Cardiology — MCQs

On this page
Diagnose the cardiac disorder based on the provided ECG findings.
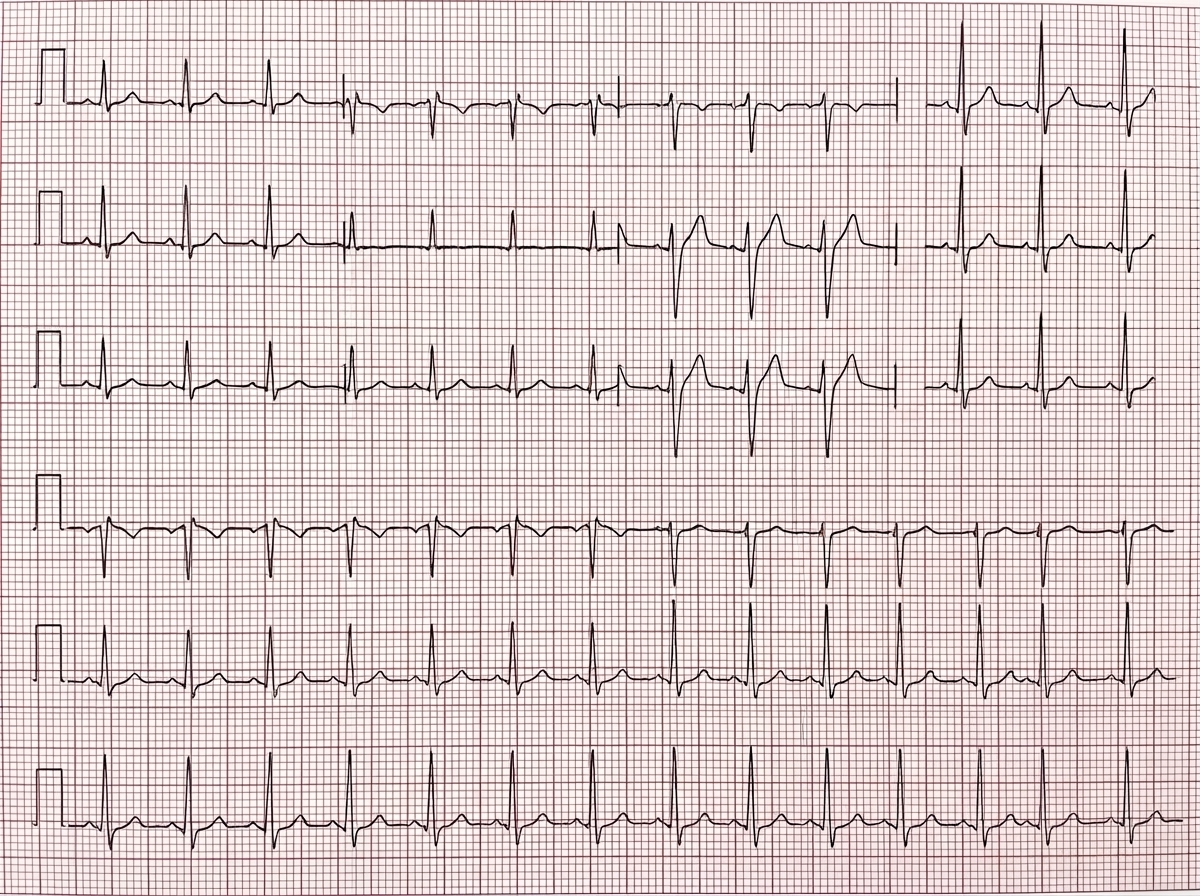
What is the typical area of the mitral valve in severe mitral stenosis during pregnancy?
A 60-year-old male, diabetic and smoker, presents with 3 hours of substernal chest pain. Which of the following statements is true regarding his ECG findings?
