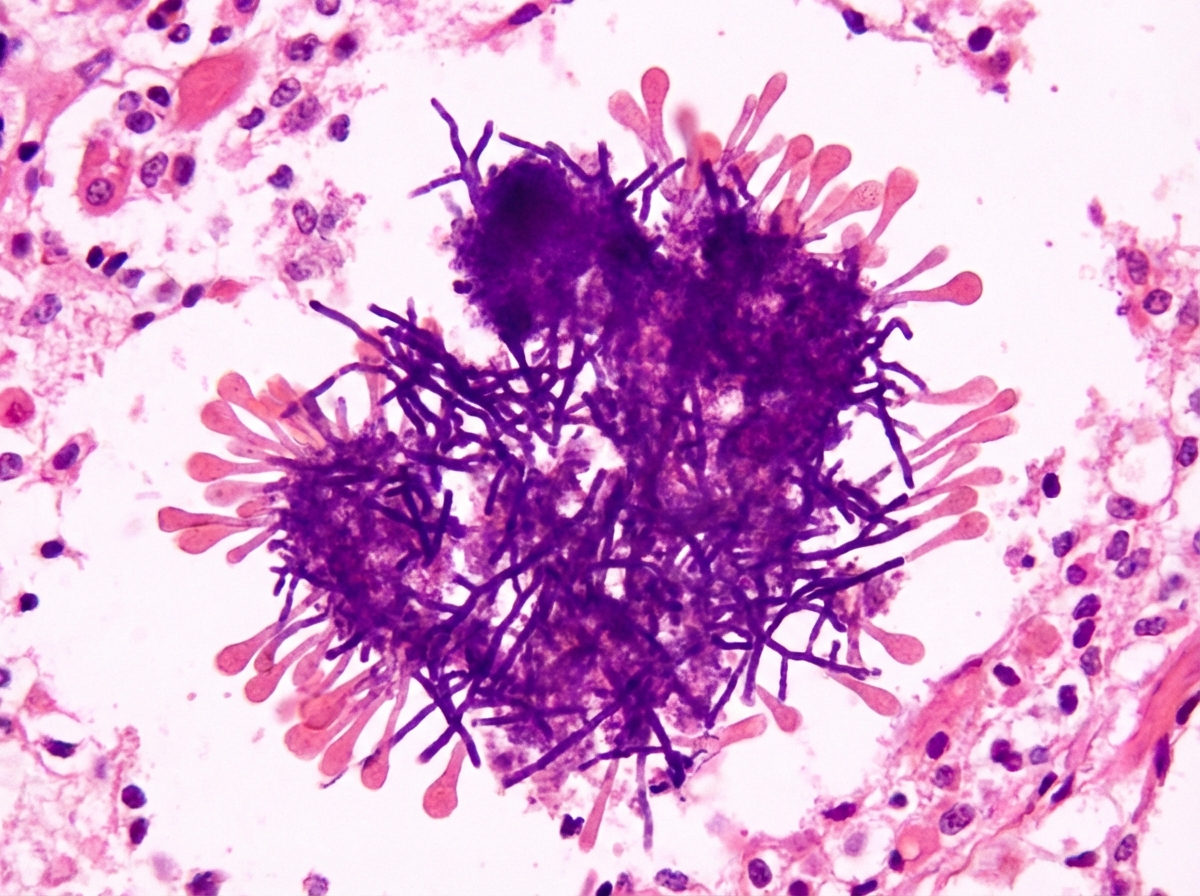
A 50-year-old female patient presented with a painless, exudative swelling of the right jaw, following trauma to the same area. Pus sent for culture revealed a sulfur granule on macroscopic examination. A Gram stain of the exudate is provided. What is the drug of choice for this condition?
Practice by Chapter
Staphylococci
Practice Questions
Streptococci and Enterococci
Practice Questions
Neisseria and Moraxella
Practice Questions
Corynebacterium and Listeria
Practice Questions
Bacillus and Clostridium
Practice Questions
Enterobacteriaceae
Practice Questions
Vibrio, Aeromonas, and Plesiomonas
Practice Questions
Pseudomonas and Related Bacteria
Practice Questions
Haemophilus and HACEK Group
Practice Questions
Bordetella and Brucella
Practice Questions
Mycobacteria
Practice Questions
Spirochetes
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
