Neuroanatomy — MCQs

On this page
Which cranial and sacral nerves carry parasympathetic fibers?
What is a known side effect of vagal nerve stimulation?
Which of the following drugs exhibits the phenomenon described?
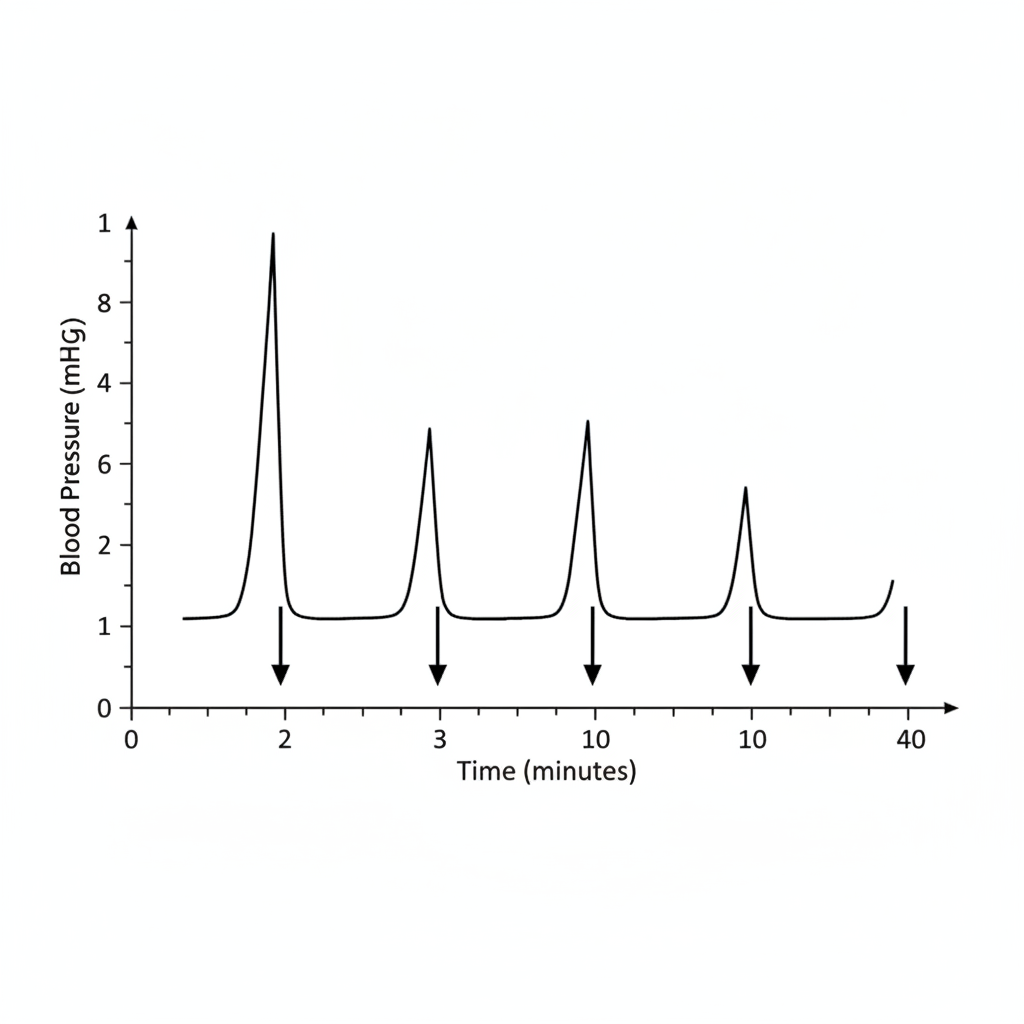
A patient cannot speak but can communicate by writing. Which of the following brain areas is most likely affected?
The facial colliculus is located in which part of the brainstem?
What is the most common salivary gland tumor in adults?
Identify the structure located at the position indicated by the arrow within the internal capsule.
