Genetics and Disease — MCQs

On this page
The following pedigree represents which of the following genetic disorders?
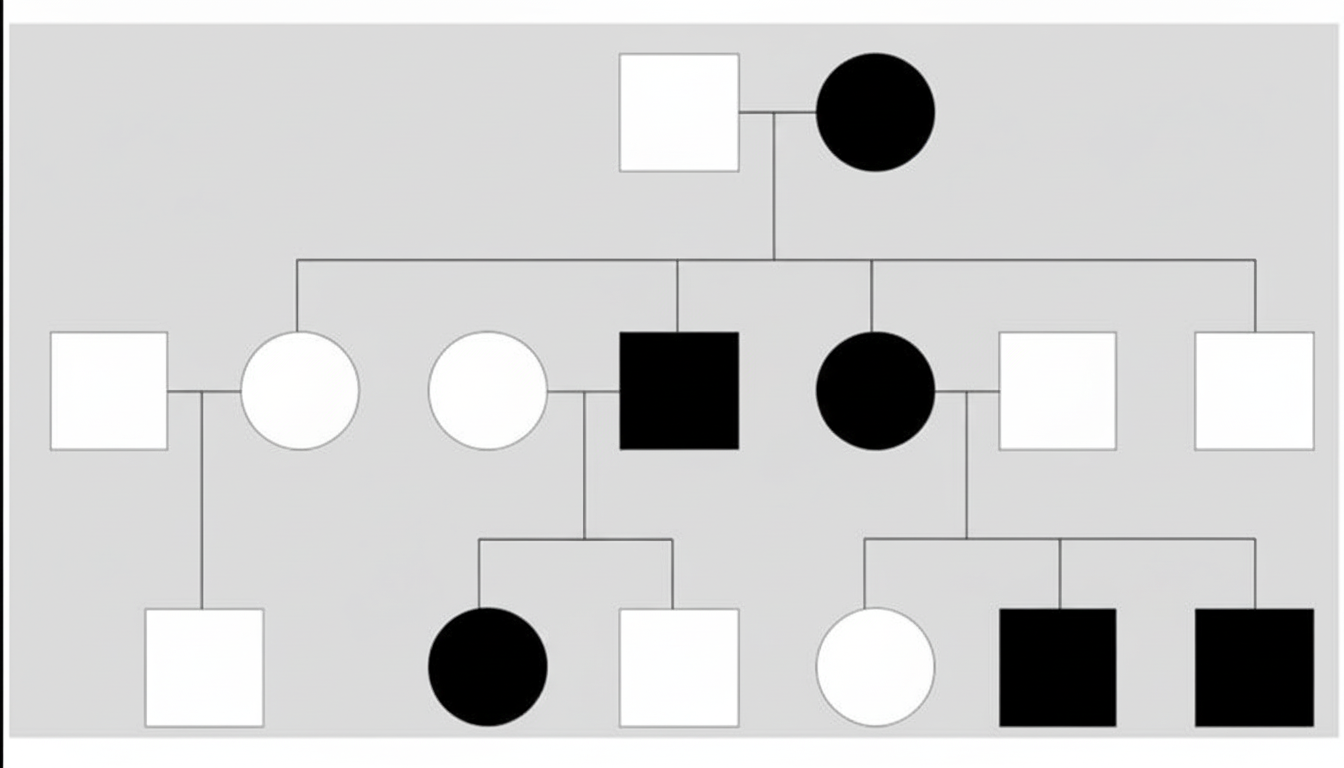
Which of the following statements is TRUE regarding Duchenne muscular dystrophy?
Which of the following statements about hemochromatosis is false?
Males who are sexually underdeveloped with rudimentary testes and prostate glands, sparse pubic and facial hair, long arms and legs and large hands and feet are likely to have which chromosome complement?
A family consists of a husband, wife, and children. The wife's father has Huntington's chorea. Which statement is true regarding this genetic condition?
What is the incidence of Down's syndrome directly proportional to?
Turner's syndrome is characterized by which of the following findings, except?
What is the cause of thick pancreatic secretions in cystic fibrosis?
What is the most common mutated gene in primary hemochromatosis?
Down's syndrome is characterized by which chromosomal abnormality?
Practice by Chapter
Principles of Medical Genetics
Practice Questions
Genetic Testing and Counseling
Practice Questions
Single Gene Disorders
Practice Questions
Chromosomal Disorders
Practice Questions
Mitochondrial Diseases
Practice Questions
Pharmacogenomics
Practice Questions
Cancer Genetics
Practice Questions
Genetics of Common Diseases
Practice Questions
Epigenetics and Disease
Practice Questions
Genetic Basis of Developmental Disorders
Practice Questions
Ethical Issues in Medical Genetics
Practice Questions
Gene Therapy and Precision Medicine
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
