Fungal Skin Infections — MCQs

On this page
What is the causative agent of Favus?
A patient with asymptomatic annular skin lesion as shown presents to OPD. Which investigation should be done?
A carpenter presents with a nodule on dorsum of hand which ulcerates after few days and has not healed for last 2 months. Biopsy of lesion was performed and shown below. All are used in management of this condition except:
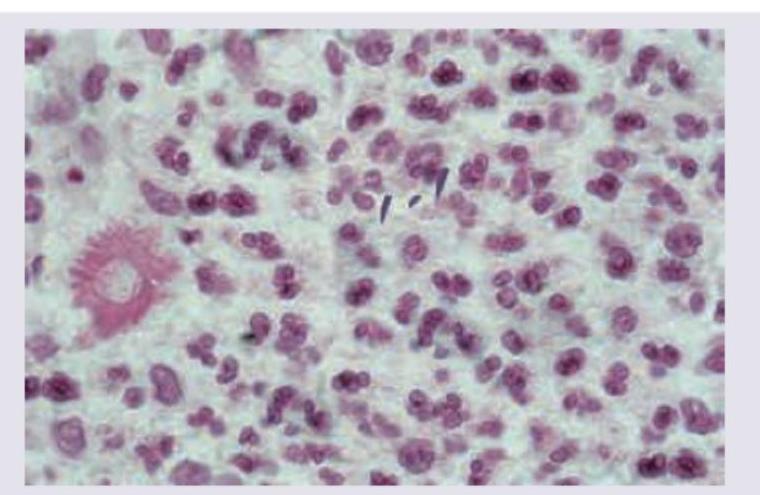
A carpenter presents with a nodule on dorsum of hand which ulcerates after few days and has not healed for last 2 months. Biopsy of lesion was performed and shown below. Diagnosis is:
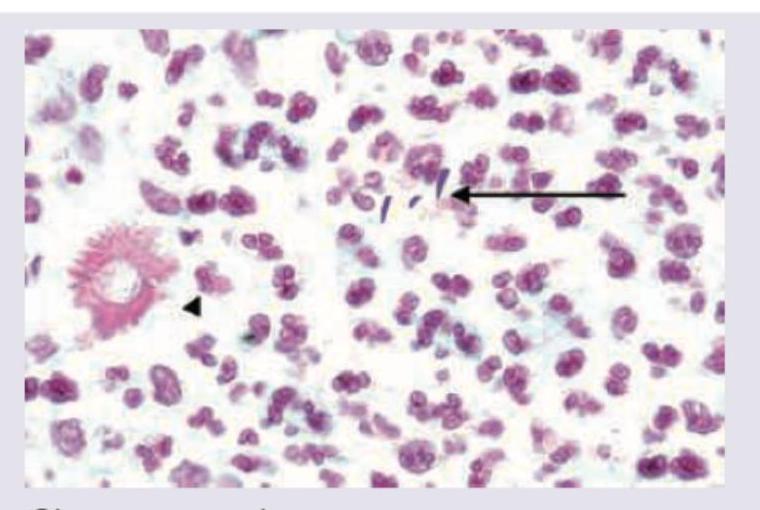
A female had a thorn prick 5 years ago. She presents with development of slowly growing $2 \times 2 \mathrm{~cm}$ verrucous lesion which on KOH mount shows the following image. Diagnosis is: (AIIMS Nov 2017)
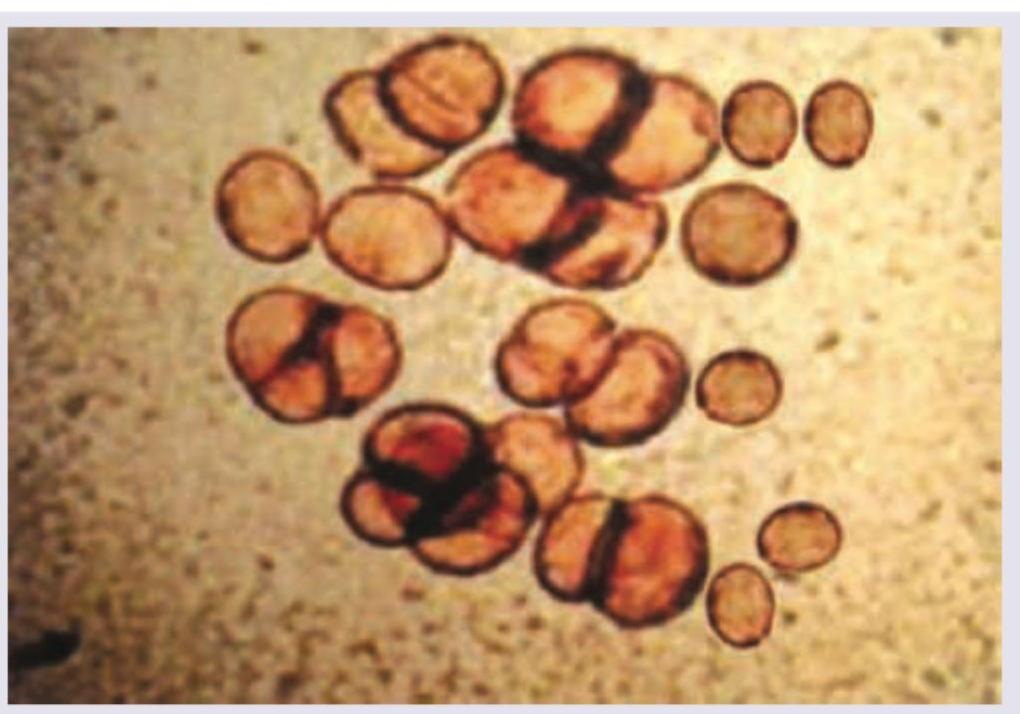
All of the following statements regarding the image given below are true except:
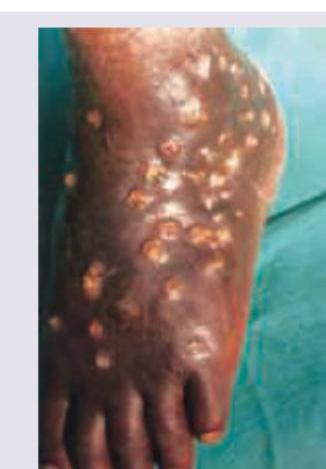
What is the most likely diagnosis of the image provided below?
