Diseases of the Pharynx — MCQs

On this page
Which of the following statements regarding foreign bodies in the oropharynx is FALSE?
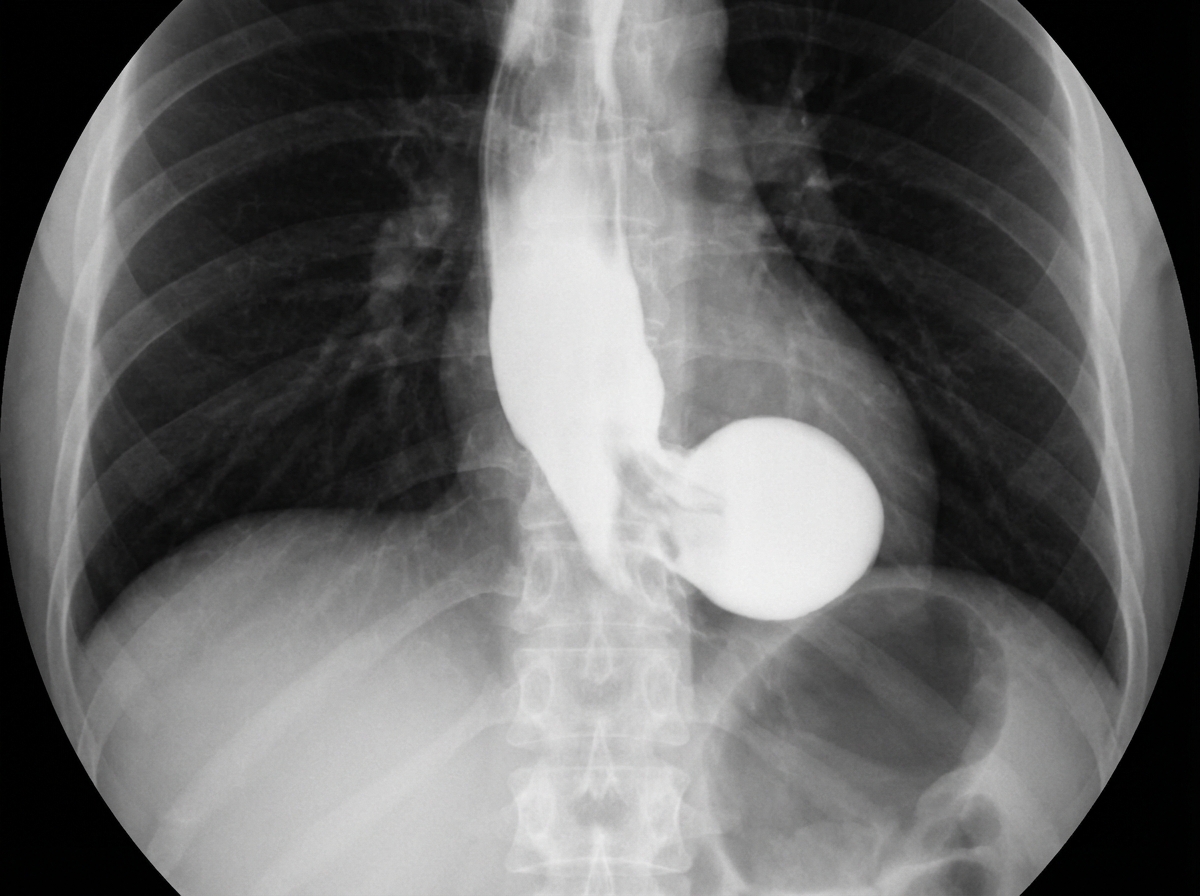
A 65-year-old patient presents with dysphagia and regurgitation. Barium swallow imaging is provided. What is the diagnosis?
Which anatomical region is NOT considered part of the hypopharynx?
Which of the following is NOT a contraindication to tonsillectomy?
Which of the following is NOT a contraindication for routine tonsillectomy?
Thornwaldt's abscess is seen in which condition?
What is the initial imaging of choice for angiofibroma?
According to the WHO classification, to which category does undifferentiated carcinoma of the nasopharynx belong?
What is the location of Killian dehiscence?
X-ray showing an air column between a soft tissue mass and the posterior wall of the nasopharynx is suggestive of which condition?
Practice by Chapter
Pharyngitis
Practice Questions
Tonsillitis
Practice Questions
Peritonsillar Abscess
Practice Questions
Retropharyngeal Abscess
Practice Questions
Adenoid Hypertrophy
Practice Questions
Sleep-Disordered Breathing
Practice Questions
Obstructive Sleep Apnea
Practice Questions
Nasopharyngeal Carcinoma
Practice Questions
Oropharyngeal Carcinoma
Practice Questions
Hypopharyngeal Carcinoma
Practice Questions
Dysphagia
Practice Questions
Globus Pharyngeus
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