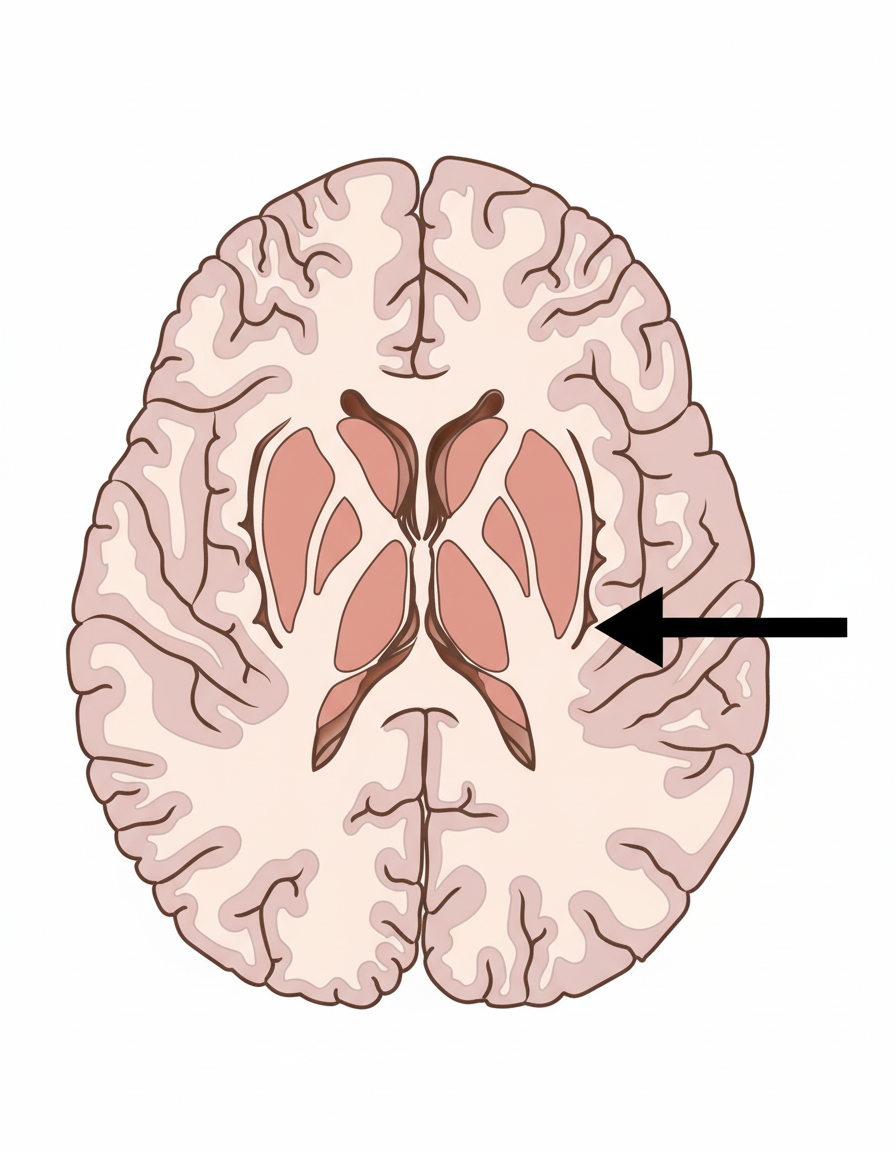
Gustatory hallucination is most commonly associated with which condition?
Hyperacute graft rejection in kidney transplants is primarily due to which of the following mechanisms?
Actin is made of:
Practice by Chapter
Organization of the Nervous System
Practice Questions
Spinal Cord Anatomy
Practice Questions
Brainstem Anatomy
Practice Questions
Cerebellum
Practice Questions
Diencephalon
Practice Questions
Cerebral Cortex
Practice Questions
Basal Ganglia
Practice Questions
Limbic System
Practice Questions
Cranial Nerves
Practice Questions
Autonomic Nervous System
Practice Questions
Neural Pathways and Tracts
Practice Questions
Neurovascular Anatomy
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