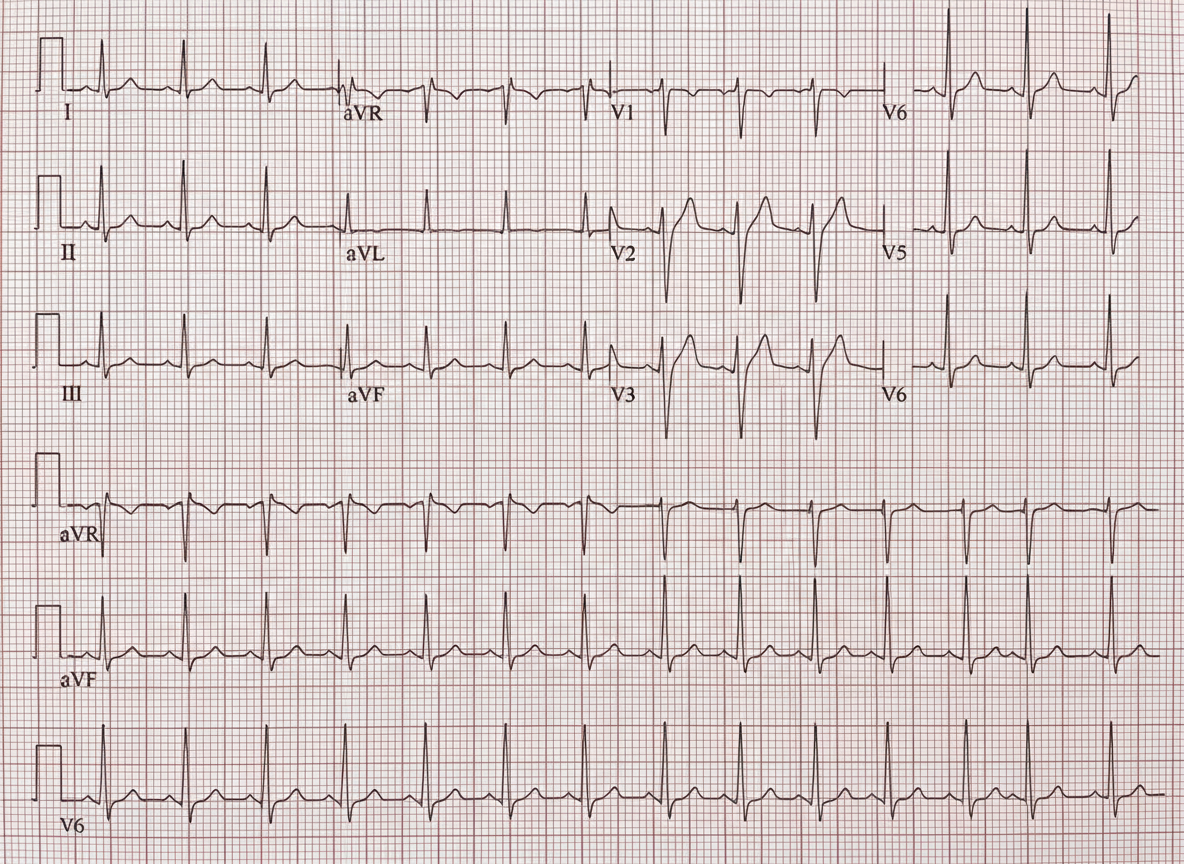
A 44-year-old woman presents with a 4-year history of increasing dyspnea and fatigue. Physical examination reveals increased JVP and a reduced carotid pulse. Precordial examination reveals a left parasternal lift, loud P2, and right-sided S3 and S4. There are no audible murmurs. Chest X-ray reveals clear lung fields and an ECG shows evidence of right ventricular hypertrophy. Pulmonary function tests show a slight restrictive pattern. A diagnosis of primary pulmonary hypertension (PPH) is made. Which of the following is the most likely cause of death in this condition?
Which of the following is NOT a component of the classical triad of ECG changes in pericardial effusion with cardiac tamponade?
Which of the following is NOT true regarding beta-blocker therapy in patients with congestive heart failure?
Which of the following is NOT a high-risk lesion for Infective Endocarditis?
A patient presents with sharp, shooting retrosternal pain that progresses downward, initially felt between the scapulae and later migrating to the epigastric region. On examination, the patient has feeble lower limb pulses compared to the upper limbs. This clinical presentation is highly suggestive of which of the following conditions?
Which of the following is true regarding atrial fibrillation?
Duke's criteria is used for the evaluation of what condition?
Practice by Chapter
Coronary Artery Disease and Angina
Practice Questions
Acute Coronary Syndromes
Practice Questions
Heart Failure
Practice Questions
Cardiac Arrhythmias
Practice Questions
Valvular Heart Diseases
Practice Questions
Cardiomyopathies
Practice Questions
Pericardial Diseases
Practice Questions
Congenital Heart Disease in Adults
Practice Questions
Hypertension and Hypertensive Emergencies
Practice Questions
Pulmonary Hypertension
Practice Questions
Non-invasive Cardiac Diagnostics
Practice Questions
Preventive Cardiology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
