Neuroanatomy — MCQs

On this page
All of the following types of interactions cooperate in stabilizing the tertiary structures of globular proteins except?
The renal parenchyma is derived embryologically from which structure?
Which branch of pharmacology deals with medicinal drugs obtained from plants and other natural resources?
Which of the following is NOT a characteristic feature of skeletal muscle?
A woman has undergone septic abortion with vegetation on the tricuspid valve. Where are emboli most likely to travel?
Troponin-T is preferable to CPK-MB in the diagnosis of acute myocardial infarction in all of the following situations except:
The covering of A is?
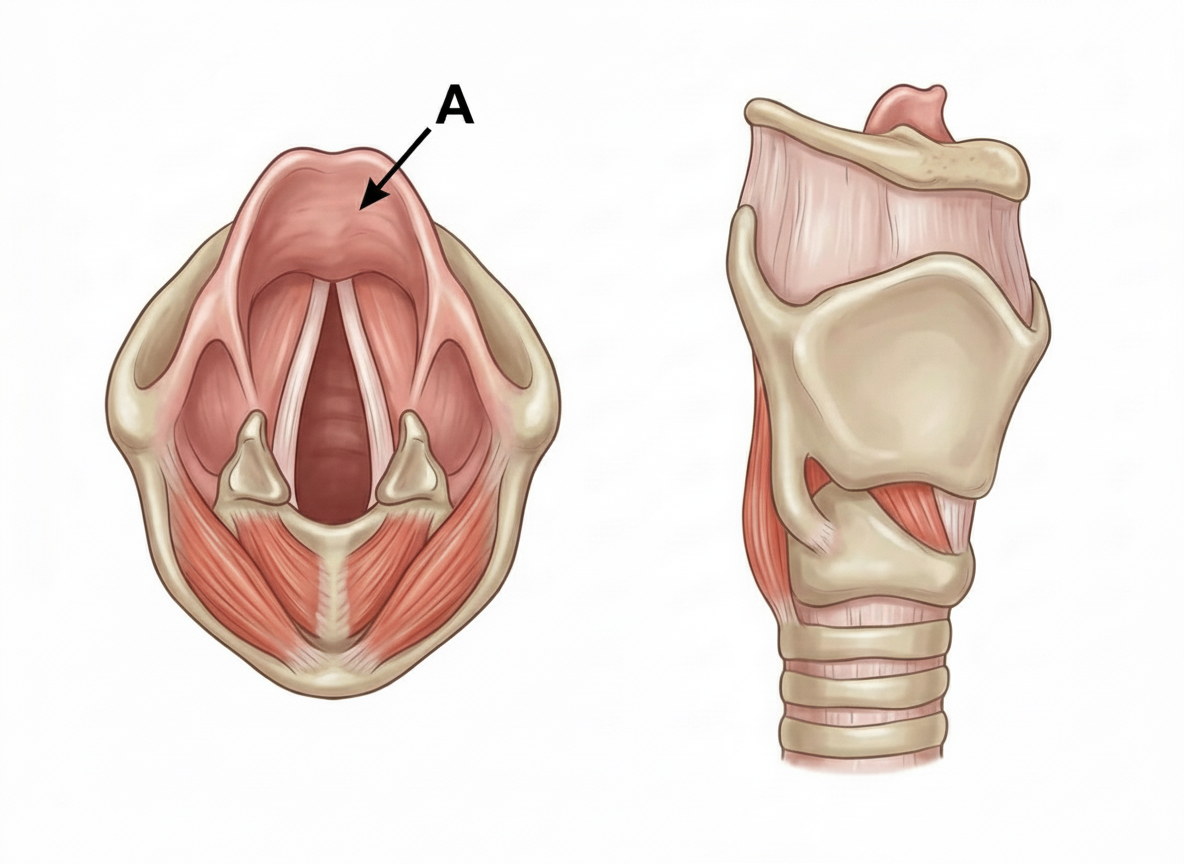
Titin is absent in which of the following?
Occlusion of the Artery of Adamkiewicz leads to infarction of which of the following structures?
What is the most effective method of treatment for digitalis toxicity?
Practice by Chapter
Organization of the Nervous System
Practice Questions
Spinal Cord Anatomy
Practice Questions
Brainstem Anatomy
Practice Questions
Cerebellum
Practice Questions
Diencephalon
Practice Questions
Cerebral Cortex
Practice Questions
Basal Ganglia
Practice Questions
Limbic System
Practice Questions
Cranial Nerves
Practice Questions
Autonomic Nervous System
Practice Questions
Neural Pathways and Tracts
Practice Questions
Neurovascular Anatomy
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
