Bacteriology — MCQs

On this page
The characteristic 'fried egg' colony morphology is observed in the culture of which microorganism?
What type of diarrhea is caused by Vibrio cholerae?
Which of the following statements is true about tuberculosis?
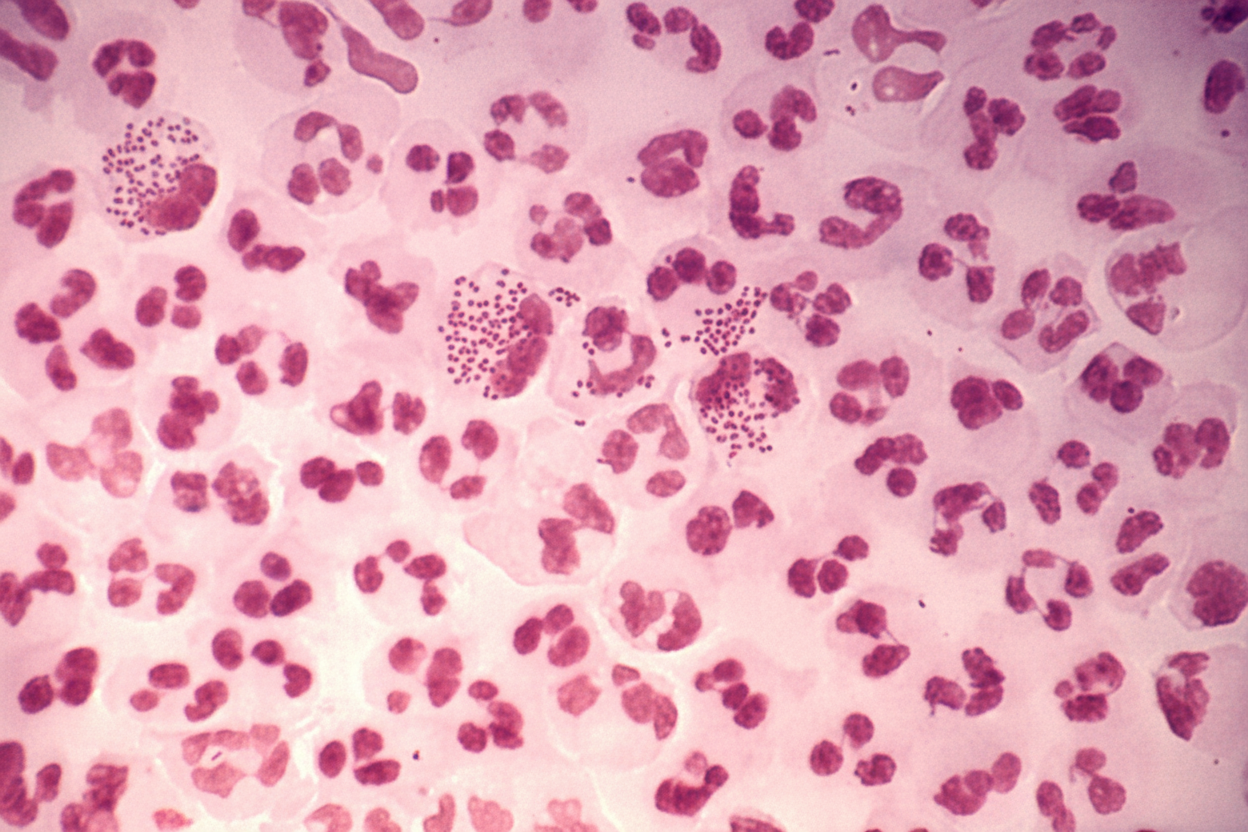
A 25-year-old sexually active unmarried male presents with urethral discharge after unprotected sex with a sexual worker. A Gram stain was provided; what is the most likely causative organism?
Which of the following is a scotochromogen?
Which of the following statements about Corynebacterium diphtheriae is incorrect?
For a bacterium to be seriously considered in the etiology of dental caries, it must:
Which structure is responsible for the adhesion of bacteria to surfaces?
Which of the following organisms is anaerobic?
Which of the following conditions is associated with antibodies against phenolic glycolipid (PGL-1)?
Practice by Chapter
Staphylococci
Practice Questions
Streptococci and Enterococci
Practice Questions
Neisseria and Moraxella
Practice Questions
Corynebacterium and Listeria
Practice Questions
Bacillus and Clostridium
Practice Questions
Enterobacteriaceae
Practice Questions
Vibrio, Aeromonas, and Plesiomonas
Practice Questions
Pseudomonas and Related Bacteria
Practice Questions
Haemophilus and HACEK Group
Practice Questions
Bordetella and Brucella
Practice Questions
Mycobacteria
Practice Questions
Spirochetes
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