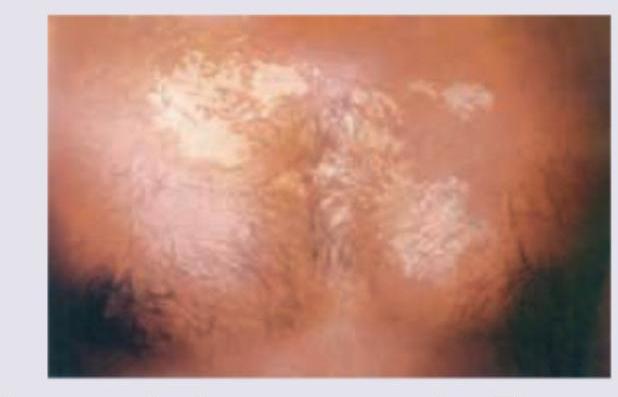
All of the following statements regarding this image are true except: (Recent NEET Pattern 2016-17)
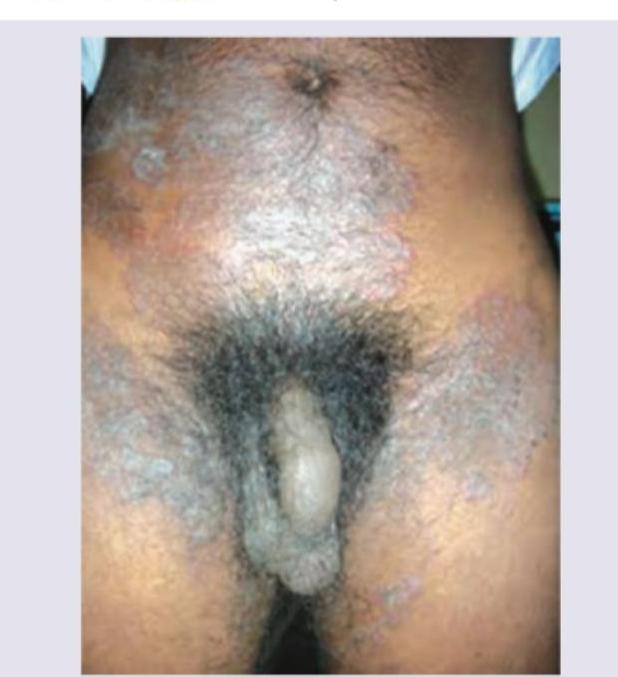
A 42-year-old male complains of itching, his clinical presentation is given in the image. Which of the following statement is false?
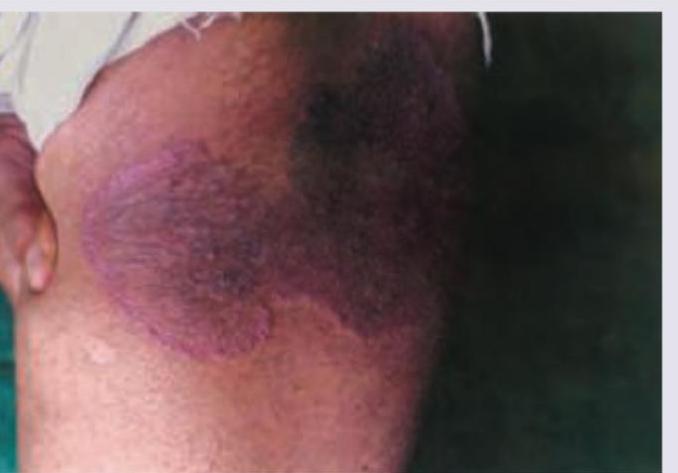
A 25-year-woman developed scaly, pruritic lesions on her back. She applied topical steroids on the lesion, following the advice of a quack. Subsequently her lesions worsened. What is the diagnosis?
Practice by Chapter
Dermatophytoses
Practice Questions
Tinea Versicolor
Practice Questions
Candidiasis
Practice Questions
Onychomycosis
Practice Questions
Subcutaneous Mycoses
Practice Questions
Systemic Mycoses with Cutaneous Manifestations
Practice Questions
Opportunistic Fungal Infections
Practice Questions
Mycetoma
Practice Questions
Tropical Fungal Infections
Practice Questions
Diagnosis of Fungal Infections
Practice Questions
Antifungal Therapy
Practice Questions
Preventive Strategies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
