Phoniatrics and Voice Disorders — MCQs

On this page
A patient complains of pain that seems similar to trigeminal neuralgia. Examination reveals a nasopharyngeal tumor as the reason for the pain. What is the most likely diagnosis?
Blomsingher prosthesis is used for the production of?
A 10-year-old boy developed hoarseness of voice following an attack of diphtheria. No other significant cranial nerves or vocal cords are paralyzed. What is the treatment of choice?
A 35-year-old male singer presents with complaints of hoarseness, vocal fatigue, and pain in the neck on prolonged phonation. Direct laryngoscopy shows bilateral pinhead-sized swellings on the anterior one-third and posterior two-thirds junction of the vocal cords. What is the probable diagnosis?
A patient who is a teacher by profession presents to the clinic with hoarseness of voice. What is the most likely diagnosis for this patient?
Which of the following studies is shown below?
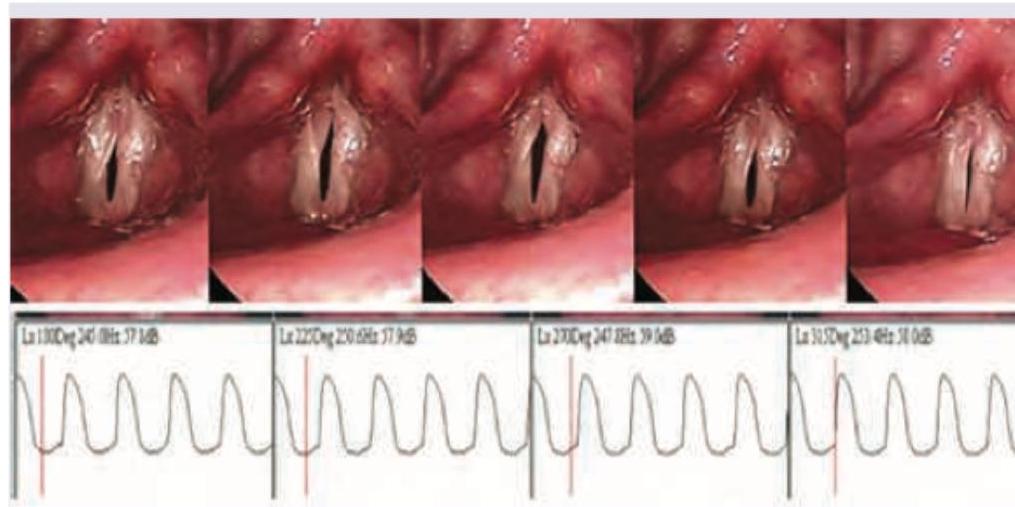
A 20-year-old lady singer of a rock band develops diplophonia after a performance. The laryngoscopy image is shown below. What is the most likely diagnosis?
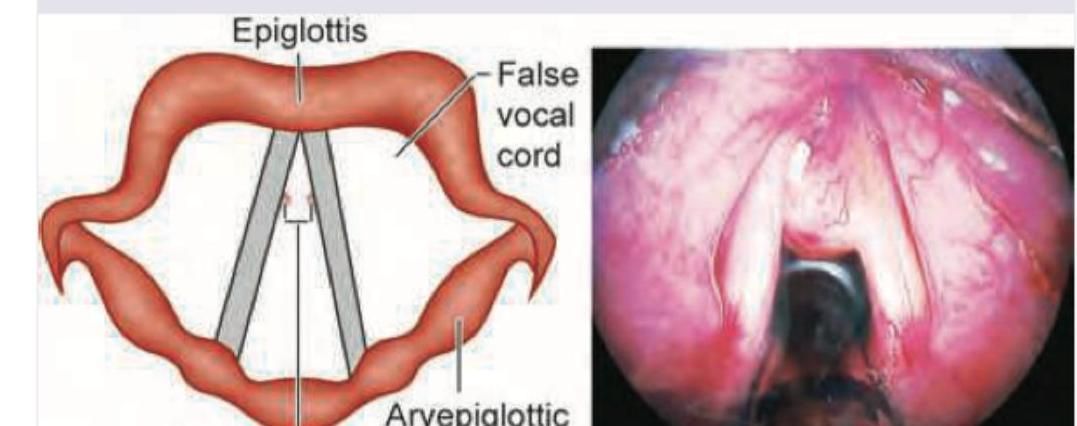
A singer presents with difficulty singing at a high pitch. On examination, bowing of the vocal cord is observed on the right side. Which of the following muscles has likely been compromised?
Dysphonia plica ventricularis is produced from:
The primary goal of Type 1 thyroplasty is:
Practice by Chapter
Vocal Fold Structure and Function
Practice Questions
Voice Assessment and Examination
Practice Questions
Stroboscopy and High-speed Imaging
Practice Questions
Nodules, Polyps, and Cysts
Practice Questions
Vocal Fold Paralysis
Practice Questions
Spasmodic Dysphonia
Practice Questions
Professional Voice Care
Practice Questions
Voice Therapy
Practice Questions
Phonosurgery Techniques
Practice Questions
Laryngeal Framework Surgery
Practice Questions
Gender-Affirming Voice Care
Practice Questions
Pediatric Voice Disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
