Abdomen — MCQs

On this page
Which of the following is a direct branch of the abdominal aorta?
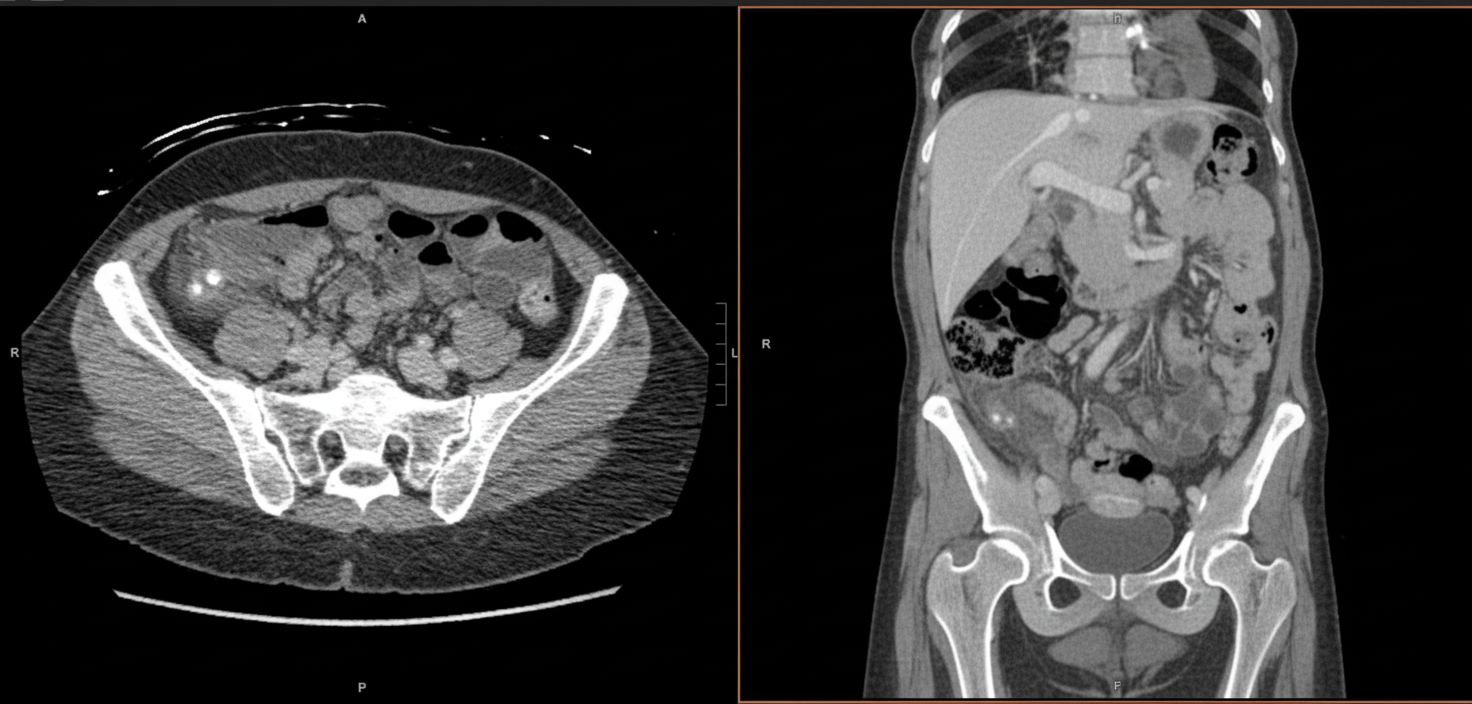
A 27-year-old woman presents with high fever and abdominal pain. Initially, the pain is around the navel but shifts to the right lower quadrant. A CT scan is provided. Which structure is affected?
The transverse mesocolon contains which of the following arteries?
All of the following statements regarding the adrenal gland are true except?
A 32-year-old man presents with a painless mass in his right scrotum of several months' duration. Ultrasonography shows a homogeneous hypoechoic intratesticular mass. Biopsy reveals a seminoma. To which of the following lymph nodes does cancer of the testis first metastasize?
The floor of the inguinal canal is formed by which of the following structures?
Ligation of the coeliac artery mostly affects all of the following organs except:
Porto-caval anastomosis is seen between which of the following anatomical locations?
What is true about splenunculi?
A patient was admitted with symptoms of bowel obstruction. Further examination revealed that the obstruction was caused by the nutcracker-like compression of the bowel between the superior mesenteric artery and the aorta. The compressed bowel is MOST likely to be:
Practice by Chapter
Anterior Abdominal Wall
Practice Questions
Peritoneum and Peritoneal Cavity
Practice Questions
Stomach and Intestines
Practice Questions
Liver, Gallbladder and Biliary Tract
Practice Questions
Pancreas and Spleen
Practice Questions
Kidneys and Suprarenal Glands
Practice Questions
Abdominal Vasculature
Practice Questions
Posterior Abdominal Wall
Practice Questions
Innervation of Abdominal Viscera
Practice Questions
Applied Anatomy and Clinical Correlations
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
