Neuroanatomy — MCQs

On this page
A patient exhibiting signs of Horner's syndrome likely has a lesion in which part of the sympathetic nervous system?
Which nerve innervates the muscles of mastication?
A patient presents with an inability to abduct the eye. Which cranial nerve is most likely affected?
A 50-year-old male presents with unilateral ptosis, miosis, and anhidrosis. Which structure is most likely involved?
A neurologist is evaluating a patient with an altered sense of taste. Damage to which cranial nerve is most likely responsible for this symptom?
A patient experiencing vertigo and tinnitus may have pathology in which cranial nerve?
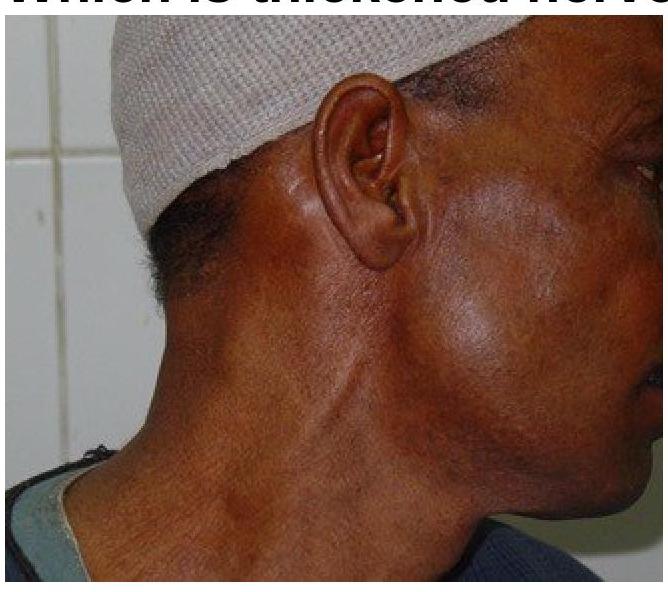
Which thickened nerve is shown in the image?
Which of the following is NOT a special visceral efferent (SVE) nerve?
HSV-2 causes latent infection in which nerve plexus/ ganglia ?
The optic nerve is formed by axons of which order neurons in the visual pathway?
Practice by Chapter
Organization of the Nervous System
Practice Questions
Spinal Cord Anatomy
Practice Questions
Brainstem Anatomy
Practice Questions
Cerebellum
Practice Questions
Diencephalon
Practice Questions
Cerebral Cortex
Practice Questions
Basal Ganglia
Practice Questions
Limbic System
Practice Questions
Cranial Nerves
Practice Questions
Autonomic Nervous System
Practice Questions
Neural Pathways and Tracts
Practice Questions
Neurovascular Anatomy
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
