Abdomen — MCQs

On this page
Which of the following statements about the third part of the duodenum is untrue?
What is the approximate length of the large intestine?
The gastrosplenic ligament is a peritoneal reflection surrounding which artery?
Which of the following are the main sources of blood supply to the stomach?
The Meckel's diverticulum is situated within about how many cm from the ileocecal valve?
Which of the following statements about Brunner's glands is FALSE?
The cardiac orifice of the stomach is located at the level of which vertebra?
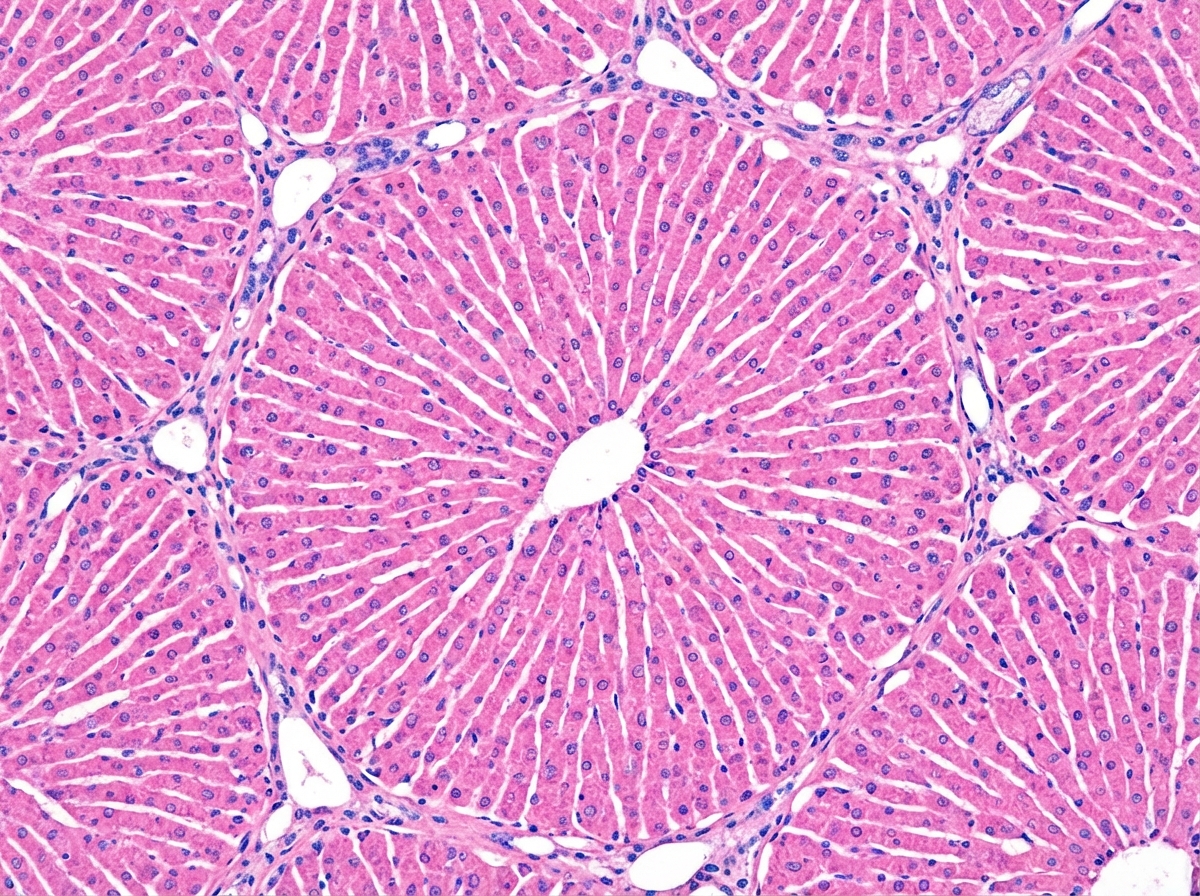
What is the predominant source of blood supply to the organ shown in the histological slide?
Which nerve is known as the criminal nerve of Grassi?
Gall bladder is lined by which type of epithelium?
Practice by Chapter
Anterior Abdominal Wall
Practice Questions
Peritoneum and Peritoneal Cavity
Practice Questions
Stomach and Intestines
Practice Questions
Liver, Gallbladder and Biliary Tract
Practice Questions
Pancreas and Spleen
Practice Questions
Kidneys and Suprarenal Glands
Practice Questions
Abdominal Vasculature
Practice Questions
Posterior Abdominal Wall
Practice Questions
Innervation of Abdominal Viscera
Practice Questions
Applied Anatomy and Clinical Correlations
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
