Diseases of the Pharynx — MCQs

On this page
A 35-year-old man presents to the emergency department with a complaint of food stuck in his throat. On examination, a bone is seen in the left piriform recess. Which of the following is most likely to be impaired?
All are correct about the image shown below except:
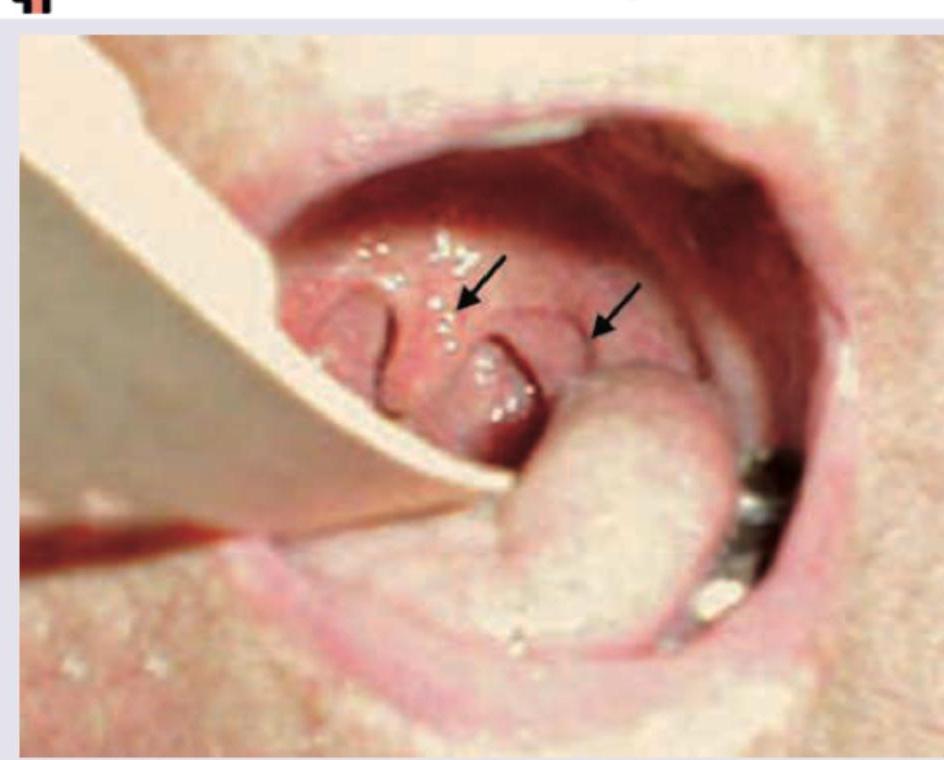
All are correct about the condition except:
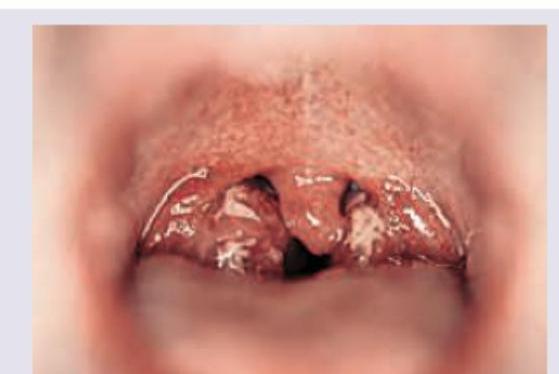
What is incorrect about the picture shown?
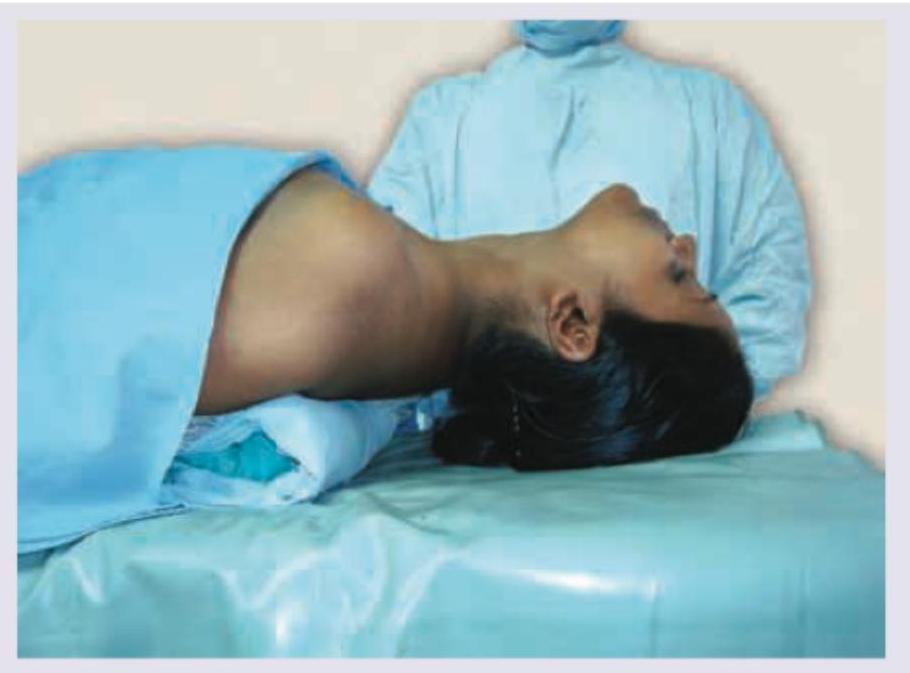
All are correct about the image shown except:
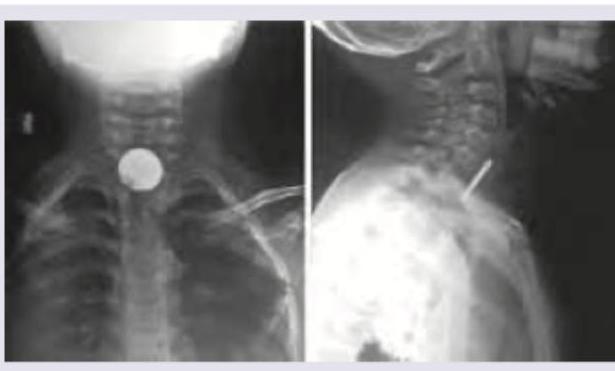
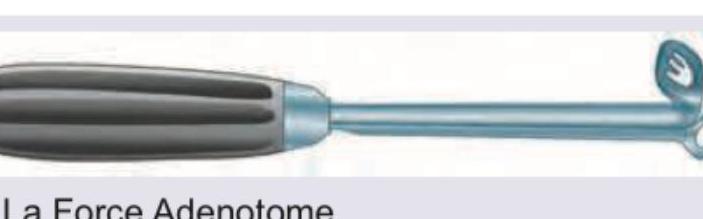
Name the instrument shown below:
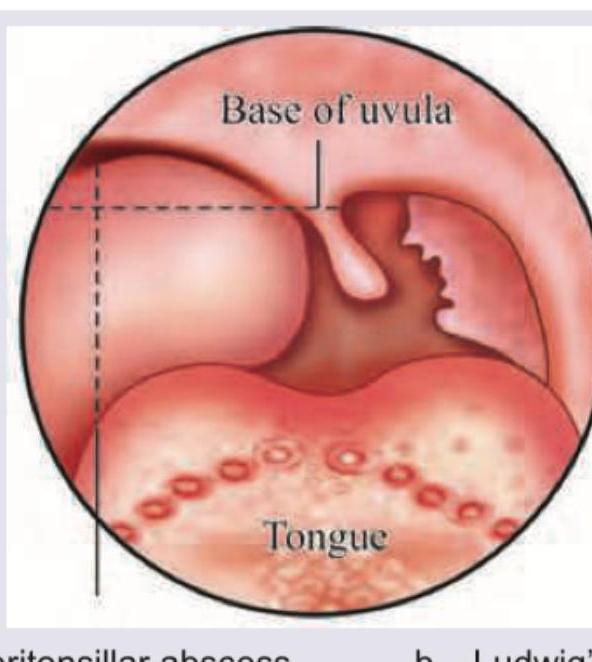
A 3-year-old child presents with fever, unilateral throat pain and trismus. Throat examination shows:
