A primigravida in her 10th week of gestation presents with spotting. On examination, the uterus corresponds to 12 weeks. Transvaginal ultrasound was done and it is given below. What is your diagnosis?
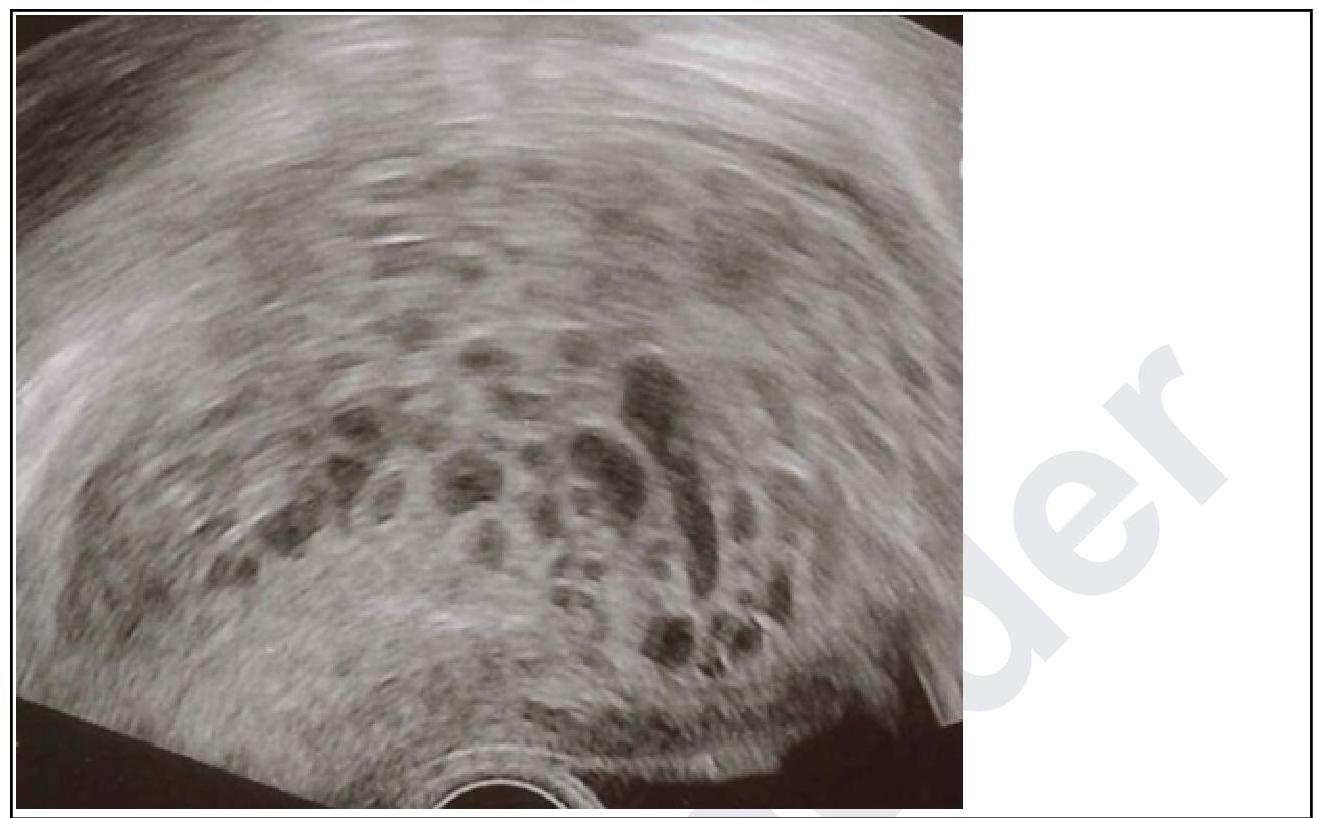
A primigravida is in labor. Her per-vaginal examination revealed a posterior cervix with 5 cm cervical length, 1 cm dilatation, soft consistency, and head at -1 station. Calculate the Bishop score.