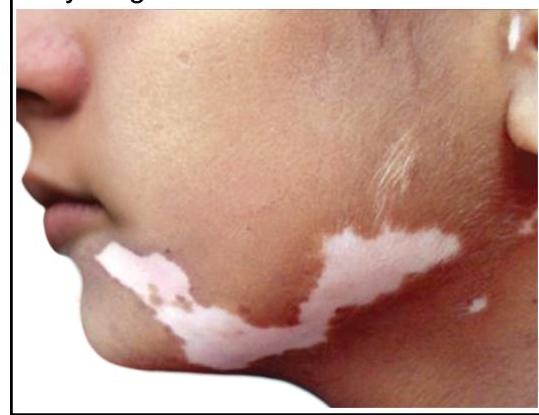
A young girl presents with leukotrichia and lesions as shown in the image. What is the most likely diagnosis?
A child presented with itchy plaques over the neck, the bilateral popliteal and cubital fossa. What could be the diagnosis?
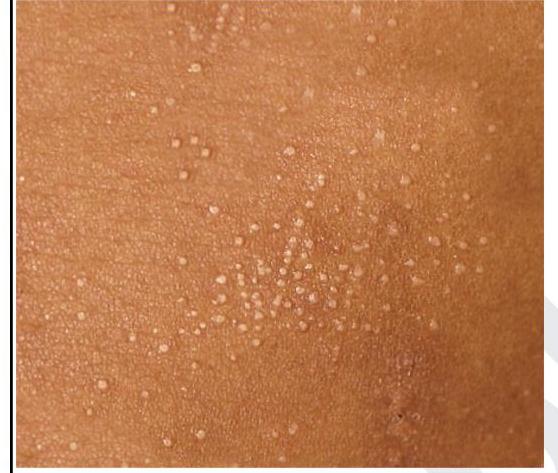
A child presented with asymptomatic lesions on the forearm and on the shaft of the penis. The lesions on the forearm are shown below. What is the most likely diagnosis?