Lower Limb — MCQs

On this page
Injury to which part causes difficulty in dorsiflexion of the foot?
Identify the bone indicated by the arrow in the image.
A surgical procedure is performed on the great saphenous vein, around 2.5 cm anterior to the medial malleolus. Which of the following structures is most likely to be injured?
What is the action of the muscle marked in the image?
Which muscles are supplied by the superficial peroneal nerve?
A patient presents with meralgia paresthetica. Based on the diagram, identify the nerve involved in this condition.
Which is correct about the markings shown on the left popliteal fossa? (Recent NEET Pattern 2016-17)

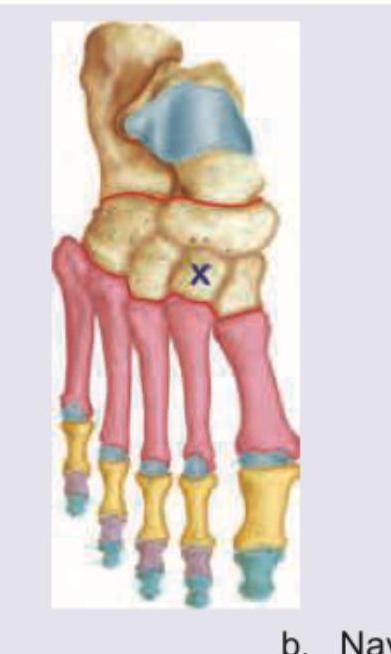
Identify the bone marked as X.
Femoral hernias are more common in females because :
Match List-I with List-II and select the correct answer using the code given below the Lists: (Refer to the image below for the lists)
Practice by Chapter
Gluteal Region and Hip
Practice Questions
Thigh and Popliteal Fossa
Practice Questions
Leg and Foot
Practice Questions
Joints of Lower Limb
Practice Questions
Nerves of Lower Limb
Practice Questions
Arterial Supply and Venous Drainage
Practice Questions
Lymphatic Drainage
Practice Questions
Muscles and Their Actions
Practice Questions
Gait Analysis and Biomechanics
Practice Questions
Applied Anatomy and Clinical Correlations
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
