General Anesthesia — MCQs

On this page
Which of the following is a depolarising muscle relaxant?
Which of the following has analgesic property?
The complete fluorination in Desflurane produces all the following effects except:
Which drug is responsible for Phase II block?
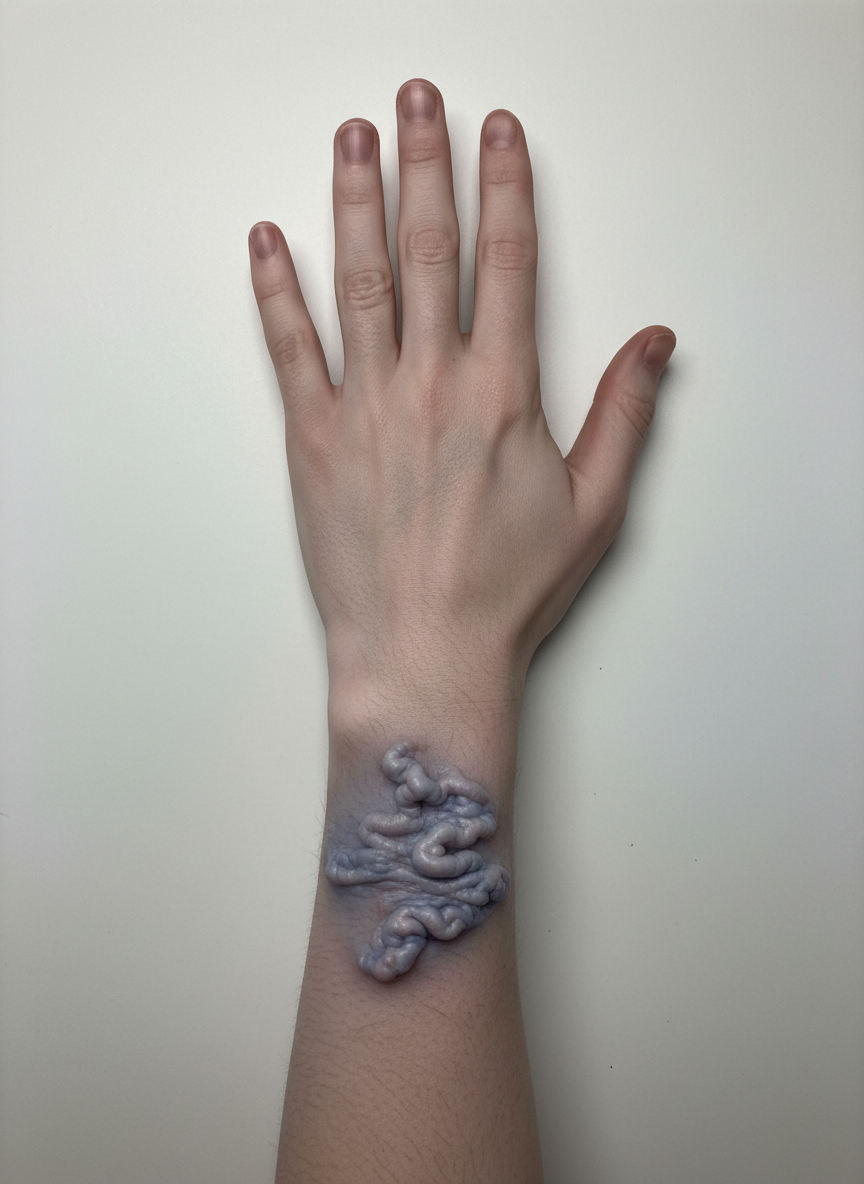
Which non-depolarizing muscle relaxant is contraindicated in the patient shown?
Atracurium is metabolized by which of the following mechanisms?
Which of the following muscles is affected first by a neuromuscular blocker?
Which anesthetic agent is explosive in the presence of cautery?
Which muscle relaxant is the drug of choice in a patient with renal failure?
Which of the following intravenous anesthetic agents is considered the most immunogenically safe?
Practice by Chapter
History of Anesthesia
Practice Questions
Preoperative Evaluation
Practice Questions
Pharmacology of Inhalational Anesthetics
Practice Questions
Pharmacology of Intravenous Anesthetics
Practice Questions
Neuromuscular Blocking Agents
Practice Questions
Airway Management
Practice Questions
Endotracheal Intubation
Practice Questions
Difficult Airway Algorithms
Practice Questions
Intraoperative Monitoring
Practice Questions
Depth of Anesthesia Monitoring
Practice Questions
Emergence from Anesthesia
Practice Questions
Postoperative Care
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
