Genetics and Disease — MCQs

On this page
Which of the following disorders is NOT autosomal dominant?
Which of the following is NOT a feature of Wilson's disease?
Which of the following is an autosomal dominant metabolic disorder?
The gene for Wilson's disease is located on which chromosome?
A normal couple has one daughter affected with Cystic fibrosis. They are now planning to have another child. What is the chance of siblings being affected by the disease?
Which of the following is an example of non-Mendelian inheritance?
Which of the following inherited disorders is the most common?
Edwards syndrome is associated with which chromosomal abnormality?
In addition to neurofibromatosis, what other examination finding would you expect for this patient?
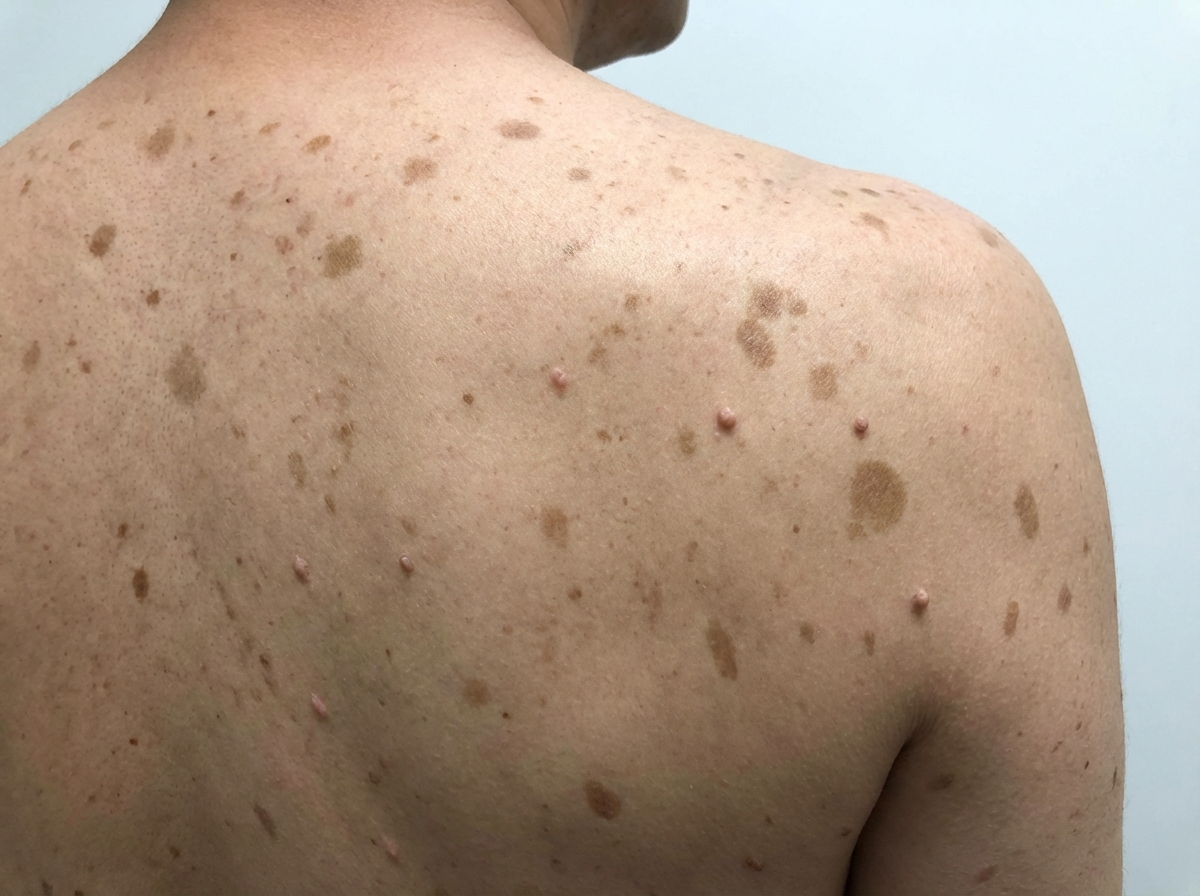
Absent radius is seen in all conditions except which of the following?
Practice by Chapter
Principles of Medical Genetics
Practice Questions
Genetic Testing and Counseling
Practice Questions
Single Gene Disorders
Practice Questions
Chromosomal Disorders
Practice Questions
Mitochondrial Diseases
Practice Questions
Pharmacogenomics
Practice Questions
Cancer Genetics
Practice Questions
Genetics of Common Diseases
Practice Questions
Epigenetics and Disease
Practice Questions
Genetic Basis of Developmental Disorders
Practice Questions
Ethical Issues in Medical Genetics
Practice Questions
Gene Therapy and Precision Medicine
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