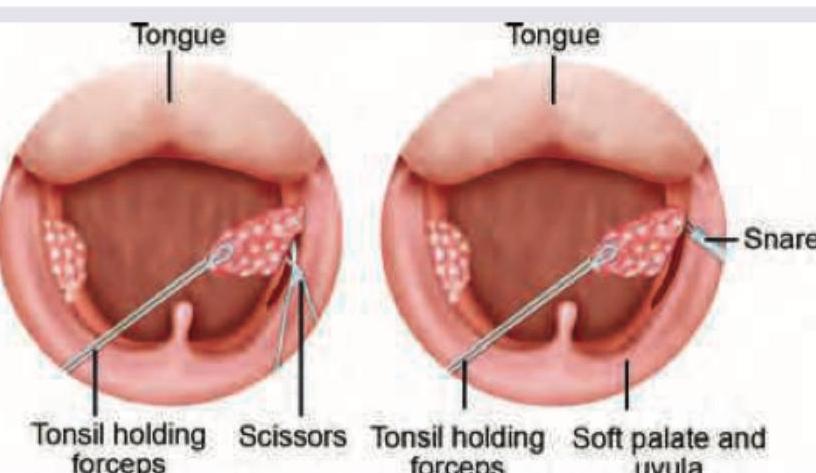
All are indications for the procedure shown except:
Regarding "Quinsy" all of the following are correct EXCEPT:
A patient presented with 2 days history of fever. On examination there was a swelling in the neck and one side tonsil was pushed to midline. What is the most likely diagnosis:-
Practice by Chapter
Pharyngitis
Practice Questions
Tonsillitis
Practice Questions
Peritonsillar Abscess
Practice Questions
Retropharyngeal Abscess
Practice Questions
Adenoid Hypertrophy
Practice Questions
Sleep-Disordered Breathing
Practice Questions
Obstructive Sleep Apnea
Practice Questions
Nasopharyngeal Carcinoma
Practice Questions
Oropharyngeal Carcinoma
Practice Questions
Hypopharyngeal Carcinoma
Practice Questions
Dysphagia
Practice Questions
Globus Pharyngeus
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
