General Anesthesia — MCQs

On this page
Postoperative muscle ache is commonly caused by which of the following agents?
Which of the following statements about Total Intra-Venous Anaesthesia (TIVA) is true?
What is the role of egg lecithin in propofol formulation?
Which of the following inhalation agents has a blood-gas partition coefficient similar to nitrous oxide?
A 35 y/o asthmatic patient is scheduled for a minor surgical procedure. Which induction agent and muscle relaxant combination is safest for this patient?
During regional anesthesia, which of the following local anesthetic agents has the longest duration of action when used for peripheral nerve block?
A 50-year-old male patient underwent lower abdominal surgery under general anaesthesia. Vecuronium was administered as a muscle relaxant during the procedure. At the end of the surgery, which of the following is the most appropriate agent to reverse the effects of vecuronium?
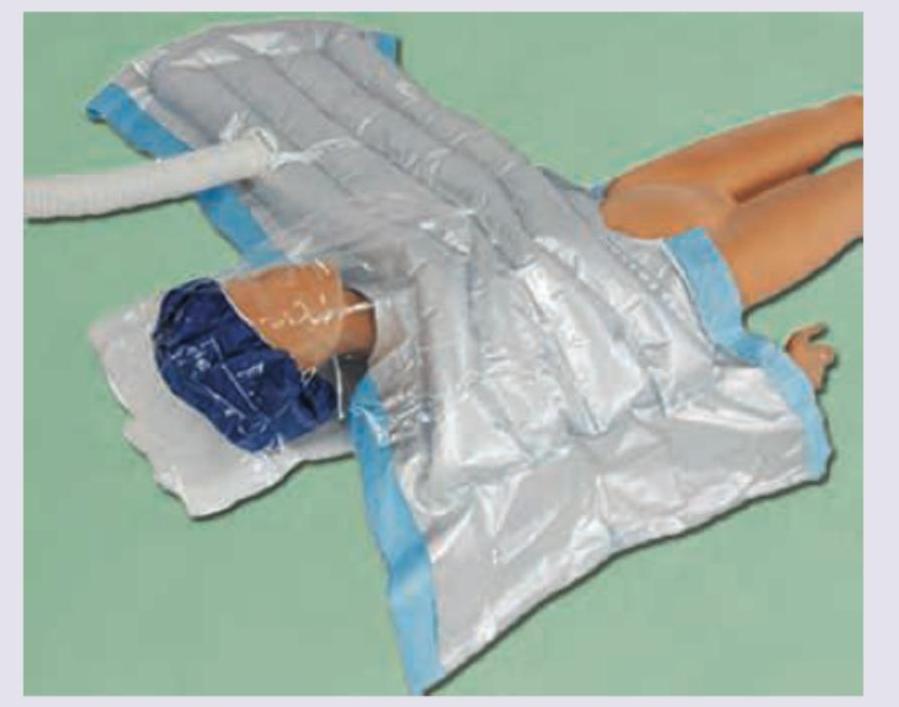
A 70-year-old patient with bilateral avascular necrosis of hip joint is undergoing total hip replacement in general anesthesia. The device shown below is used for?
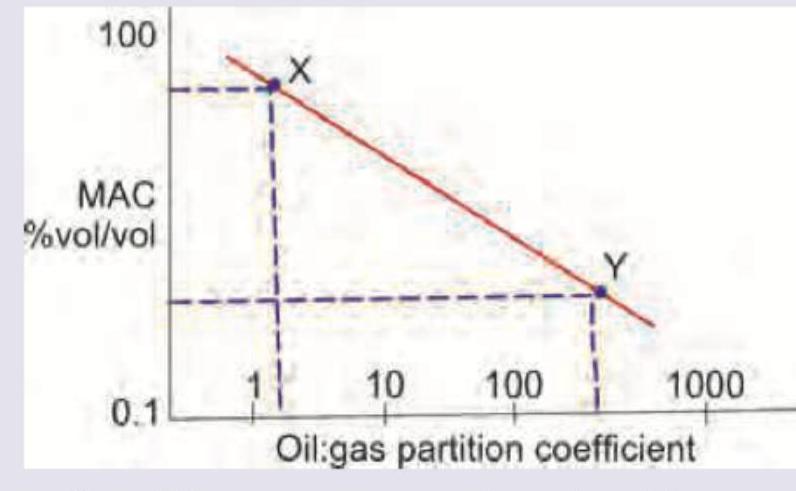
Which is correct about the anesthetic drugs X and Y respectively?
The commonly used muscle relaxant with quickest onset of action and spontaneous recovery is :
Practice by Chapter
History of Anesthesia
Practice Questions
Preoperative Evaluation
Practice Questions
Pharmacology of Inhalational Anesthetics
Practice Questions
Pharmacology of Intravenous Anesthetics
Practice Questions
Neuromuscular Blocking Agents
Practice Questions
Airway Management
Practice Questions
Endotracheal Intubation
Practice Questions
Difficult Airway Algorithms
Practice Questions
Intraoperative Monitoring
Practice Questions
Depth of Anesthesia Monitoring
Practice Questions
Emergence from Anesthesia
Practice Questions
Postoperative Care
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
