Abdomen — MCQs

On this page
The renal collar, which surrounds the aorta, has its two limbs split by which structure?
In lumbar sympathectomy, which root value is spared?
A patient presents with pain in the right testis. Examination reveals a 'bag of worms' appearance, suggestive of a varicocele. Into which vessel does the right testicular vein drain?
Which structures are injured during resection of the free edge of the lesser omentum?
Which anatomical space is described as the sub-diaphragmatic right posterior intraperitoneal space?
The cecum is found to be placed below the stomach and is midline. Which of the following abnormalities must have taken place during the rotation of the gut?
Which of the following is a content of Calot's triangle?
A 29-year-old man presents with duodenal peptic ulcer and complains of cramping epigastric pain. Which of the following structures harbors the cell bodies of abdominal pain fibers?
Where are Peyer's patches located in the gastrointestinal tract?
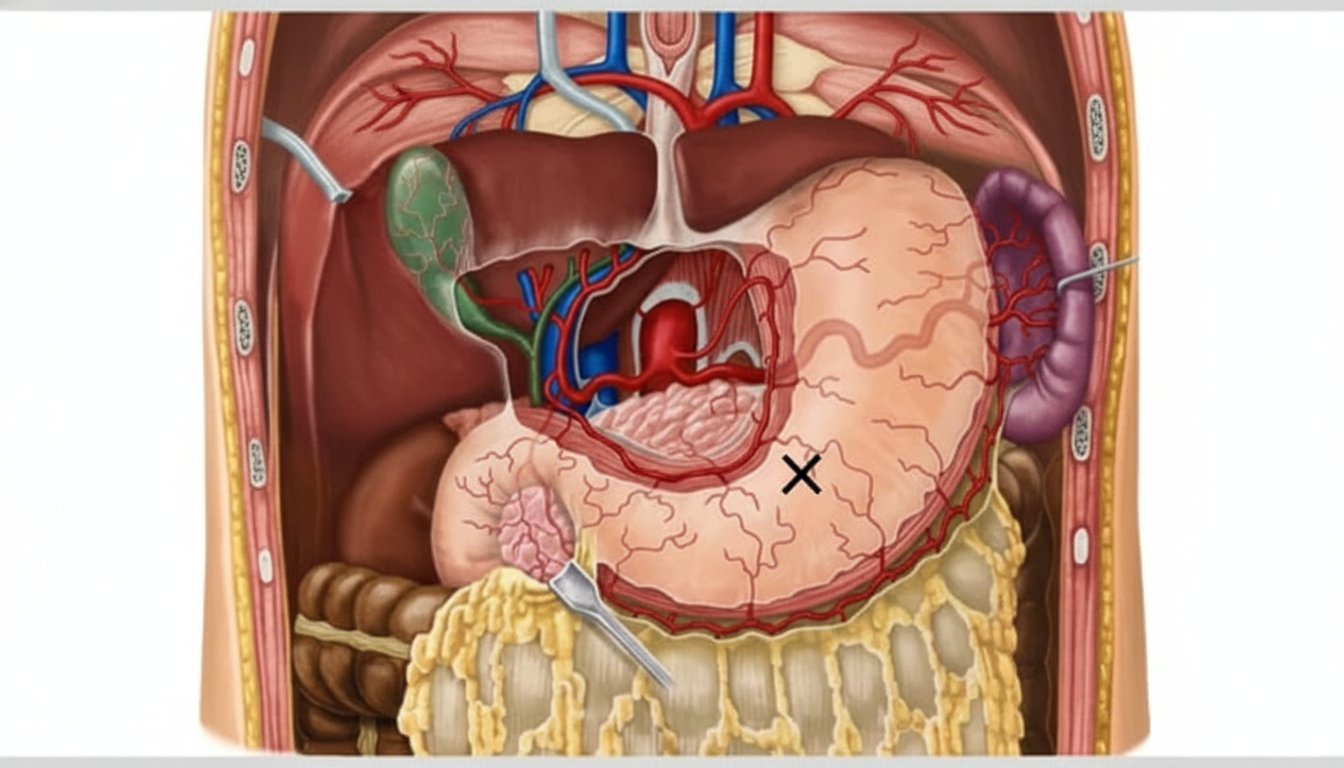
The artery marked X is most commonly a branch of?
Practice by Chapter
Anterior Abdominal Wall
Practice Questions
Peritoneum and Peritoneal Cavity
Practice Questions
Stomach and Intestines
Practice Questions
Liver, Gallbladder and Biliary Tract
Practice Questions
Pancreas and Spleen
Practice Questions
Kidneys and Suprarenal Glands
Practice Questions
Abdominal Vasculature
Practice Questions
Posterior Abdominal Wall
Practice Questions
Innervation of Abdominal Viscera
Practice Questions
Applied Anatomy and Clinical Correlations
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
