Neuroanatomy — MCQs

On this page
The type of joint between the sacrum and the coccyx is a
In alcoholic liver disease, which of the following pigments is deposited in the hepatocytes?
All of the following form the deep venous system of the brain, EXCEPT?
All of the following have general visceral efferent fibers except?
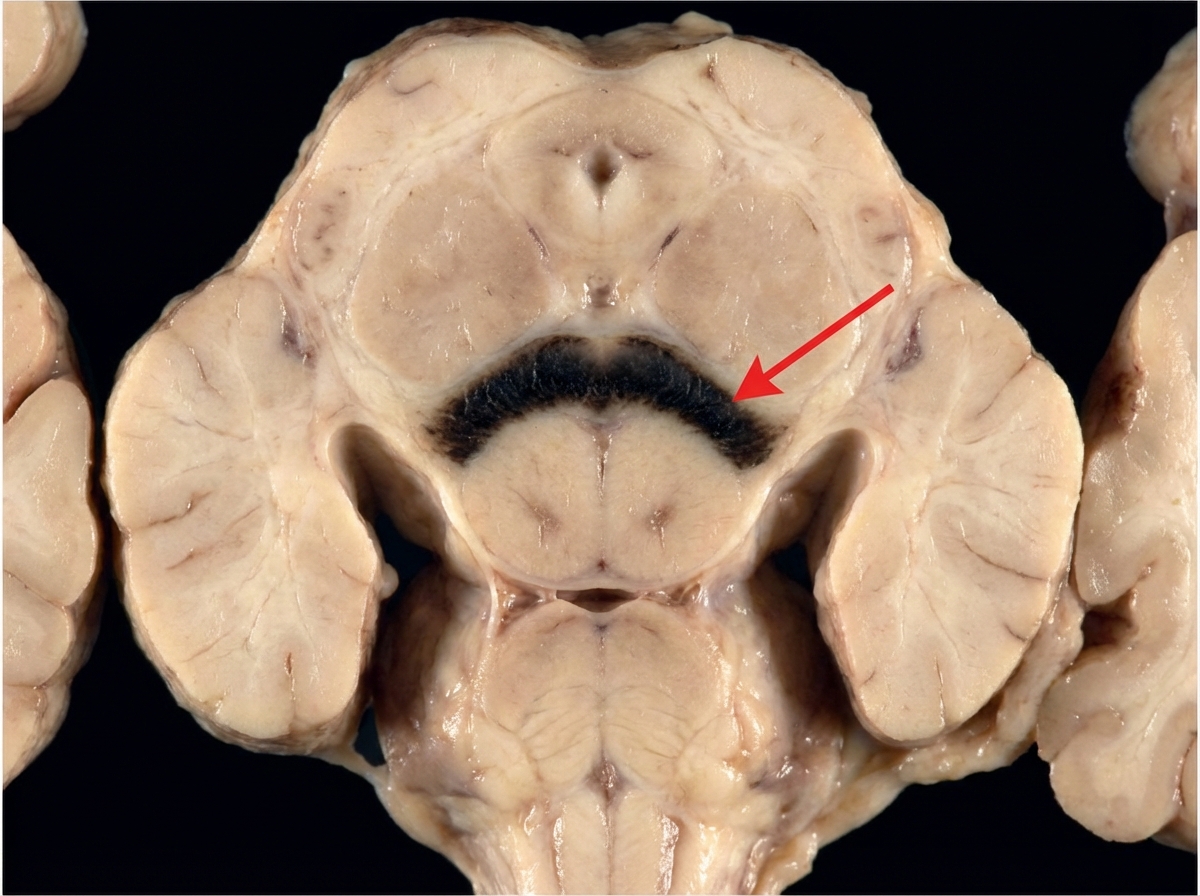
The marked structure is involved in which pathology?
A 58-year-old man is admitted to the emergency department with progressive unilateral hearing loss and ringing in the affected ear (tinnitus) of 4 months' duration. Radiographic examination reveals a tumor at the cerebellopontine angle. Which of the following nerves is most likely affected?
Which of the following is a derivative of the neural crest?
Increased expression of which of the following causes oncogenesis?
What are the first-order neurons of the anterior spinocerebellar tract?
All of the following cranial nerves pass through the middle part of the jugular foramen, except?
Practice by Chapter
Organization of the Nervous System
Practice Questions
Spinal Cord Anatomy
Practice Questions
Brainstem Anatomy
Practice Questions
Cerebellum
Practice Questions
Diencephalon
Practice Questions
Cerebral Cortex
Practice Questions
Basal Ganglia
Practice Questions
Limbic System
Practice Questions
Cranial Nerves
Practice Questions
Autonomic Nervous System
Practice Questions
Neural Pathways and Tracts
Practice Questions
Neurovascular Anatomy
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
