Bacteriology — MCQs

On this page
Which of the following microorganisms can be grown in cell culture media?
What is the commonest method for detecting diphtheria carriers?
A man presented with diarrhea three days after consuming uncooked meat. Stool examination revealed comma-shaped organisms with red blood cells and white blood cells. What is the causative organism?
Swimming pool conjunctivitis is caused by which of the following microorganisms?
What is the approximate number of genes in the complete genome sequence of M. tuberculosis?
"Genital elephantiasis" is caused by which of the following?
Chlamydia are isolated by which of the following methods?
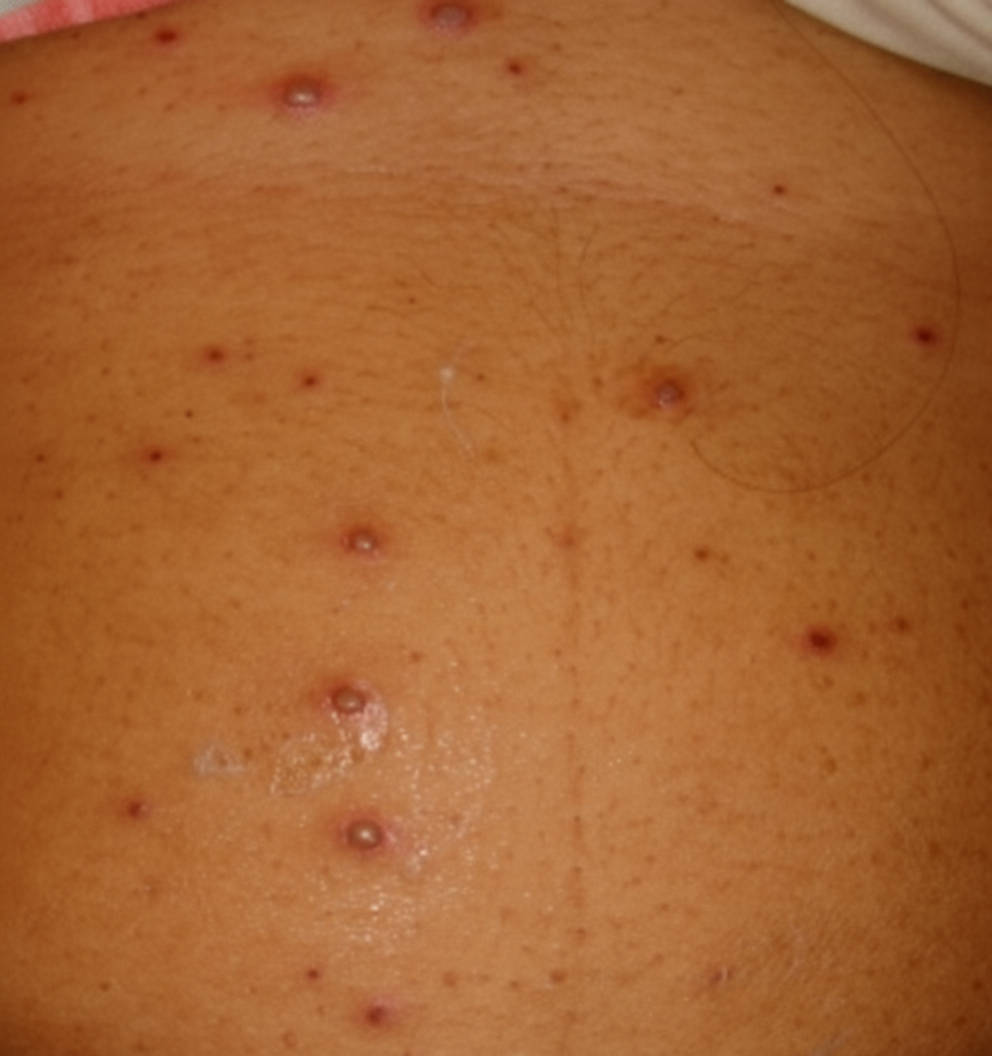
Which is the most common complication of this rash?
Which of the following is coagulase-negative Staphylococcus?
Which of the following media does not support the growth of H. influenzae?
Practice by Chapter
Staphylococci
Practice Questions
Streptococci and Enterococci
Practice Questions
Neisseria and Moraxella
Practice Questions
Corynebacterium and Listeria
Practice Questions
Bacillus and Clostridium
Practice Questions
Enterobacteriaceae
Practice Questions
Vibrio, Aeromonas, and Plesiomonas
Practice Questions
Pseudomonas and Related Bacteria
Practice Questions
Haemophilus and HACEK Group
Practice Questions
Bordetella and Brucella
Practice Questions
Mycobacteria
Practice Questions
Spirochetes
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
