Neuroanatomy — MCQs

On this page
The gustatory nucleus is part of which of the following nuclei?
Corpora amylacea are found in which gland?
Meckel's diverticulum is a remnant of which embryonic structure?
Which ECG finding is indicative of hypercalcemia?
All of the following are tumor markers except?
In ICD-10 classification, what does the code F20 denote?
Which of the following is true for the receptor action of a drug?
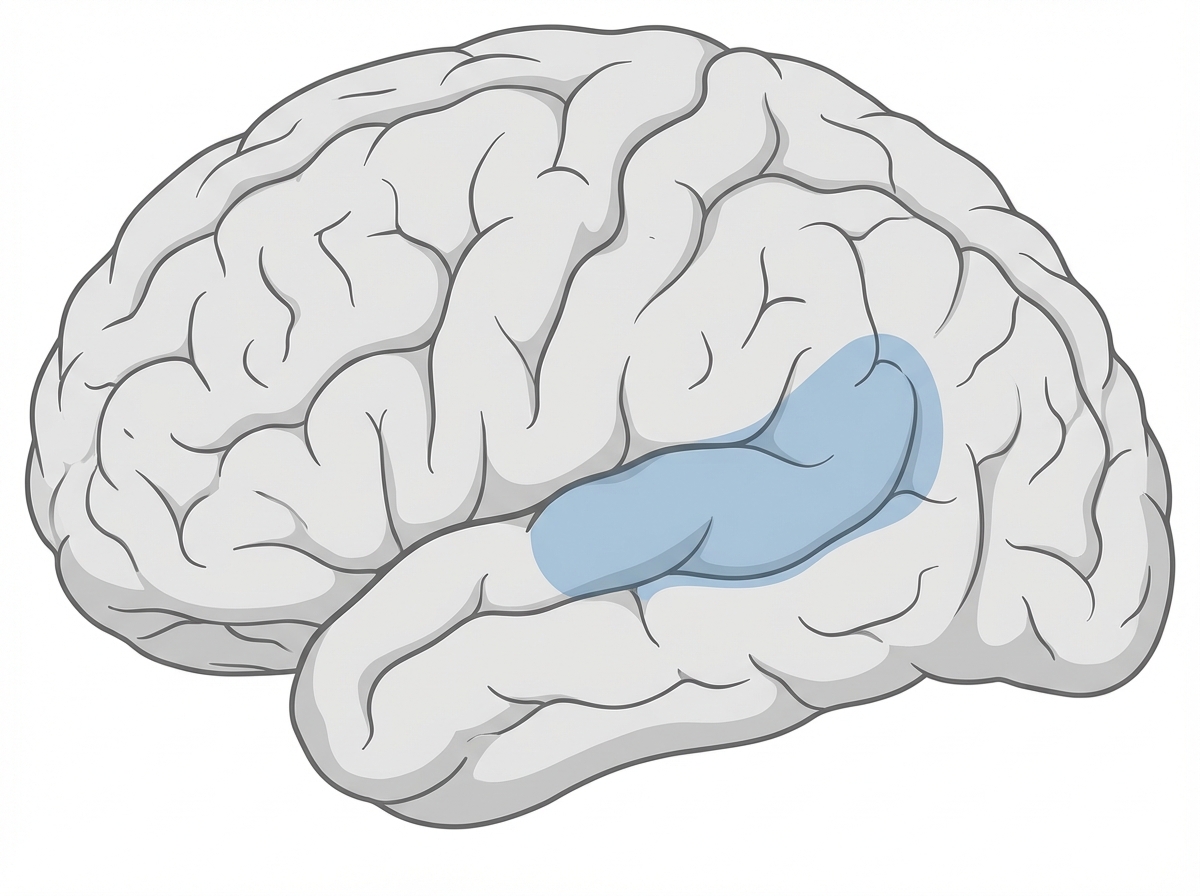
Which of the following is likely to be found in a patient with a lesion in the shaded area?
Failure of closure of the posterior neuropore causes what condition?
To which of the following thalamic nuclei do the spinothalamic fibers project?
Practice by Chapter
Organization of the Nervous System
Practice Questions
Spinal Cord Anatomy
Practice Questions
Brainstem Anatomy
Practice Questions
Cerebellum
Practice Questions
Diencephalon
Practice Questions
Cerebral Cortex
Practice Questions
Basal Ganglia
Practice Questions
Limbic System
Practice Questions
Cranial Nerves
Practice Questions
Autonomic Nervous System
Practice Questions
Neural Pathways and Tracts
Practice Questions
Neurovascular Anatomy
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
