Cardiology — MCQs

On this page
Auenbrugger's sign is seen in which of the following conditions?
Notching of the ribs is seen in which of the following conditions?
Right axis deviation is seen in all except?
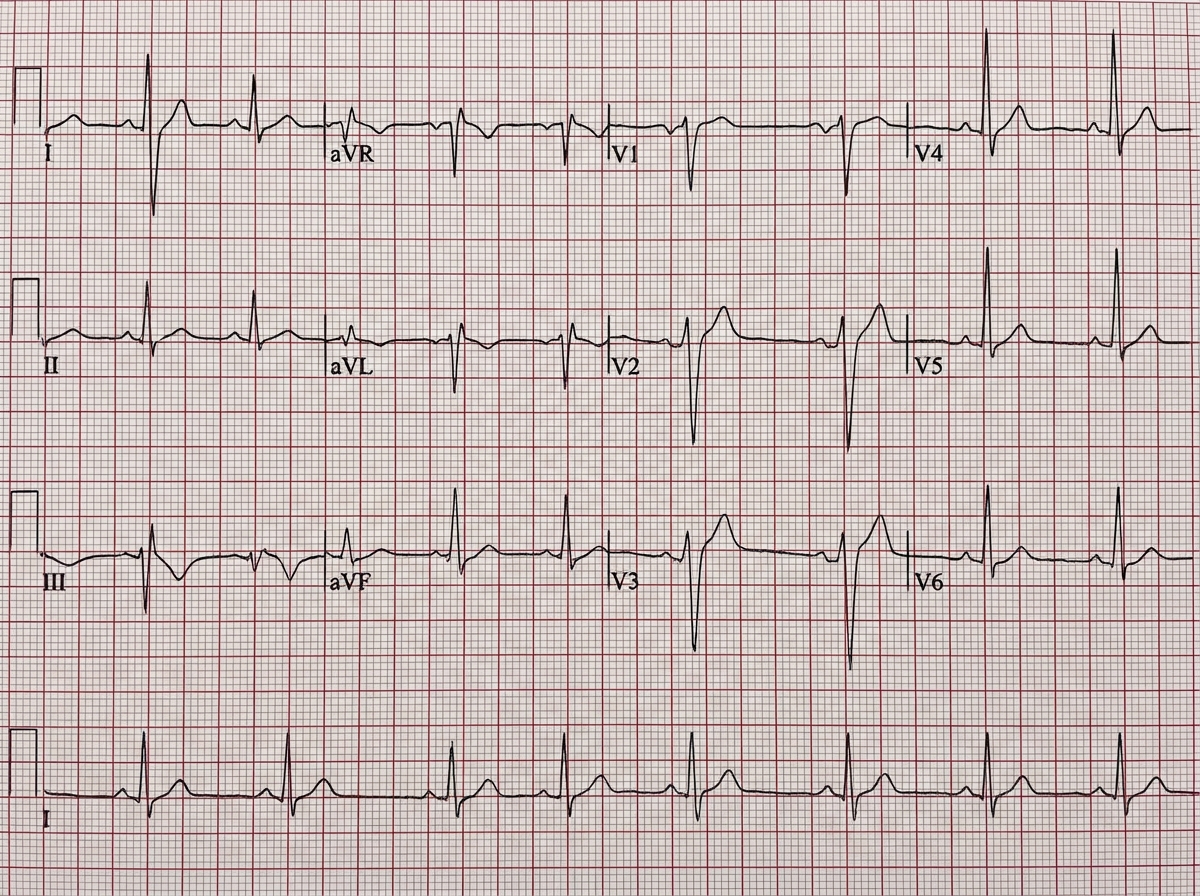
The given ECG shows which of the following conditions?
Which of the following parameters adds predictive information regarding cardiovascular risk stratification and the measurement of serum cholesterol?
A patient complains of retrosternal chest pain lasting for more than half an hour. What is the most likely diagnosis?
Which of the following is NOT considered a major criterion in the Framingham criteria for the diagnosis of congestive heart failure?
The ROSE questionnaire is used for what purpose?
A 50-year-old patient with a history of breast cancer presents with breathlessness. What would the ECG most likely show?
Broad complex tachycardia is suggested by which of the following?
Practice by Chapter
Coronary Artery Disease and Angina
Practice Questions
Acute Coronary Syndromes
Practice Questions
Heart Failure
Practice Questions
Cardiac Arrhythmias
Practice Questions
Valvular Heart Diseases
Practice Questions
Cardiomyopathies
Practice Questions
Pericardial Diseases
Practice Questions
Congenital Heart Disease in Adults
Practice Questions
Hypertension and Hypertensive Emergencies
Practice Questions
Pulmonary Hypertension
Practice Questions
Non-invasive Cardiac Diagnostics
Practice Questions
Preventive Cardiology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
