Abdomen — MCQs

On this page
Which structure is held by forceps?
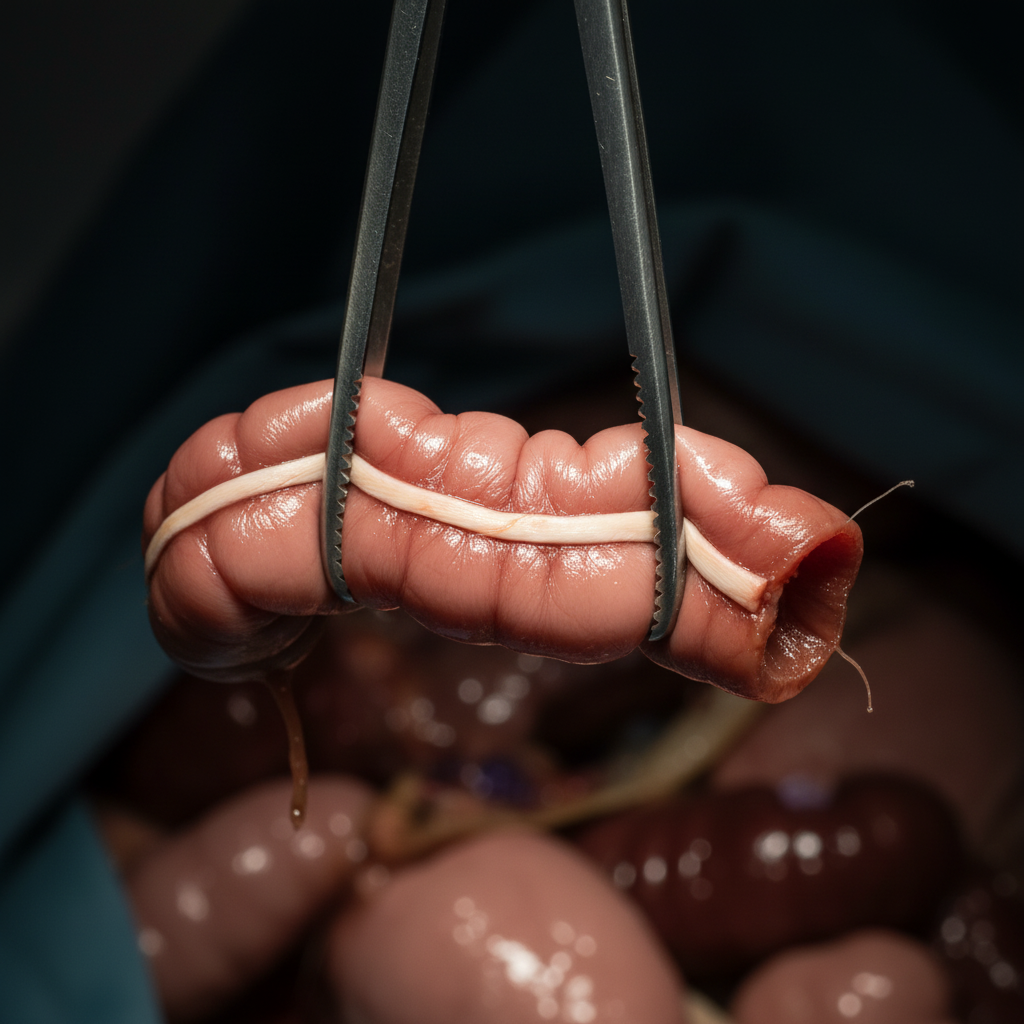
The cholecysto-venacaval line separates which of the following structures?
Which of the following is NOT true about the right kidney?
What is the length of the lower esophageal sphincter?
In a patient with compensated liver cirrhosis who presented with a history of variceal bleed, what is the treatment of choice?
A gallstone gets impacted most commonly in which part of the common bile duct?
Which artery is most commonly responsible for bleeding in duodenal ulcer hemorrhage?
All of the following are true regarding the blood supply to the kidney, EXCEPT?
The left renal vein crosses the aorta at which level?
A 20-year-old male presents with repeated episodes of hematemesis. There is no history of jaundice or liver decompensation. On examination, significant findings include splenomegaly (8 cm below the costal margin) and the presence of esophageal varices. There is no ascites or peptic ulceration. The liver function tests are normal. What is the most likely diagnosis?
Practice by Chapter
Anterior Abdominal Wall
Practice Questions
Peritoneum and Peritoneal Cavity
Practice Questions
Stomach and Intestines
Practice Questions
Liver, Gallbladder and Biliary Tract
Practice Questions
Pancreas and Spleen
Practice Questions
Kidneys and Suprarenal Glands
Practice Questions
Abdominal Vasculature
Practice Questions
Posterior Abdominal Wall
Practice Questions
Innervation of Abdominal Viscera
Practice Questions
Applied Anatomy and Clinical Correlations
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
